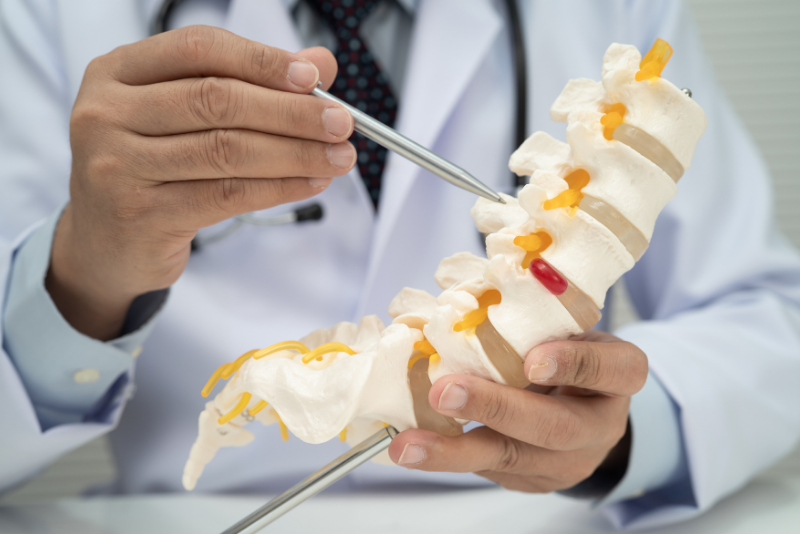
Yes — and the mechanism runs through the spinal cord’s blood supply just as much as it runs through mechanical compression.
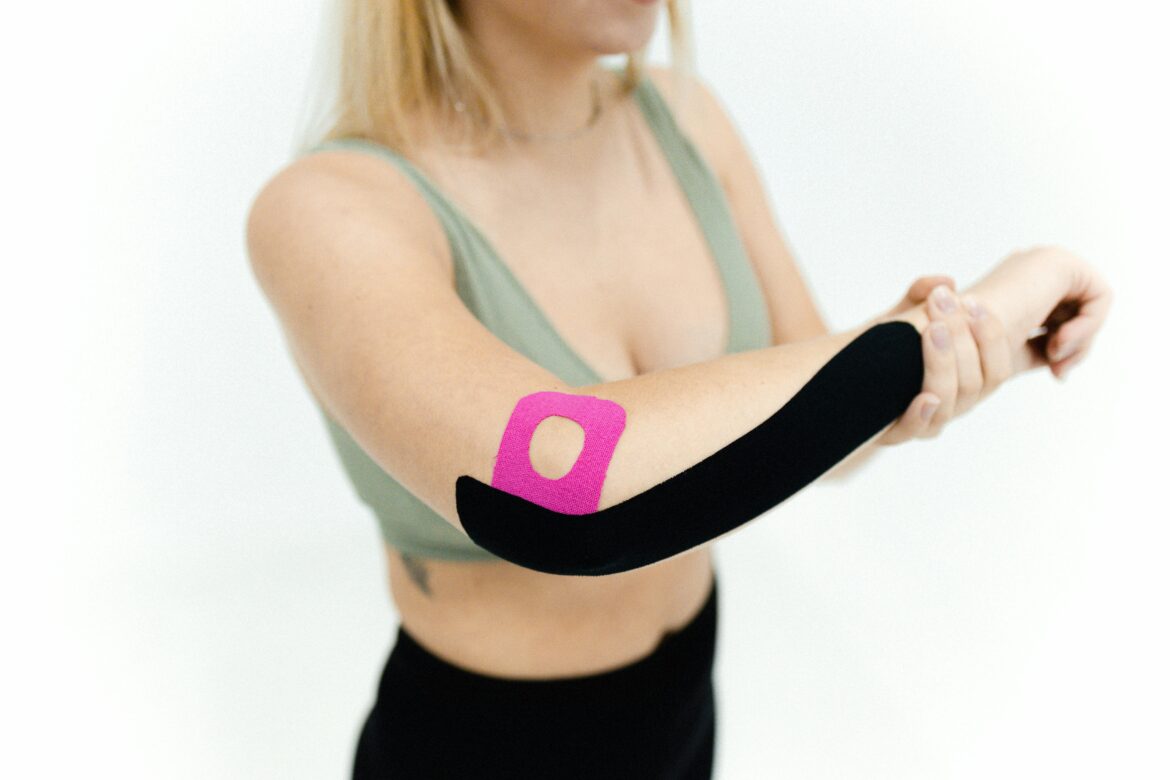
Understanding How Repetitive Arm Movements Can Lead to Chronic Elbow Damage
Whether the strain comes from sports, physical labor, office work, or repetitive exercise routines, repeated stress on the elbow can gradually damage tendons, muscles, and joint structures over time.
Massage Therapy Continuing Education
The value of massage therapy continuing education is often dependent on learning how to apply fundamental skill sets of manual therapy.
