Self-care for the client/patient with rotator cuff pathology depends on the specific muscle that is affected and the specific pathology that is present.
Scapular Dyskinesis Increases the Risk of Future Shoulder Pain
One potential risk factor for shoulder pain is scapular dyskinesis. Scapular dyskinesis refers to altered position and motion of the scapula.
What are the self-care and medical approaches to frozen shoulder?
An easy & effective self-care stretch for frozen shoulder is the “finger walk” on a wall. To warm the tissues, heat should be applied before stretching.
Six Causes of Shoulder Impingement Syndrome – Part 3
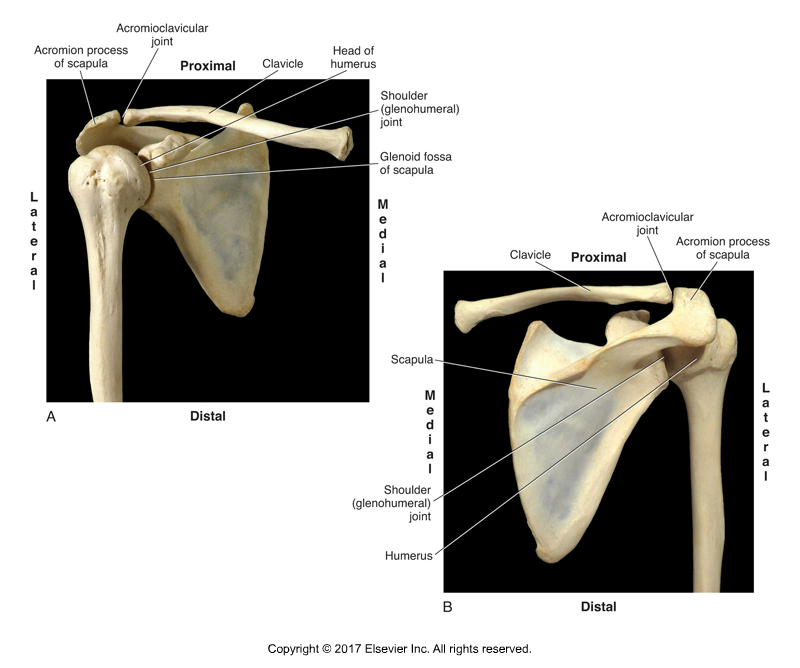
Another reason for shoulder impingement syndrome to occur is insufficient elevation of the clavicle. Most of scapular upward rotation is actually caused by elevation of the clavicle at the sternoclavicular joint, so if clavicular elevation is prevented for any reason, shoulder impingement syndrome can occur.
Six Causes of Shoulder Impingement Syndrome – Part 2
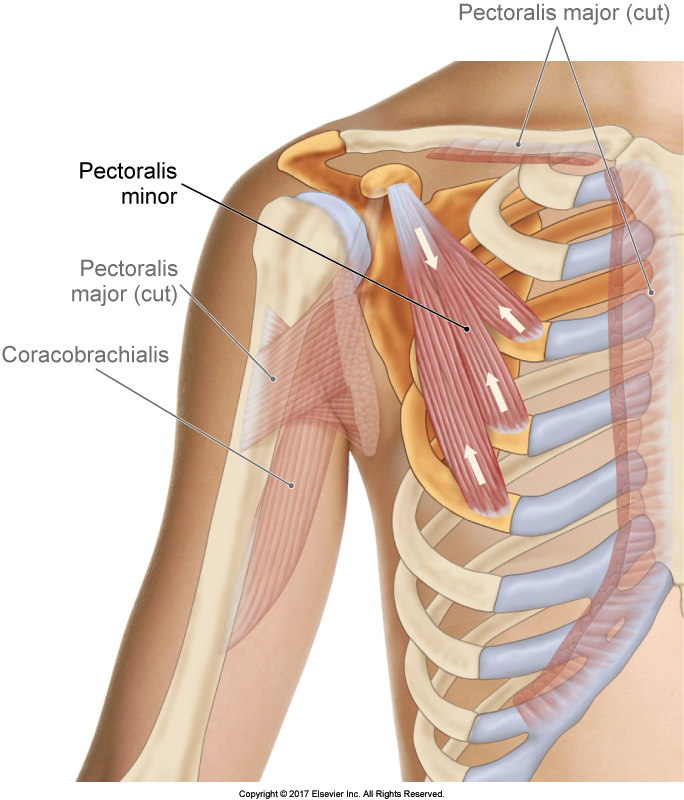
For scapular upward rotation to occur, scapular downward rotator musculature must lengthen. If scapular downward rotation muscles are tight, they might not be flexible enough to allow for scapular upward rotation, thereby causing shoulder impingement syndrome to occur.
