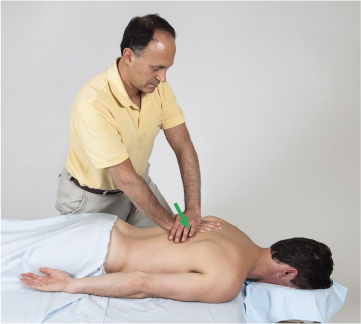
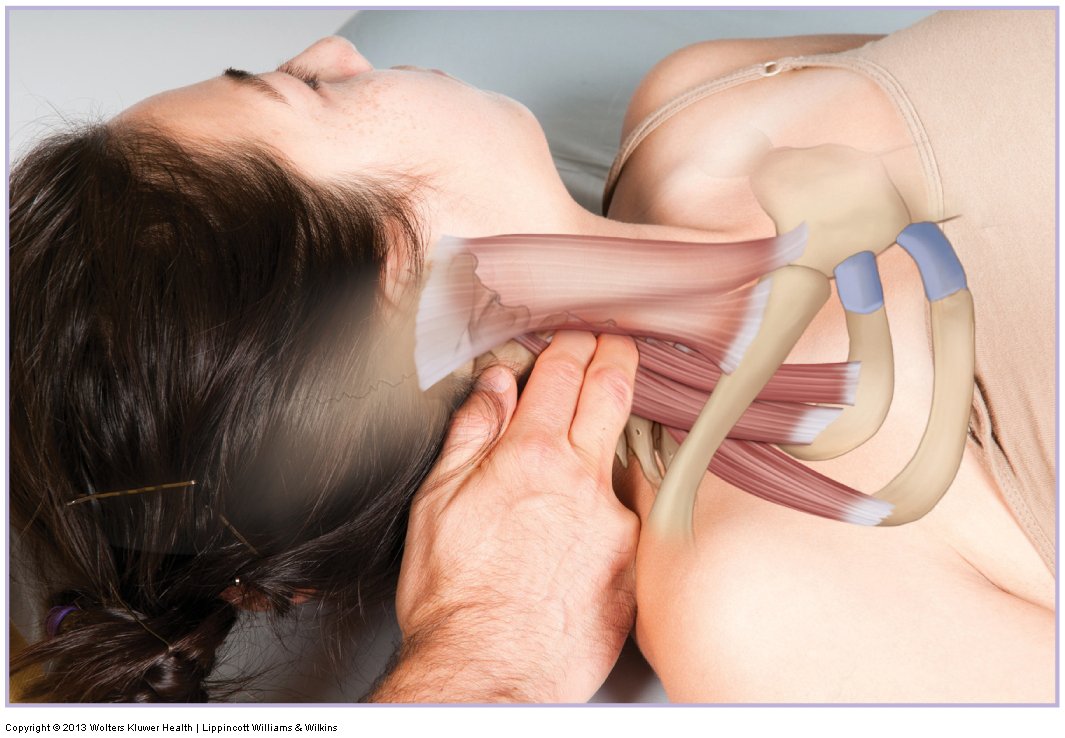
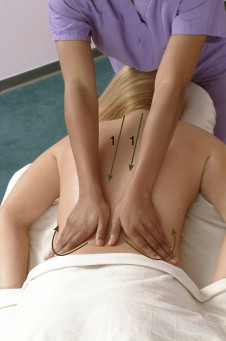
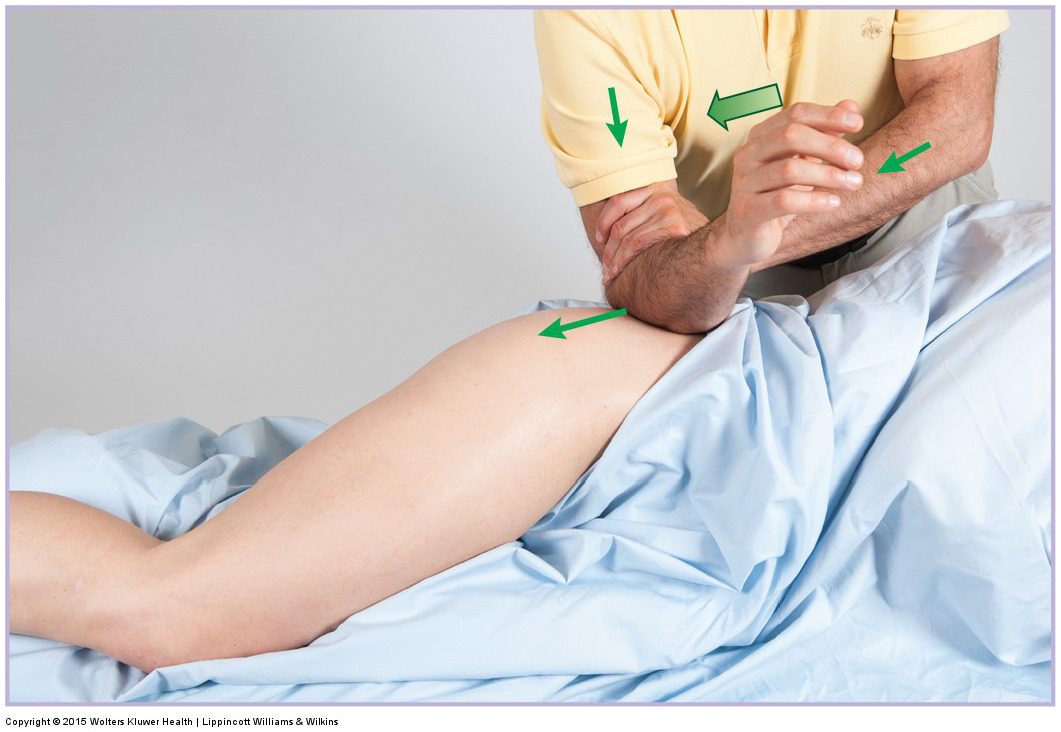
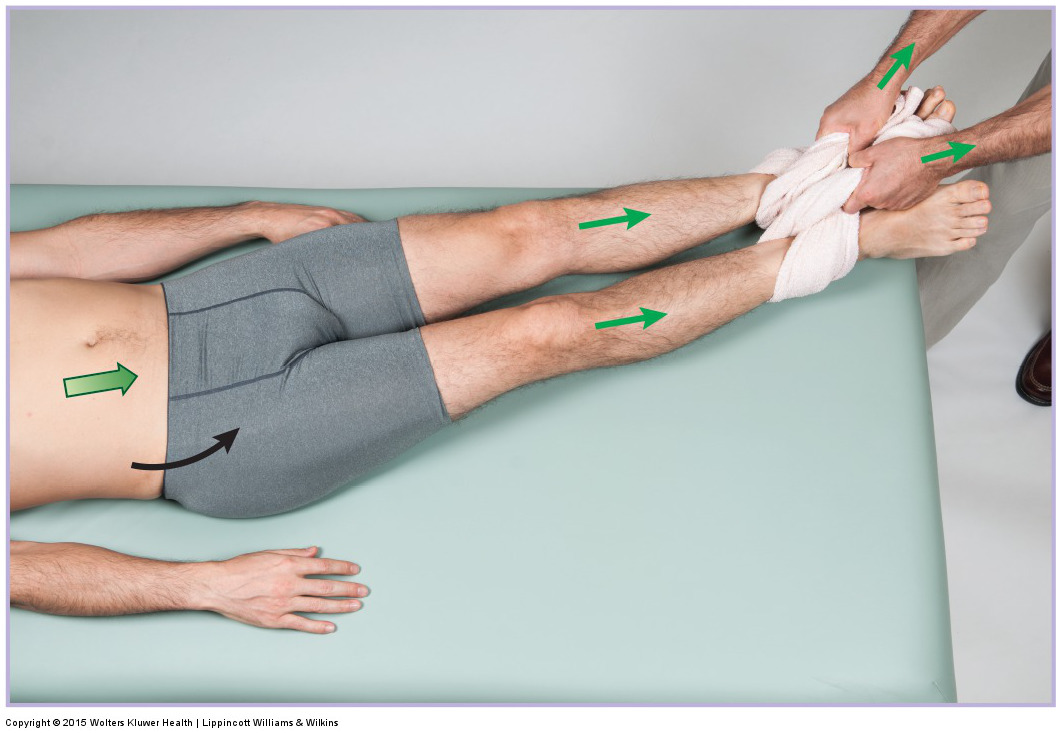
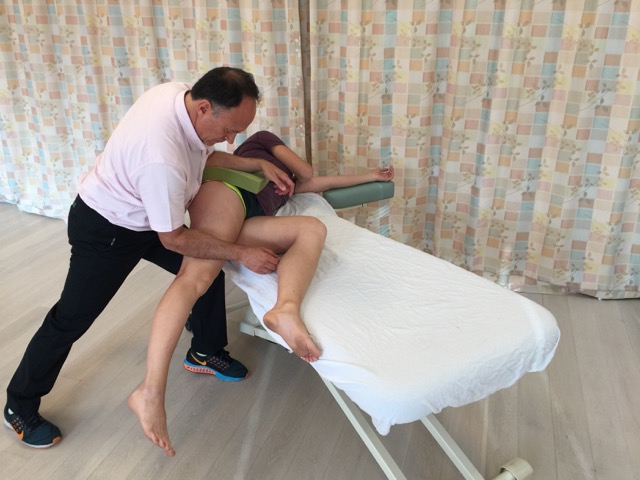
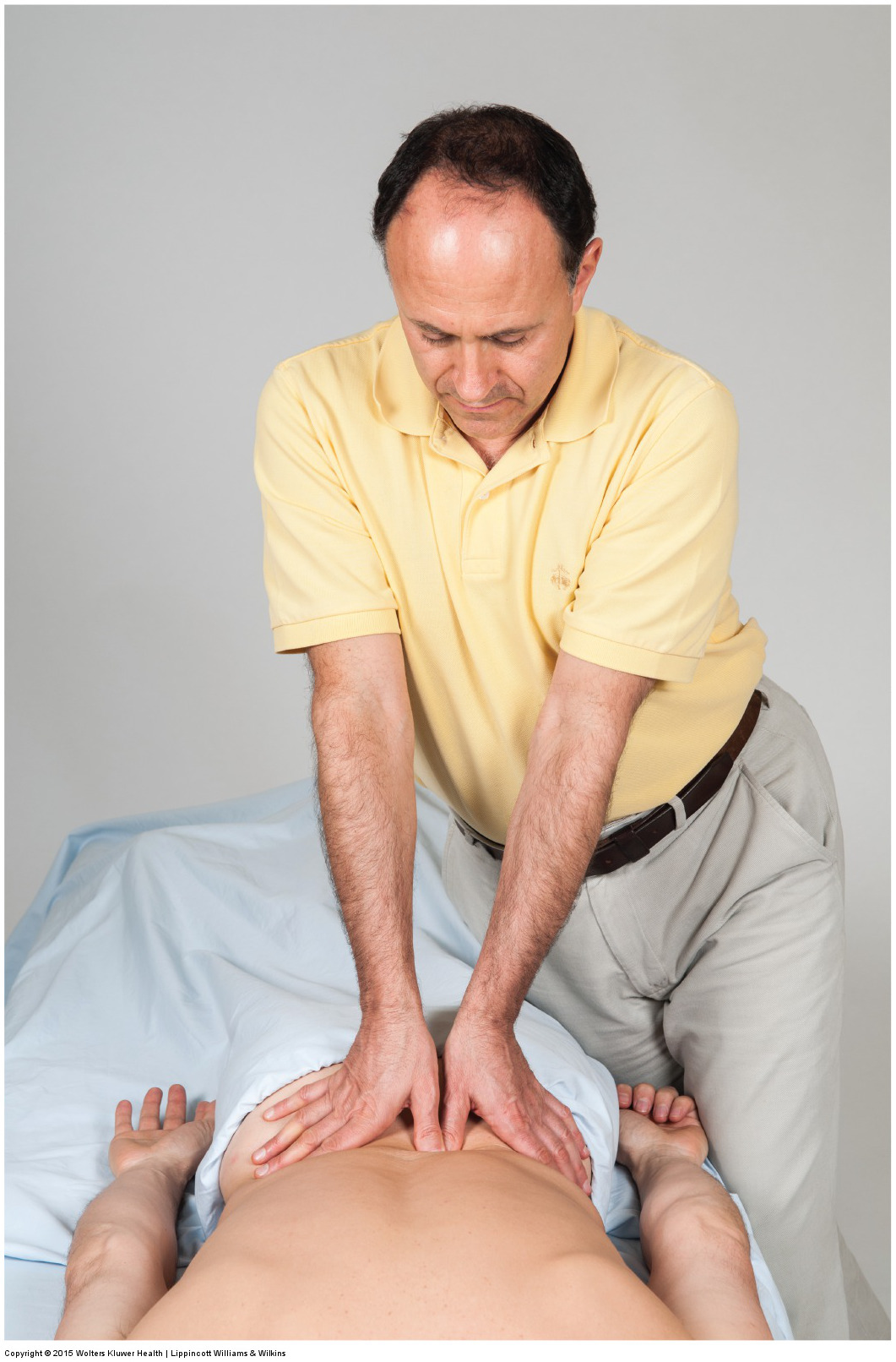
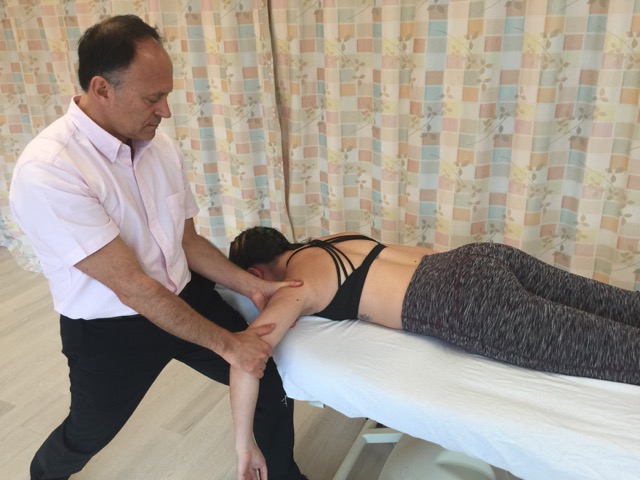
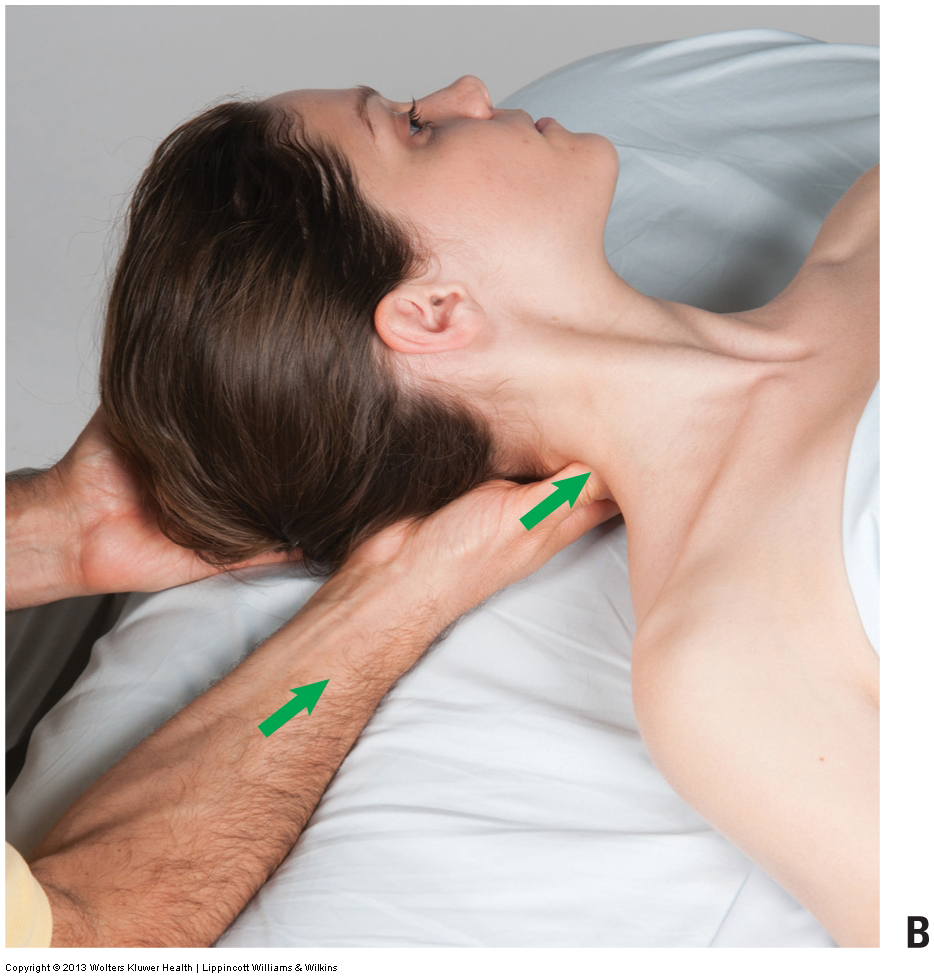
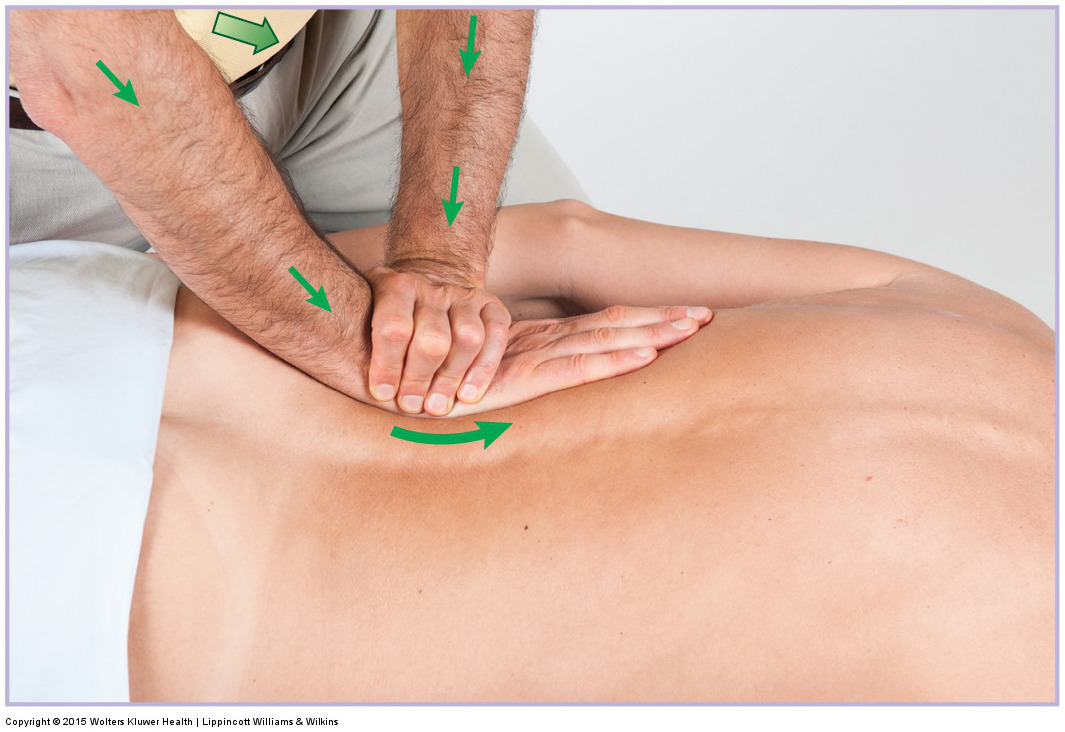
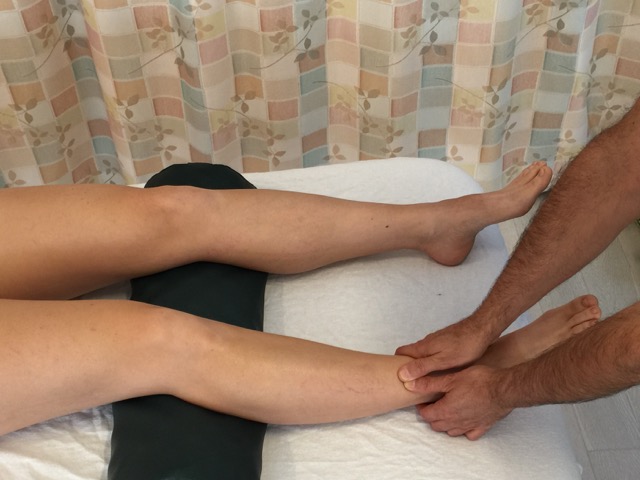
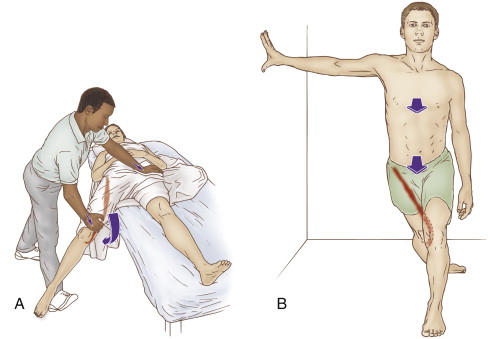