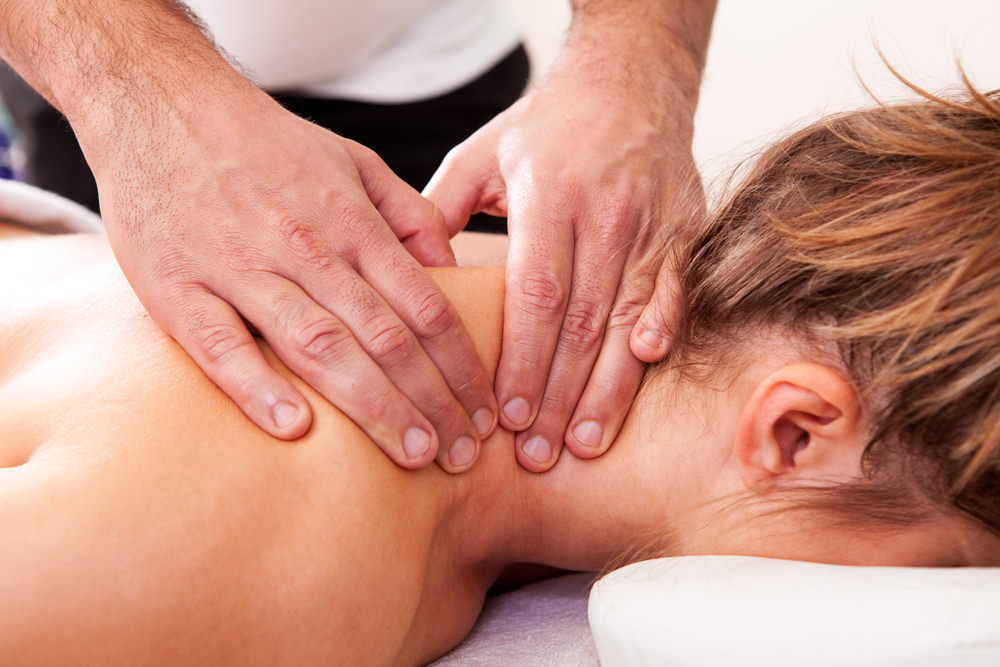
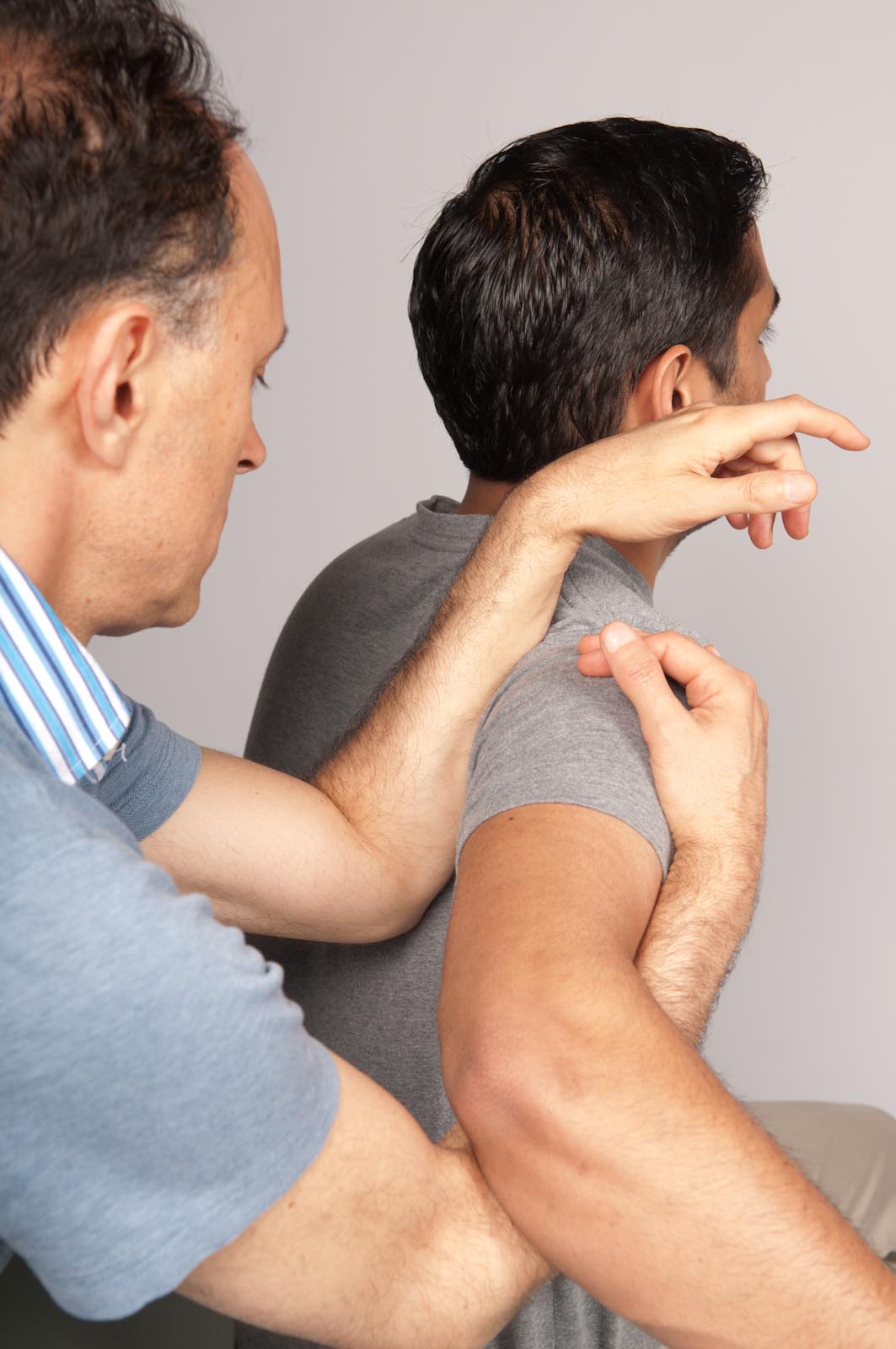
More Frequent Massage Sessions are More Effective for Neck Pain
Multiple 60-minute massages per week were more effective than fewer or shorter sessions for individuals with chronic neck pain.
How Targeted Therapy and Gentle Chiropractic Care Improve Pain Relief and Patient Mobility
This article explores some of the current methods of treatment for chronic heel pain and highlights the benefits of a gentle chiropractic approach to managing pain and increased mobility.
Effective Strategies for Foot & Joint Health: From Plantar Fasciitis to Arthritis Care
No matter which disorder you suffer from, starting your treatment plan, which should include exercise, flexibility training, and proper education, will make your life easier and healthier
Best Mattresses for Back Pain Relief: A Manual Therapist’s Guide to Spinal Alignment and Recovery
This guide explores what separates a truly therapeutic mattress from one that’s just comfortable enough to ignore the problem.
