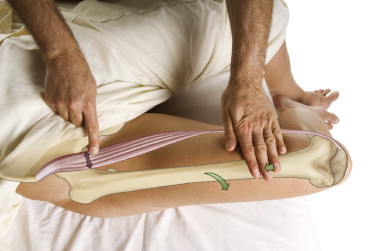
Signs and symptoms:
Compression of a sensory nerve can decrease its transmission, causing altered sensitivity, in other words paresthesia. Paresthesia can be divided into decreased sensitivity, termed hypesthesia, and increased sensitivity, termed hyperesthesia. Compression of a nerve can block or partially block nerve transmission causing hypesthesia such as numbness; or it can irritate the nerve causing increased transmission or aberrant signals resulting in increased sensitivity to touch or pain. Therefore, meralgia paresthetica can present with lateral thigh pain, tingling, numbness or other altered sensation in the lateral thigh.
Assessment/Diagnosis:
Meralgia paresthetica is primarily assessed/diagnosed by its clinical presentation of the client/patient reporting pain or other paresthesia in the lateral thigh. The therapist can determine the region of altered sensation using a pinwheel (in place of a pinwheel, another object such as the tip of a pen cap can be used). Lightly run the pinwheel along the surface of the skin of the client’s/patient’s thigh on each side of the body, comparing what they feel from one side to the other. In this manner, the region of paresthesia can be mapped and compared to the dermatomal innervation pattern for the lateral femoral cutaneous nerve.
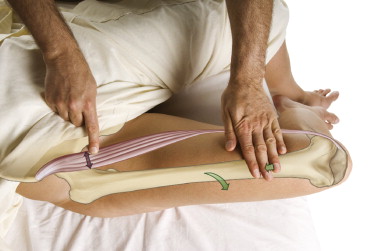
Palpation of the sartorius muscle. The thigh is laterally rotated at the hip joint and then flexed against resistance. Permission: Joseph E. Muscolino. The Muscle and Bone Palpation Manual, with Trigger Points, Referral Patterns, and Stretching, 2ed. (2016) Elsevier.
Moderate to deep palpatory pressure can be placed along the inguinal ligament near the anterior superior iliac spine (ASIS). In more severe cases, this pressure might reproduce or increase the characteristic sensory referral pattern that the client/patient has been experiencing, confirming the assessment of meralgia paresthetica. Palpatory assessment of the sartorius or tensor fasciae latae (TFL) and surrounding hip flexor musculature, including the abdominal belly of the psoas major, as well as the quadratus lumborum should also be done in the event that tight musculature is pressing on the nerve. Palpate also for fascial adhesions that might be pressing on the nerve.
During verbal history, it is important to determine if any of the causative stress factors (see other blog article on this condition) for meralgia paresthetica are present. Finally, the assessment of meralgia paresthetica is somewhat an assessment/diagnosis of exclusion, meaning that if all other conditions that can cause pain or altered sensation in the lateral thigh are assessed for and ruled out, the assessment of meralgia paresthetica can be made with a high degree of confidence.
Note: A physician can order electrophysiologic testing in which conduction of the lateral femoral cutaneous nerve is assessed. This is not often done, but is the most accurate way to diagnose meralgia paresthetica.
Differential assessment:
Because meralgia paresthetica is largely an assessment of exclusion, it is important to be sure that the client’s/patient’s symptoms are not due to another condition. In addition to the lateral femoral cutaneous nerve, there are three other nerves that provide sensory innervation to the thigh. They are the posterior femoral cutaneous nerve in the posterior thigh, the femoral nerve in the anterior thigh, and the obturator nerve in the medial thigh.
Pain or other paresthesia in the lateral thigh can also be due to referral from a myofascial trigger point. The following muscles should be assessed for trigger points: gluteus minimus, vastus lateralis, vastus intermedius, tensor fasciae latae, piriformis, and gluteus maximus and medius. It is also possible that the nerve roots that comprise the lateral femoral cutaneous nerve are being compressed at the spine due to a space-occupying lesion such as a pathologic disc or bone spur narrowing the intervertebral foramen (IVF) or central canal of the spinal column; this can be assessed via cough test or Valsalva maneuver (or perhaps straight leg raise), or diagnosed by an MRI ordered by a physician. And finally, the lateral thigh itself should be examined to rule out any local condition that might be causing lateral thigh pain/paresthesia.