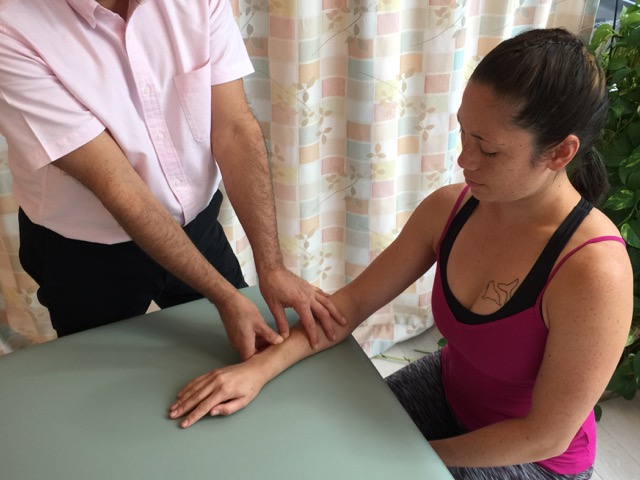
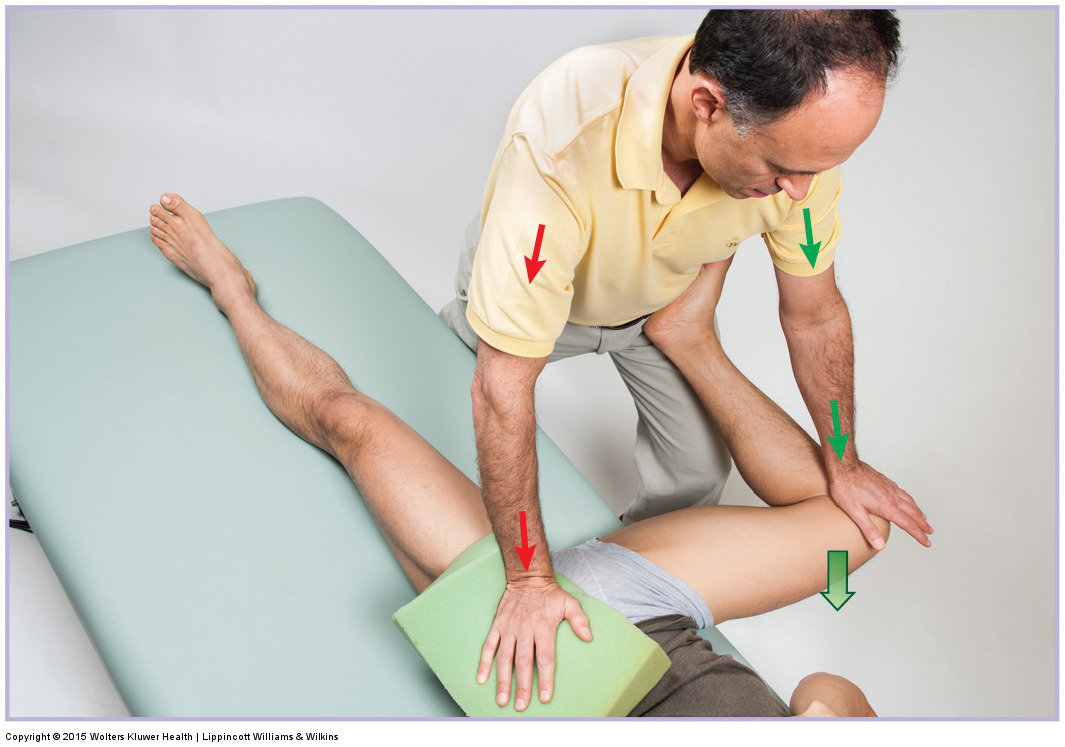
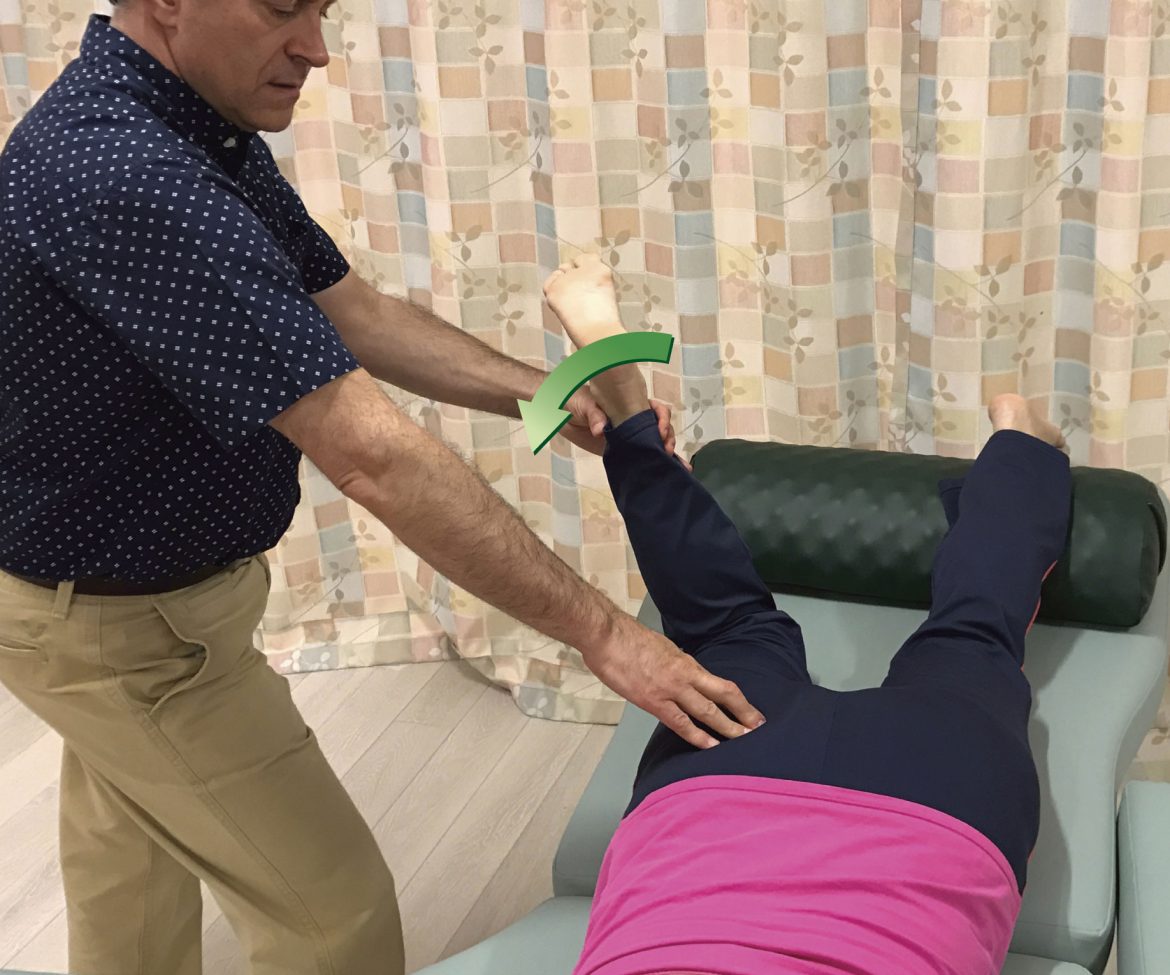
When performing soft tissue manipulation/massage, it is always wise to begin with light to medium pressure, and then transition to deeper pressure.
Manual Therapy Certification for Chiropractors
What is most important in any Manual Therapy Certification program is marrying together the underlying science with the hands-on manual therapy skills.