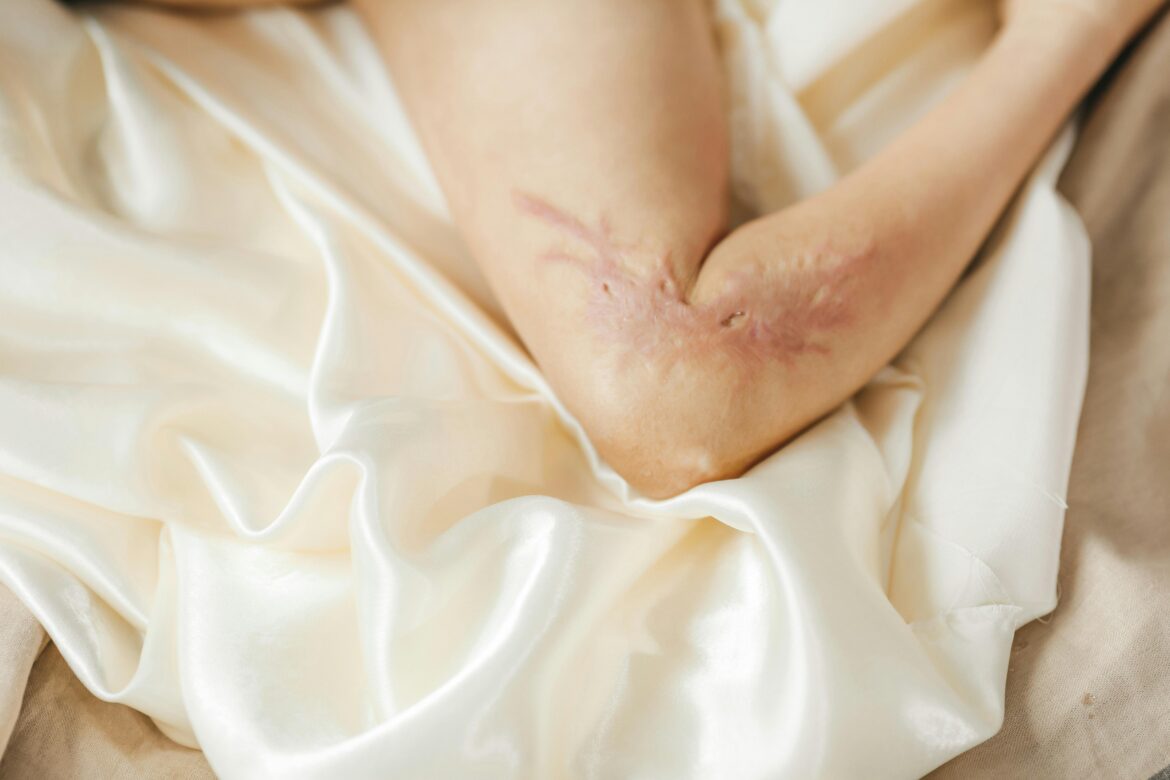
When Healing Limits Movement: How Scar Tissue Can Affect Mobility After Injury
Careful observation, clear communication, appropriate pressure, and a function-focused approach can help support more comfortable movement.
Fasting and Muscle Cramps: What Manual Therapists Should Know
Learn why fasting clients may experience muscle cramps or tightness, how hydration and electrolyte balance affect muscle function, and what manual therapists should know.
Massage Therapy is an Effective Post-Exercise Recovery Technique to Reduce DOMS
The authors concluded that massage appears to be the most effective method that was studied for reducing DOMS and perceived fatigue.
