
All images are copyright-free and were created by Muqaddas Mehak using Ideogram AI
In manual therapy and movement-based practices, posture and breath are foundational elements. As clinicians, we analyze respiratory patterns, rib cage mobility, and diaphragmatic function to improve musculoskeletal health. But one often-overlooked factor that can meaningfully impact both posture and breath mechanics is chronic allergies, particularly allergic rhinitis.
Although typically framed as a seasonal nuisance, allergies can be a year-round driver of compensatory breathing and musculoskeletal dysfunction, making them highly relevant in clinical assessment and care planning.
Allergies and Breathing: More Than Just a Runny Nose

Chronic allergic rhinitis affects an estimated 15-30% of the global population. Characterized by nasal congestion, sneezing, postnasal drip, and sinus pressure, this condition frequently leads to mouth breathing, particularly at night or during exertion.
Mouth breathing bypasses the nasal passage’s natural filtering and humidifying functions. It can lead to:
- Reduced diaphragmatic engagement
- Shallow, apical breathing patterns
- Impaired thoraco-abdominal pressure regulation
Over time, these patterns contribute to altered motor control of the thorax and neck, increased muscular tension, and restricted rib cage excursion. Clinically, this often presents as tension-type headaches, myofascial trigger points, and decreased rib mobility, particularly in the posterior costo-vertebral region.
Postural Adaptations: How the Body Compensates
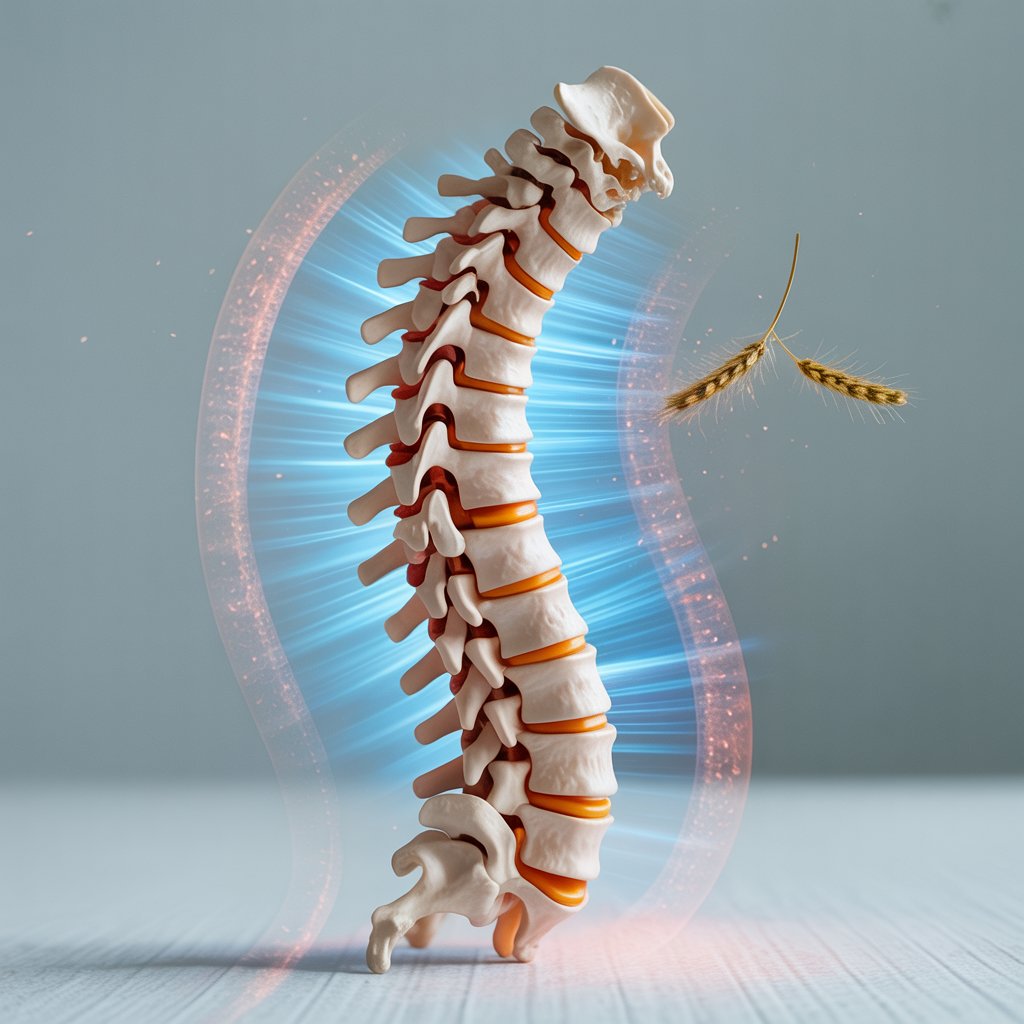
Persistent upper airway obstruction due to allergies can lead to a recognizable set of postural changes, including:
- Cervical protraction and upper cervical extension (classic “forward head posture”)
- Thoracic hyperkyphosis, reducing posterior rib mobility
- Scapular protraction, contributing to shoulder dysfunction
- Altered lumbopelvic alignment due to kinetic chain compensation
These patterns often mirror what’s described in Janda’s Upper Crossed Syndrome.
Research shows that chronic mouth breathing, especially during developmental years, can influence craniofacial structure, mandibular positioning, and upper airway space. In adults, compensations become more muscular and postural than skeletal, but still significantly affect breathing efficiency and biomechanics.
Manual Therapy: Effective, but Incomplete Without Root Cause Resolution
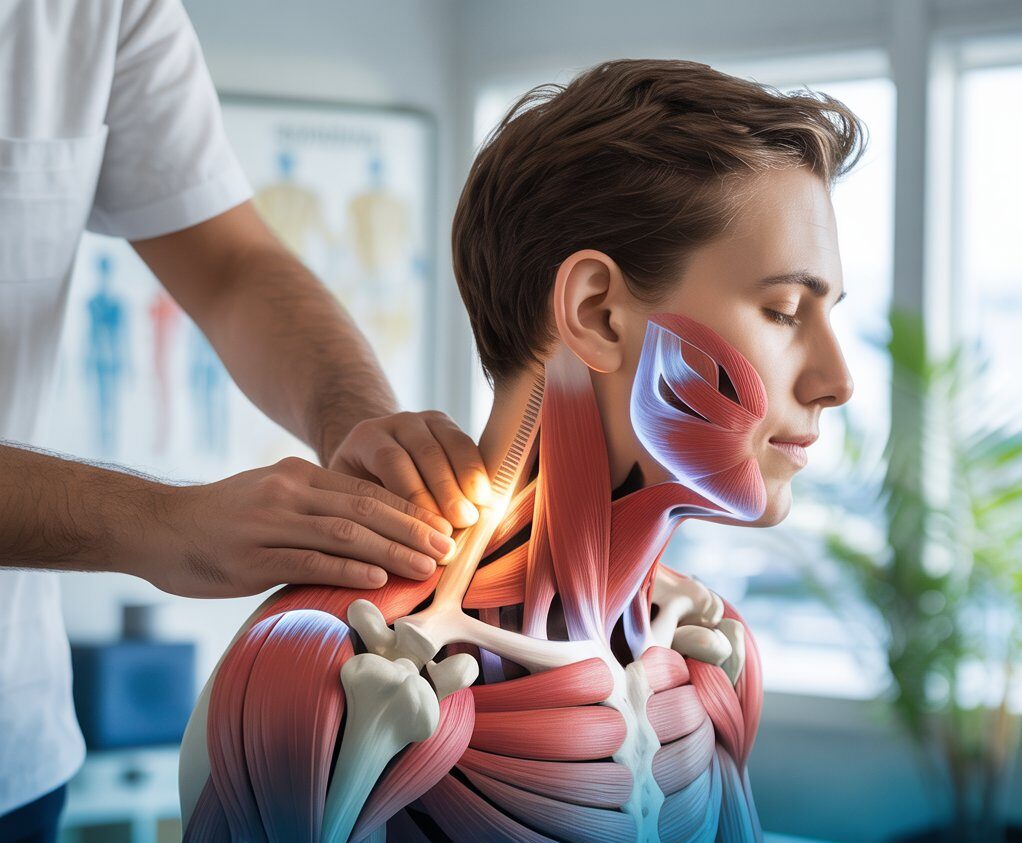
Manual therapy and movement re-education can effectively:
- Mobilize the costovertebral joints
- Release overactive (e.g., SCM, upper traps)
- Support diaphragmatic and nasal breathing
- Improve craniovertebral alignment
However, without addressing the underlying allergic congestion, clients will often relapse into dysfunctional breathing and postural habits. This makes treating the root cause, not just the compensation, crucial.
Immunotherapy: Addressing the Source of Dysfunction