7 Osteopathic Concepts Every Manual Therapist Should Understand
Understanding these concepts can transform the way you think and work. Mastery of the hands begins with mastery of these foundational ideas.
Real-World Massage Therapy is Effective for Treating Lower Back Pain
After 12 weeks, more than half of the patients reported improved outcomes in terms of pain reduction, and meaningful physical and mental improvement.
Breathing, Posture, and Allergies: The Overlooked Triangle in Manual Therapy
Allergies can be a year-round driver of compensatory breathing and musculoskeletal dysfunction, making them highly relevant in clinical assessment and care planning.
Ten Massage Therapy “Dos and Don’ts”
This is not a list of precautions or contraindications for massage therapy. Rather it is list of miscellaneous, somewhat random, “dos and don’ts” that I believe would improve massage therapy sessions with clients.
What are the self-care and medical approaches to frozen shoulder?
An easy & effective self-care stretch for frozen shoulder is the “finger walk” on a wall. To warm the tissues, heat should be applied before stretching.
How do we treat a pathologic disc with manual therapy?
Traction can be beneficial for the client/patient with a pathologic disc because it opens up the intervertebral foramina of the spine.
Manual Therapy Certification for Massage Therapists
There are two major reasons why a massage therapist should consider working toward and earning a Continuing Education Certificate in Manual Therapy.
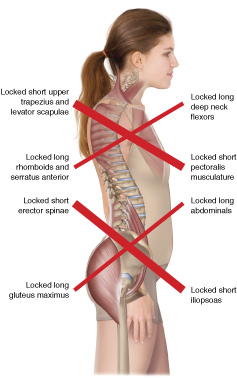
Locked Short Muscles – Locked Long Muscles
Two opposing muscle groups, the “facilitated” muscles that are locked short and the “inhibited” muscles that are locked long.
Manual Therapy as a Treatment for Overuse Injures
Regarding overuse injuroies, the authors suggested that if manual therapy were administered early, before pathological changes occur…
Self-Care and Medical Approaches to Slumped Spinal Posture
An excellent self-care exercise is to recommend that the client/patient lie supine on an exercise ball to help move the thoracolumbar spine into extension.
How do we treat lower crossed syndrome with manual therapy?
If consistent manual therapy care is given, including heat, massage, and stretching, lower crossed syndrome responds very well to treatment.
What are the self-care and medical approaches to De Quervain’s Syndrome?