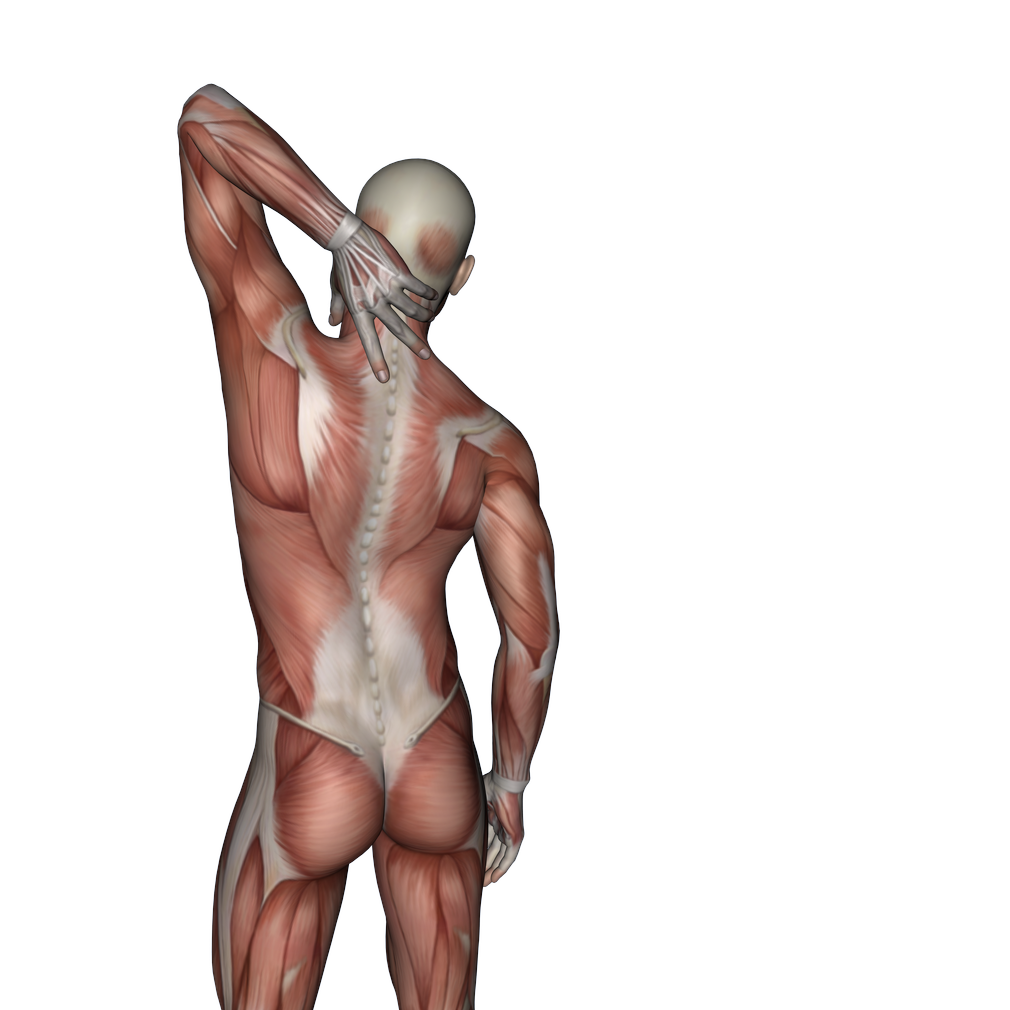
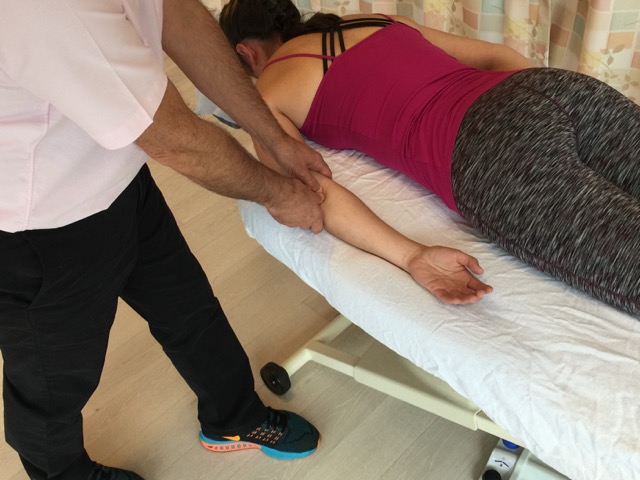
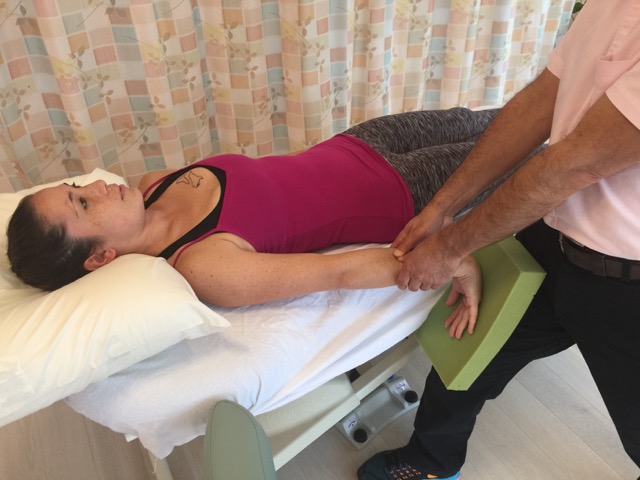
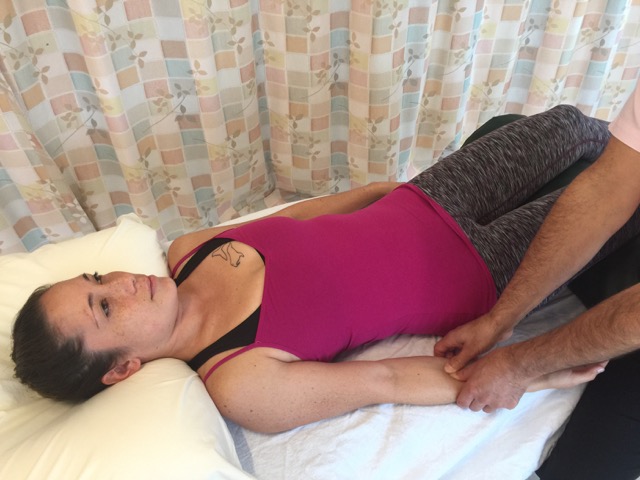
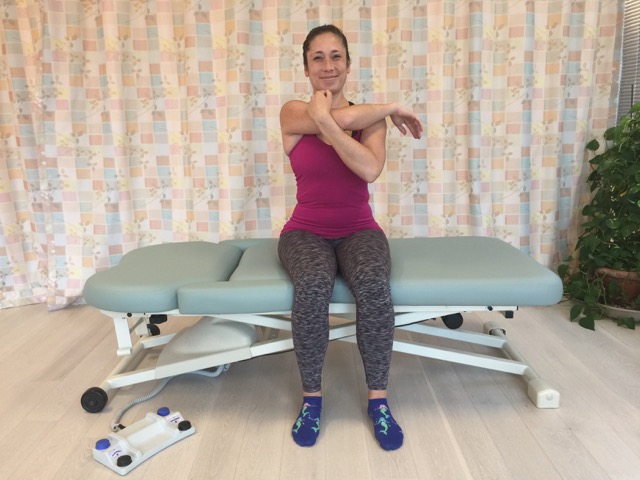
How do we Treat Upper Crossed Syndrome with Manual Therapy?
Especially effective for the pectoralis musculature is to use pin and stretch technique. With the client/patient supine and positioned toward the side of the table, pin the musculature with your finger pads as you bring the client/patient’s abducted arm off the side of the table and down into horizontal extension.
