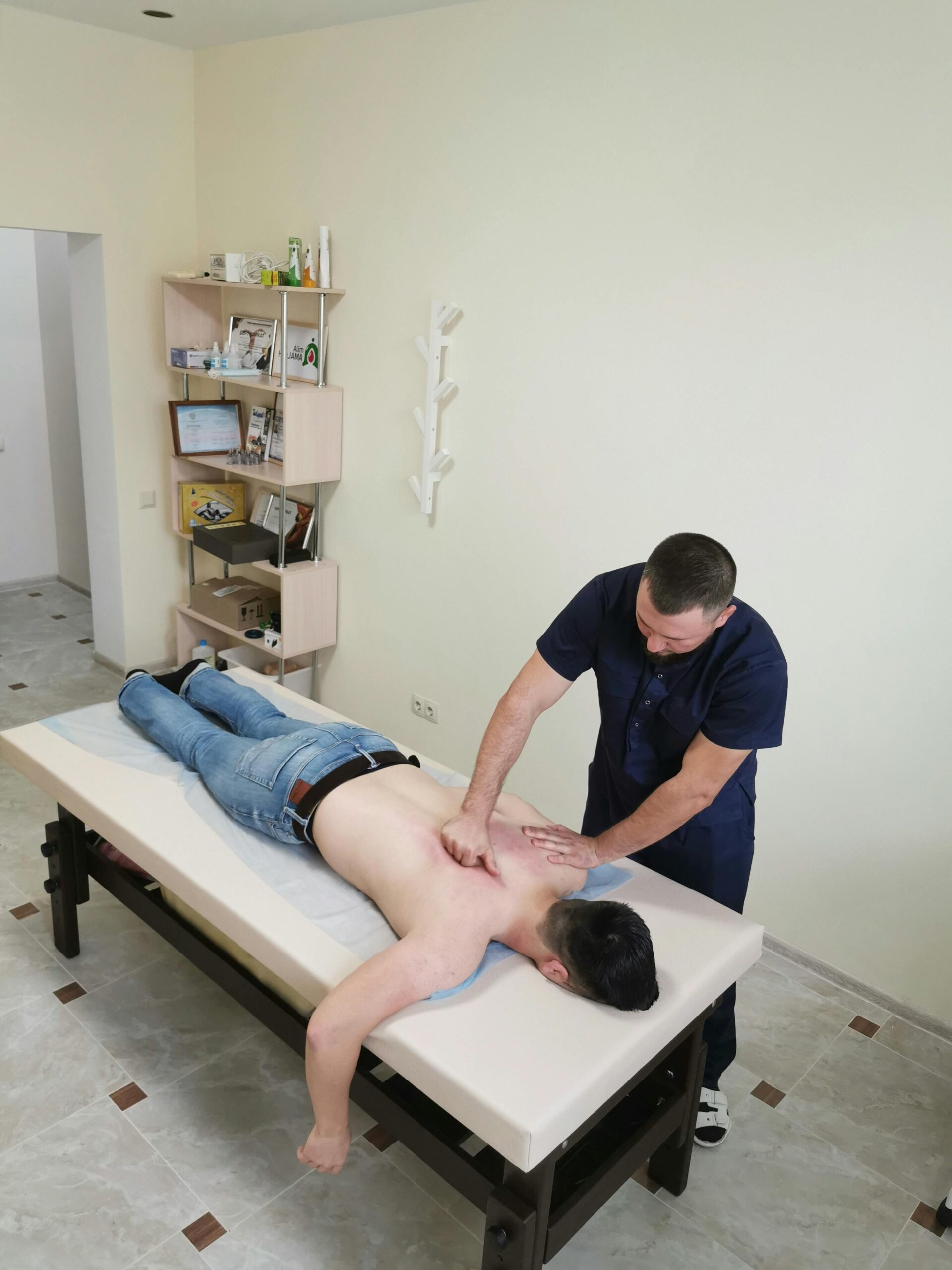
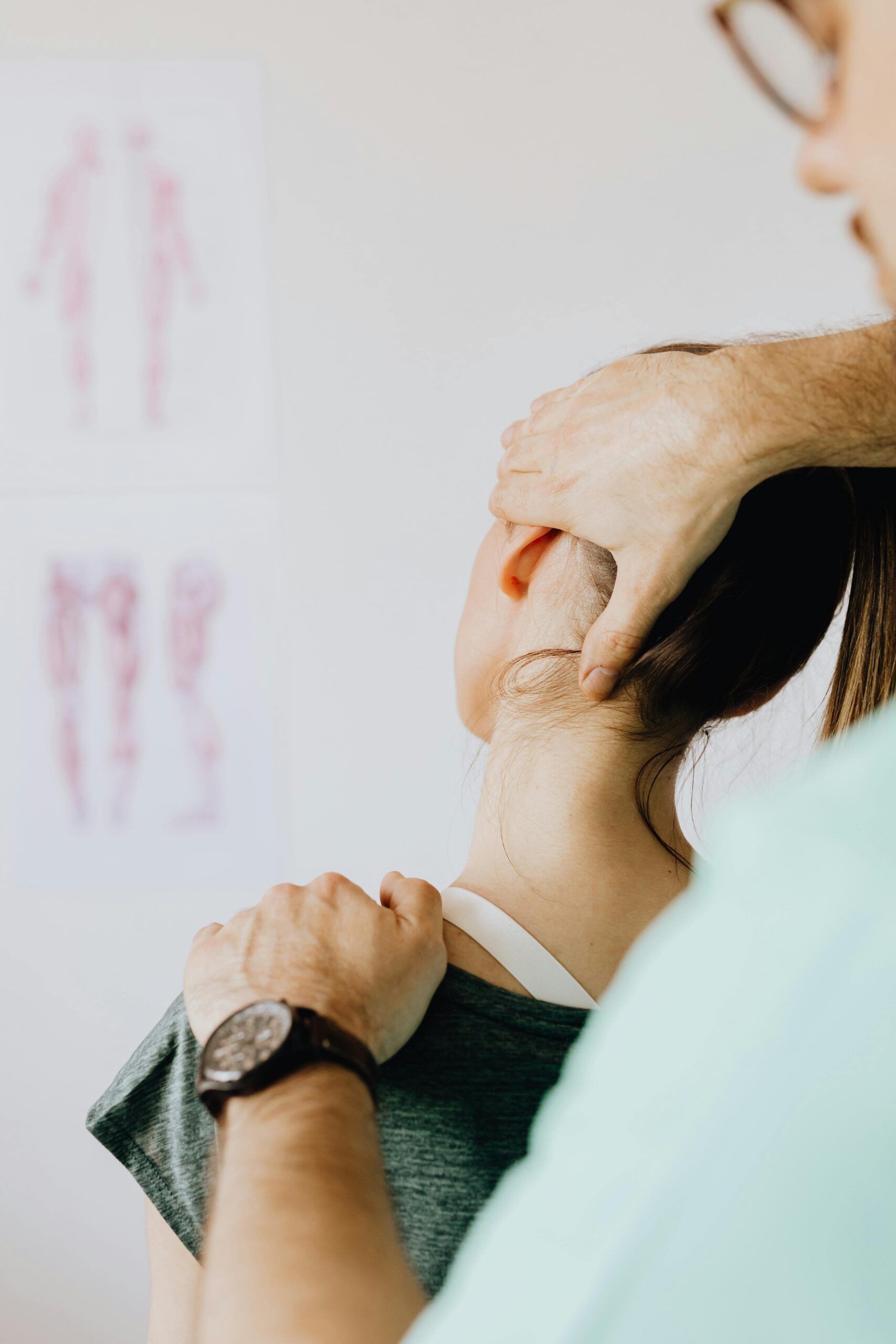
Self-care for whiplash injuries is not merely rest. It’s intelligent movement, proper support, and long-term ergonomic awareness. As an occupational therapist, physical therapist, or caregiver, your hands can do wonders in creating a recovery-facilitative environment where recovery is done at home.
From buying hospital beds and recuperative pillows to installing supportive equipment and making environmental adjustments, creating a recovery-aided setup can reduce strain, enhance healing, and alleviate pain.
This guide discusses functional equipment, arrangements, and rehabilitation routines that therapists can recommend for the effective and safe treatment of acute neck strain or cervical trauma in clients.
Understanding the Basics of Whiplash and Cervical Strain
Whiplash occurs when the neck is unexpectedly flexed and then extended, most commonly after car wrecks, falls, or athletics. This abrupt movement may cause the soft tissues of the neck to strain, resulting in stiffness, pain, headaches, tiredness, and limited mobility.
It is important to spot and treat these symptoms early on, even if they seem insignificant. Delayed treatment can lead to recurring issues such as chronic pain or reduced range of motion. This is why it is important to teach clients about early signs and proper maintenance. Self-care for whiplash injuries begins with body awareness. Practitioners can educate themselves further on the muscle groups involved in cervical strain.
A wonderful source for this is the Muscle Anatomy Master Class. This training module instructs practitioners regarding the profound muscular functions and dysfunctions of the spine and neck. Clients who are recovering at home need assistance that connects what they learn in therapy to their daily lives. That means attention not just to exercises but also to how their living situation and daily routines affect their healing.
The Role of the Environment in Neck and Spine Recovery
Recovery needs to minimize physical stress and promote proper positioning. In the case of spine and neck injuries, this involves ergonomic support and rest therapy. Start with sleep. It’s the most overlooked aspect of recovering from injury, but one of the most vital.