Perhaps the most important self-care advice for De Quervain’s syndrome is to avoid as much as possible offending postures and activities of the thumb.
How do we treat iliotibial band friction syndrome with manual therapy?
Manual therapy for iliotibial band friction syndrome is directed toward reducing the inflammation of the condition and correcting its underlying cause.
How do we treat spasmed low back muscles with manual therapy?
Manual therapy treatment for low back muscle tightness involves hot and cold hydrotherapy, soft tissue manipulation, stretching, and joint mobilization.
How do we treat frozen shoulder with manual therapy?
Manual therapy stretching and joint mobilization are two essential treatment modalities when working on a client with frozen shoulder.
How do we treat hamstring strain with manual therapy?
The goal of manual therapy for a chronic hamstring strain is to decrease hamstring hypertonicity and help promote healthy scar formation.
How do we treat spasmed neck muscles with manual therapy?
Manual therapy treatment: Manual therapy treatment for spasmed muscles of the neck (tightness of neck musculature) includes all the major soft tissue technique tools. Heat hydrotherapy, soft tissue manipulation, stretching, and joint mobilization (also known as arthrofascial stretching/AFS). It is …
Self-care and medical approaches to iliotibial band friction syndrome
Self-care for iliotibial band friction syndrome (ITBFS) begins with RICE: rest, ice, compression, and elevation. And offending activities should be avoided.
Key Strategies to Improve Your Manual Therapy Skills
In this blog, we will share key strategies to help you enhance your manual therapy skills and build confidence in your practice.
How do we treat low back strains and sprains with manual therapy?
For a low back strain / sprain, because the muscles of the low back are so large and powerful, the first goal of manual therapy is to reduce the spasming.
How do we treat an ankle sprain with manual therapy?
Manual therapy treatment for an acute inversion ankle sprain is aimed at decreasing swelling and inflammation and relieving associated muscle spasming.
What are the self-care and medical approaches to meralgia paresthetica?
Self-care for meralgia paresthetica: heat and stretching of the involved muscles, and removing the physical stress factors that contribute to the condition.
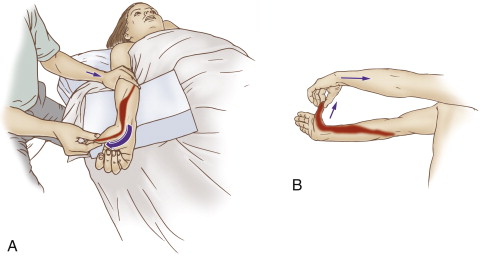
How do we treat De Quervain’s syndrome with manual therapy?
Once present, De Quervain’s syndrome (De Quervain’s disease) can be challenging to resolve, but manual therapy treatment can be very beneficial.
How do we treat adductor strain with manual therapy?
Once chronic, manual therapy for an adductor strain is geared toward decreasing muscle tightness, myofascial trigger points, and fascial adhesions.
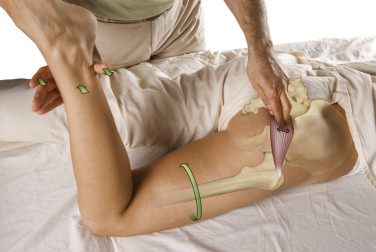
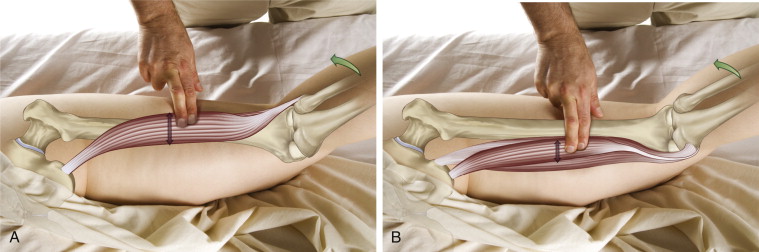
Pin and Stretch Technique
Pin and stretch technique focuses the force of the stretch on the region of the muscle that is between the pinned point and the attachment that is moved.
How do we treat Tennis Elbow with manual therapy?
A good manual therapy protocol for tennis elbow is fascial spreading, longitudinal and cross fiber strokes, and pin and stretch to the posterior forearm.
The Science Behind Physiotherapy’s Role in Muscle Recovery
Let’s discuss why and how physiotherapy works and how it is crucial in proper muscle recovery.
ASK Dr. Joe – “Ask Me Anything”
I am creating a new blog post feature to my content called Ask Dr. Joe, or perhaps better put, Ask Me Anything*. With Ask Me Anything, you can write to me by email (joseph.e.muscolino@gmail.com) and ask me any question about: …