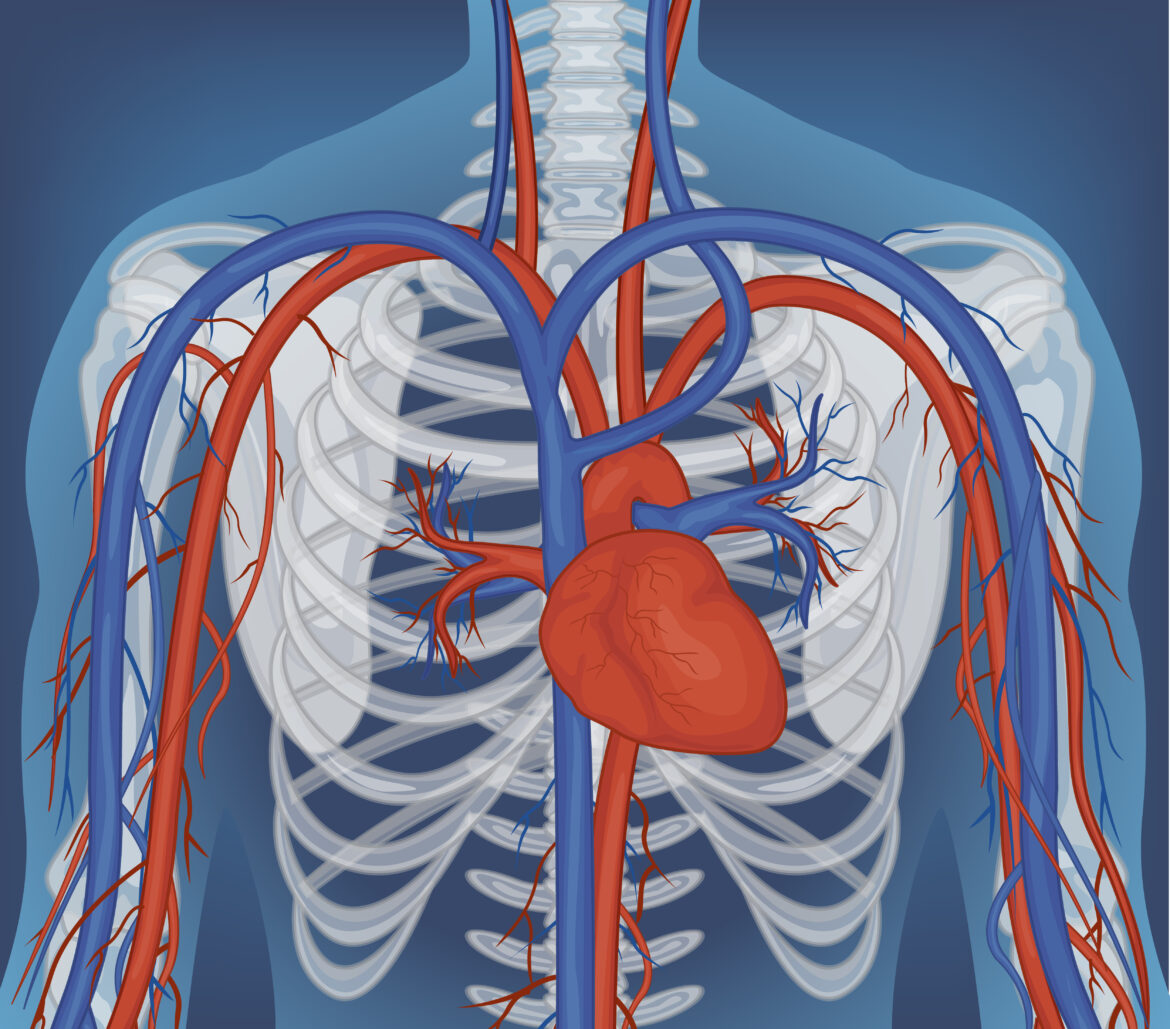
The Skeletal Muscle Pump: How Musculoskeletal Function Shapes Venous Return and Vein Health
Manual therapists and other professionals who work with older adults have a critical role in supporting this pump in the years prior to significant structural vein disease.
Muscle Strengthening Helps Decrease Neck Pain in the Workplace
The researchers found that the only intervention to clearly improve neck pain that was supported by the evidence in these studies was targeted neck and shoulder musculature strengthening exercise.
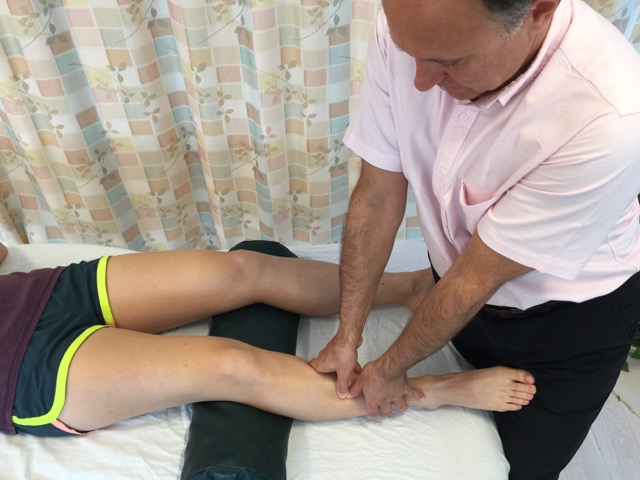
How do we treat shin splints with manual therapy?
The first goal of manual therapy treatment for shin splints is to relieve the tension of the involved musculature by lessening baseline muscle tone and eliminating any trigger points that might be present. The second goal is to treat swelling, if present.
Can manual therapy alter the thoracolumbar fascia?
To believe that manual therapy cannot affect the structure of thoracolumbar fascia is to deny the fundamental characteristic of soft tissue known as creep!
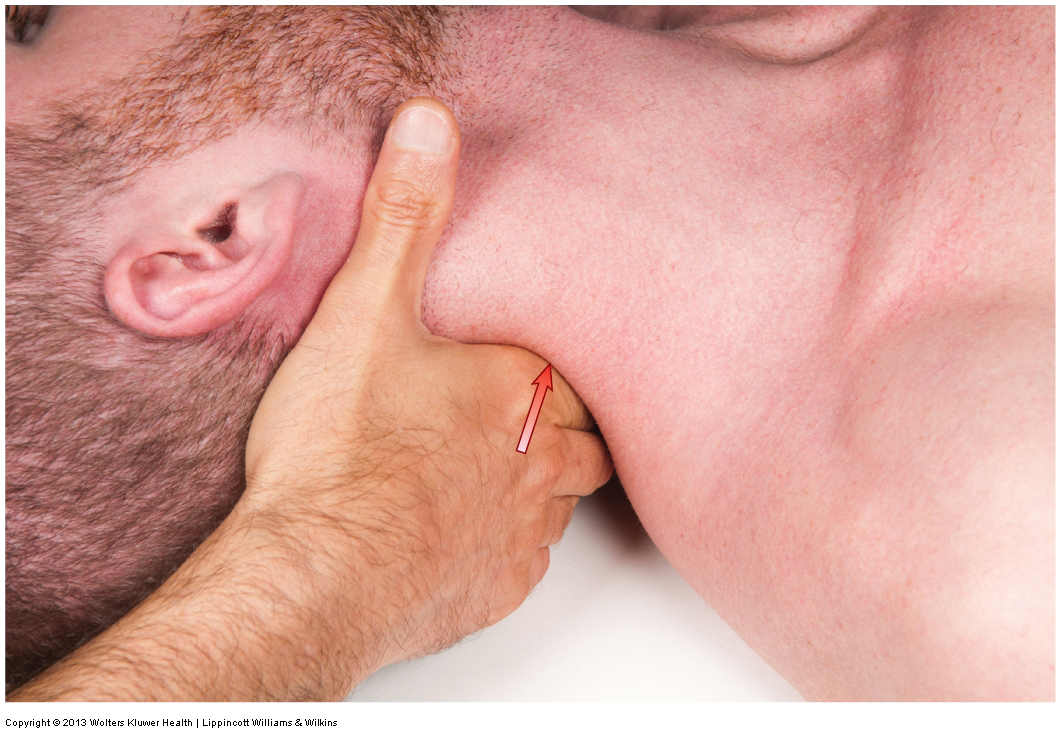
How do we treat Golfer’s Elbow with manual therapy?