Have clients tilt their heads slightly, employ a cervical support pillow, and avoid sleeping positions that flex the neck. Adaptable sleeping arrangements are lifesavers for individuals with extreme pain or compromised mobility. That’s where hospital beds can help. Unlike your run-of-the-mill bed, hospital beds can vary the head and foot levels to a certain degree of accuracy to reduce pressure and keep the spine straight while sleeping.
For clients who need to use long-term care at home, you can recommend that they buy hospital beds with therapeutic positioning features, simple controls, and optional side rails for safety. Other things your client will need are:
- Quiet and uncluttered room to maximize comfort.
- Blackout curtains to encourage high-quality, uninterrupted sleep.
- Frequently used items within easy reach to avoid unnecessary neck movements.
All these adjustments as a whole can have a significant impact on your clients’ everyday experience.
Recommended Recovery Tools and At-Home Adjustments
Aside from the bed, the right equipment may assist with comfort, promote healing, and avoid reinjury. Some of the most frequently suggested items by professionals are:
- Cervical pillows: These support the natural curve of the neck and reduce pressure at night.
- Neck braces (soft collars): Most useful applied short term following acute trauma to restrict motion as tissues heal.
- Hot and cold therapy: Heat pads assist with muscle stiffness, while ice packs inhibit inflammation during flare-ups.
- Posture supports: Wearable braces or straps help patients to keep a healthy shoulder and spine position for extended periods.
For clients who work from home, the environment setup is also important. Recommend that they:
- Use an adjustable chair that adjusts to accommodate the clients’ lower back.
- Place computer monitors at eye level, and use a pile of books as a monitor riser if needed.
- Use a phone stand to prevent smartphone use by being stared at downward for hours on end.
These adjustments can help the client’s body heal from the whiplash injury by reducing bad habits that disrupt recovery or exacerbate symptoms.
Customize your recommendations to the extent of injury. A client with mild whiplash may need only a pillow and modified workspace arrangement, whereas a client with moderate to severe strain may require a complete home ergonomic transformation.
Gentle Movement, Massage, and Pain Management Tips
While rest is key during the acute phase, controlled motion, when done cautiously, is also important in healing.
Begin by letting your client try these limited range-of-motion exercises (after only medical authorization):
- Tilt head back to neck to align spine, slowly tucking the chin in.
- Tilt head from side to side slowly to release tension.
- Roll shoulders to loosen the upper back and trap tension.
Massage therapists treating whiplash clients have to be cautious and follow these guidelines:
- Start with gentle pressure and brief sessions.
- Massage adjacent muscle groups (such as the upper back and shoulders) before direct neck massage.
- Speak often with the client regarding pain sensitivity and boundaries, and adjust accordingly.
To help alleviate pain at home, consider recommending:
- TENS units: Low-voltage, small electrical devices that block pain signals.
- Topical creams: Menthol, arnica, or capsaicin-containing products that provide relief from within.
- Ice or heat packs: These are still quick and simple methods to control symptoms between appointments.
Combining these treatments with adequate rest can help your client recover faster and achieve range of motion sooner.
Educating Clients on Long-Term Self-Care and Prevention
Recovery is not just about removing the pain—it’s about good habits and regular movement. Professionals must help clients return to regular routines progressively by:
- Pacing physical tasks such as lifting or driving.
- Setting reminder alarms so that clients remember to stand up and stretch throughout the day at work.
- Working in good lifting habits: lift legs, keep back straight, and no sudden jerks.
Posture awareness every day is also essential. Get clients to:
- Sit with ears aligned over their shoulders, not too far forward or back
- Answer phone calls on speaker or use wireless earbuds rather than holding the phone to their neck and shoulder.
- Use footrests and lumbar pillows to support their whole spinal alignment, not just the neck.
Follow-ups are crucial, so you should schedule regular follow-up checks on clients’ progress and adjust the home setup or daily regimes accordingly. The tools and techniques that were successful in week one may be replaced or enhanced as recovery goes on.

Conclusion
Client recovery from neck and spine injuries is as much a matter of daily routine and life as it is of their treatment in the clinic. For this reason, therapists and medical professionals have a crucial influence on both aspects of the recovery process. By prescribing treatment settings like cervical pillows, adjustable beds, and posture support, you help clients to decrease bodily tension and improve daily function.
Using hospital beds is one optimal method of promoting higher-quality sleep and comfort at home for moderate to high-risk injured patients. Above all, keep in mind that whiplash injury self-care is a guided process for your client. Your assistance can help them avoid long-term complications, promote healing, and slowly gain control of the day-to-day responsibilities of their recovery process.
Written by lawanda@chulasmart.com