Conventional medications like antihistamines and corticosteroid sprays offer symptom relief but do not retrain the immune system. That’s where allergy immunotherapy becomes a valuable long-term intervention.
There are two primary types: sublingual and subcutaneous immunotherapy.
Sublingual immunotherapy, often called allergy drops, involves drops or tablets taken daily under the tongue. They’re especially convenient for individuals managing environmental allergies like pollen, dust mites, or pet dander. They are FDA-approved for certain allergens and are gaining popularity for their at-home accessibility and safety profile.
Subcutaneous immunotherapy, often referred to as allergy shots, involves injections administered underneath the skin. These are administered in a clinical setting at regular intervals, typically over a 3–5 year treatment period. They are considered the gold standard for long-term allergy management, particularly for patients with multiple environmental allergens.
Both methods work by gradually exposing the immune system to controlled doses of allergens, building tolerance and reducing hypersensitivity over time. According to the Mayo Clinic, immunotherapy can lead to significant reductions in symptoms, improved sleep, and decreased reliance on medications.
How Clinicians Can Spot the Allergy-Posture Connection

As manual and movement therapists, we are well-positioned to identify clinical presentations that may reflect underlying respiratory or immune-related dysfunction. Although allergies are not within our direct scope to diagnose, we can recognize biomechanical patterns that suggest further evaluation may be warranted.
Be attentive to signs such as:
- Chronic mouth breathing, particularly during rest or sleep
- Cervical protraction with upper cervical extension that resists postural correction
- Persistent hypertonicity in the scalenes, sternocleidomastoid, and upper trapezius
- Client-reported symptoms such as nasal congestion, sinus pressure, fatigue, or non-restorative sleep
These patterns may reflect compensatory adaptations to impaired nasal airflow and dysfunctional breathing mechanics, often driven by allergic rhinitis or other inflammatory airway conditions.
Look Beyond the Table
Effective posture correction goes beyond biomechanics. Chronic allergies and immune stress can be hidden drivers of breathing dysfunction, compensatory posture, and recurring musculoskeletal complaints.
By looking through both a structural and immune lens, and understanding options like allergy immunotherapy, clinicians can help clients not just move better, but breathe better.
Author Bio
This article was written for Learnmuscles by Holly Clark, who has been working in the care industry for 5+ years as a project coordinator. She regularly blogs about both the personal and practical challenges of caring and is always actively working on producing informative content.