A good protocol for manual therapy for golfer’s elbow involves fascial spreading, longitudinal and cross fiber strokes, and pin and stretch technique.
How do we treat sciatica with manual therapy?
It is necessary to determine what condition is causing the sciatic nerve compression and address that. If the cause is a pathologic disc, then addressing factors that affect disc compression is appropriate.
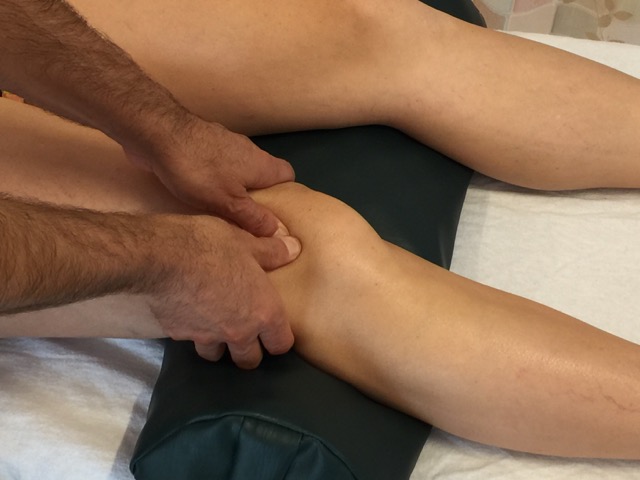
How do we treat patellofemoral syndrome with manual therapy?
Given the many possible causes of patellofemoral syndrome, following is a typical guideline for manual therapy treatment.
How do we treat spinal joint dysfunction with manual therapy?
Joint mobilization treatment (Grade IV or V) is the most effective treatment technique to remedy a spinal joint dysfunction hypomobility once it is present.
Manual therapy and self-care treatment of wrist sprain, strain & tendinitis
A wrist sprain is challenging to treat with manual therapy because it is essentially an overstretching of ligaments, which causes joint instability.
What is the medical approach to wrist sprains, strains, and tendinitis?
The medical approach to wrist sprain/strain is usually to recommend rest, a brace, and non-steroidal or steroidal anti-inflammatory medication.
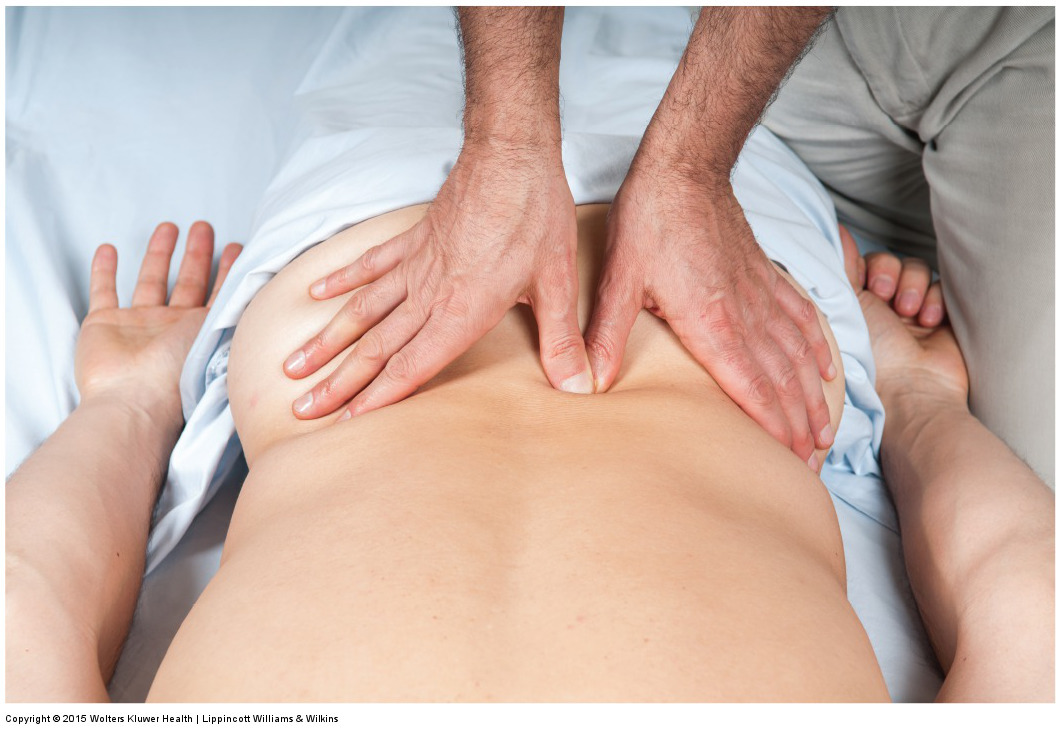
Deep Pressure Massage to the Low Back – Deep Strokes
To transition to perform deep strokes and maintain proper body mechanics, it is necessary to transition from being perpendicular to be slightly horizontal to glide along the client’s body. However, minimize the horizontal direction or pressure into the client’s tissues will be lost.
What are the self-care and medical approaches to spinal joint dysfunction?