Six Causes of Shoulder Impingement Syndrome – Part 1
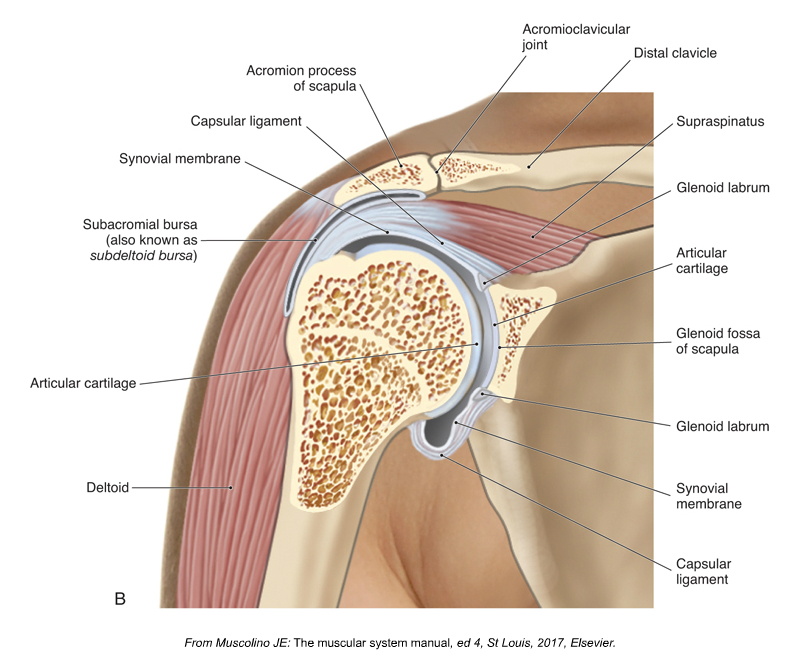
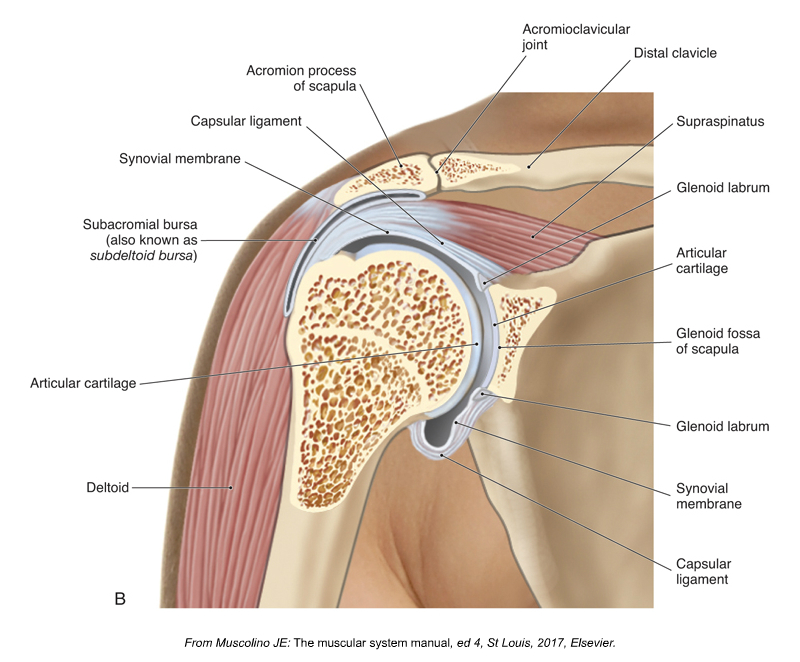
Shoulder impingement syndrome is a condition in which the distal tendon of the supraspinatus and the subacromial bursa become impinged between the head of the humerus and the acromion process of the scapula. Following are the six major causes of shoulder impingement syndrome.
Muscle Tightness as a Cause of Frozen Shoulder
This case series of five patients with frozen shoulder demonstrates that active muscle guarding may be a major contributing factor to frozen shoulder.
What are the causes of frozen shoulder?
Frozen shoulder is a condition in which the glenohumeral joint loses mobility. The two stages are neurogenic frozen shoulder and adhesive capsulitis.
Signs, symptoms, and assessment (diagnosis) of frozen shoulder
The most common sign of frozen shoulder is decreased GH joint range of motion. Most commonly affected motions are abduction, flexion, and lateral rotation.
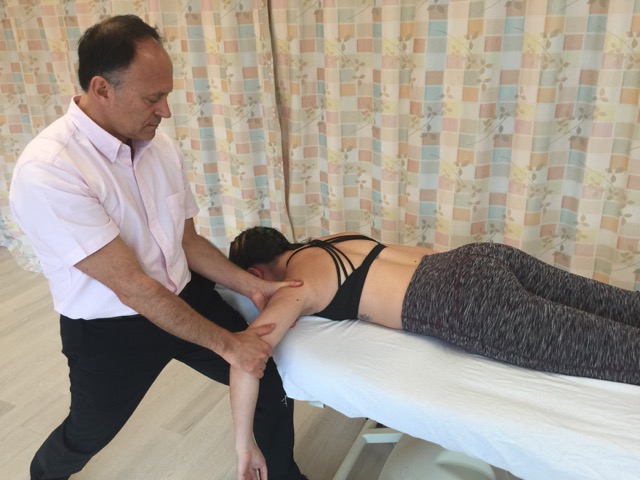
How do we treat frozen shoulder with manual therapy?
Manual therapy stretching and joint mobilization are two essential treatment modalities when working on a client with frozen shoulder.