As a rule, moist heat followed by stretching is beneficial for spinal hypomobilities, and strengthening is beneficial for regions of spinal hypermobility.
Massage Therapy Reduces Pain in Mothers After Caesarean Birth
Mothers who had massage therapy after caesarean birth had increased relaxation, decreased pain, decreased stress, and decreased opioid use.
What are the self-care and medical approaches to rotator cuff pathology?
Self-care for the client/patient with rotator cuff pathology depends on the specific muscle that is affected and the specific pathology that is present.
Body Mechanics for Deep Pressure Massage to the Low Back – Overview
For proper body mechanics, it is important to support your contact. Place the thumb pad of your right hand over the thumb pad contact of the left hand to brace/support it. Proper location of the brace is to place the right thumb pad on the dorsal surface of the distal phalanx of the thumb.
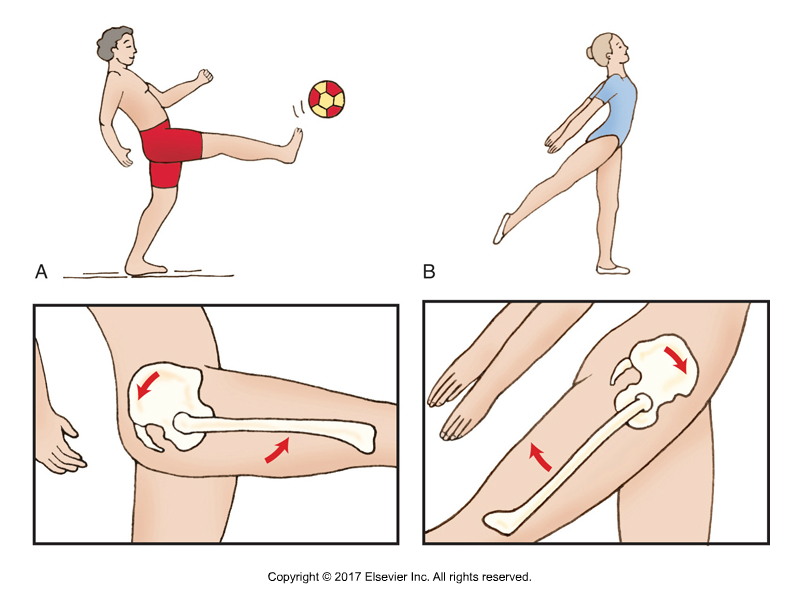
Altered Pelvic Bone Motion and Sacroiliac Pain
These findings of altered movement and glide support the concept that altered mechanics of the sacroiliac joint are correlated with the presence of pain.
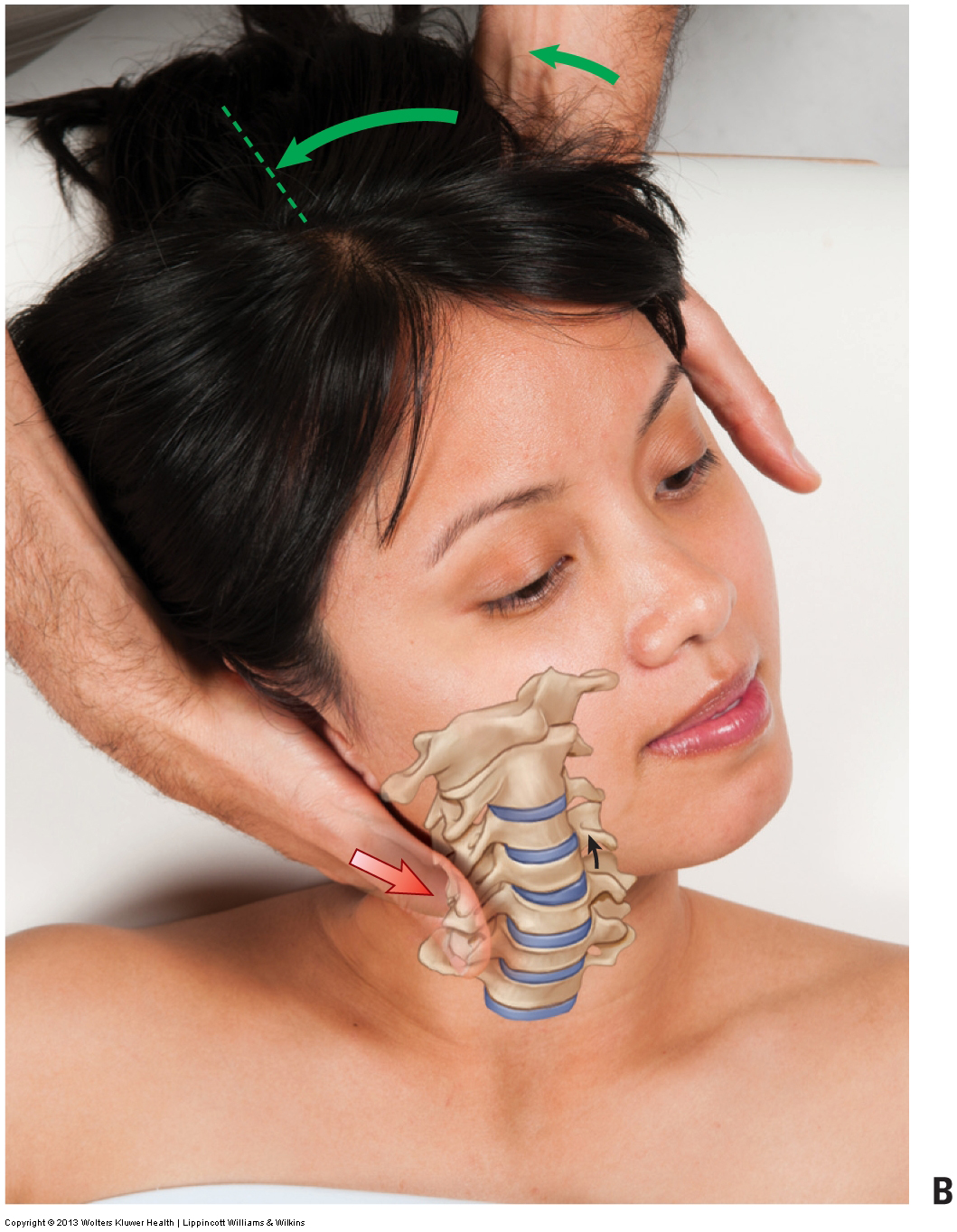
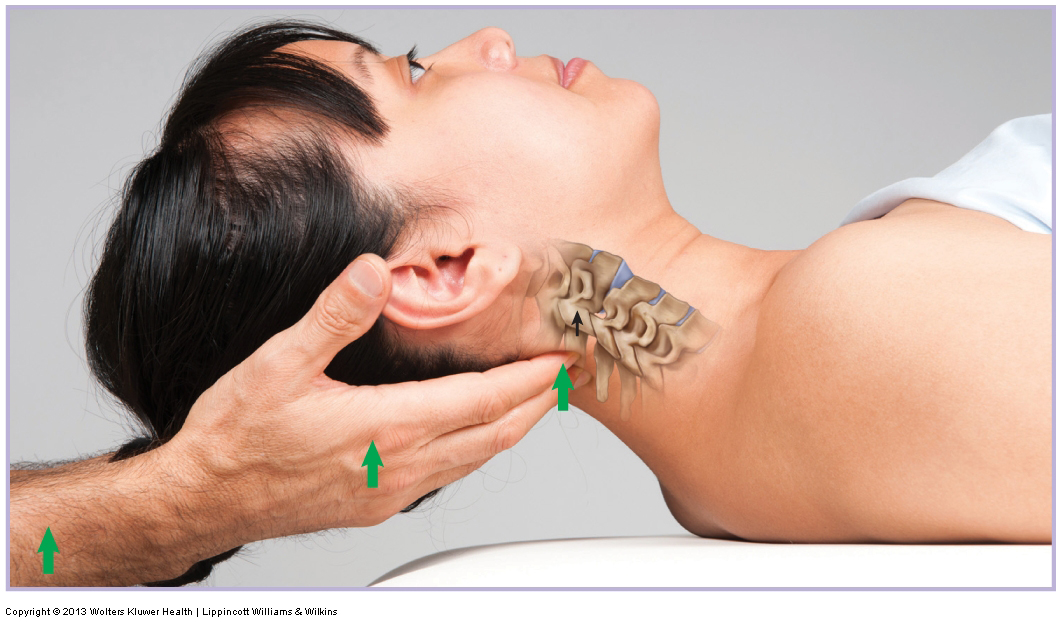
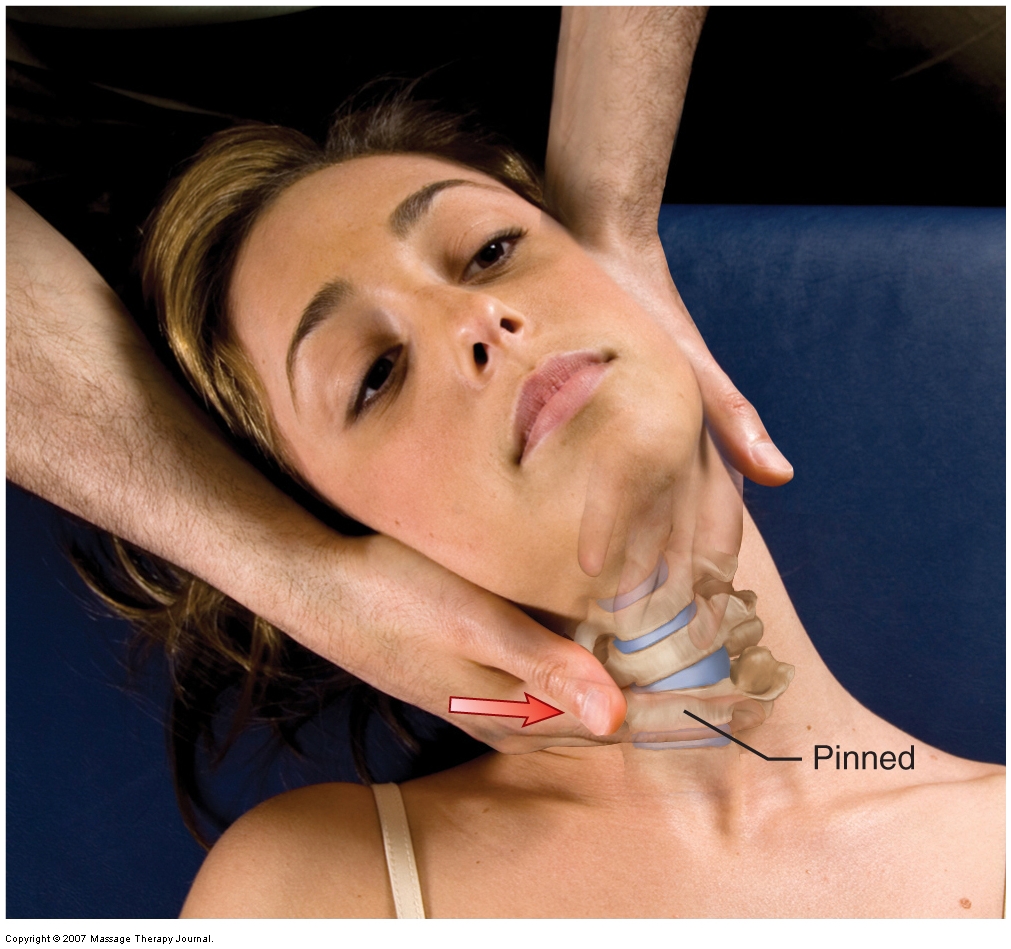
How do we treat Whiplash with manual therapy?
A whiplash/neck sprain is problematic to treat because it involves overstretching of ligaments, which causes joint instability.
Decreasing Postoperative Abdominal Adhesions using Manual Therapy
This study demonstrates that manual therapy initiated immediately postoperatively is an effective preventive approach for postoperative abdominal adhesions.
How Access to Care Shapes the Work of Manual Therapists
Therapists hold a unique position in healthcare. They bridge the gap between insurance realities and healing outcomes.