Manual Therapy Treatment for Spinal Joint Dysfunction
The treatment for a hypomobile spinal joint is straightforward and simple. Joint mobilization is the most effective treatment technique to remedy a hypomobility once it is present. Proactive gross range of motion stretching can be beneficial toward preventing the development of hypomobile spinal joints, but once the hypomobile segments are present, gross stretching usually does not work because adjacent compensatory hypermobilities move when the stretch is performed, thereby eliminating the need of the hypomobile joint to move.
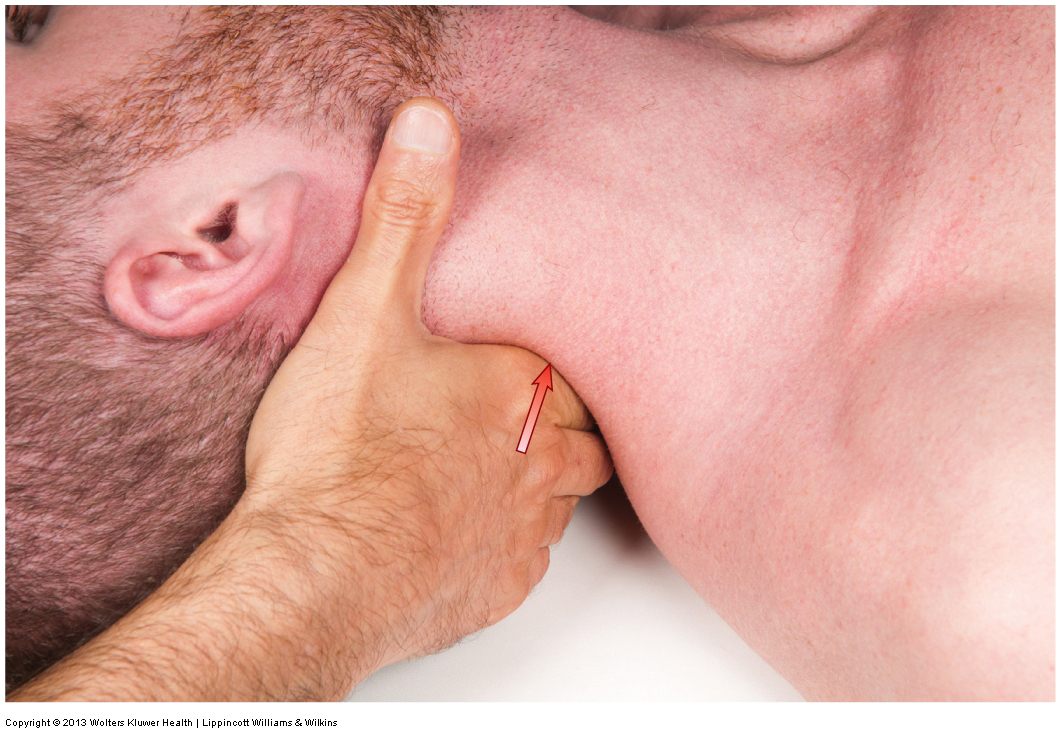
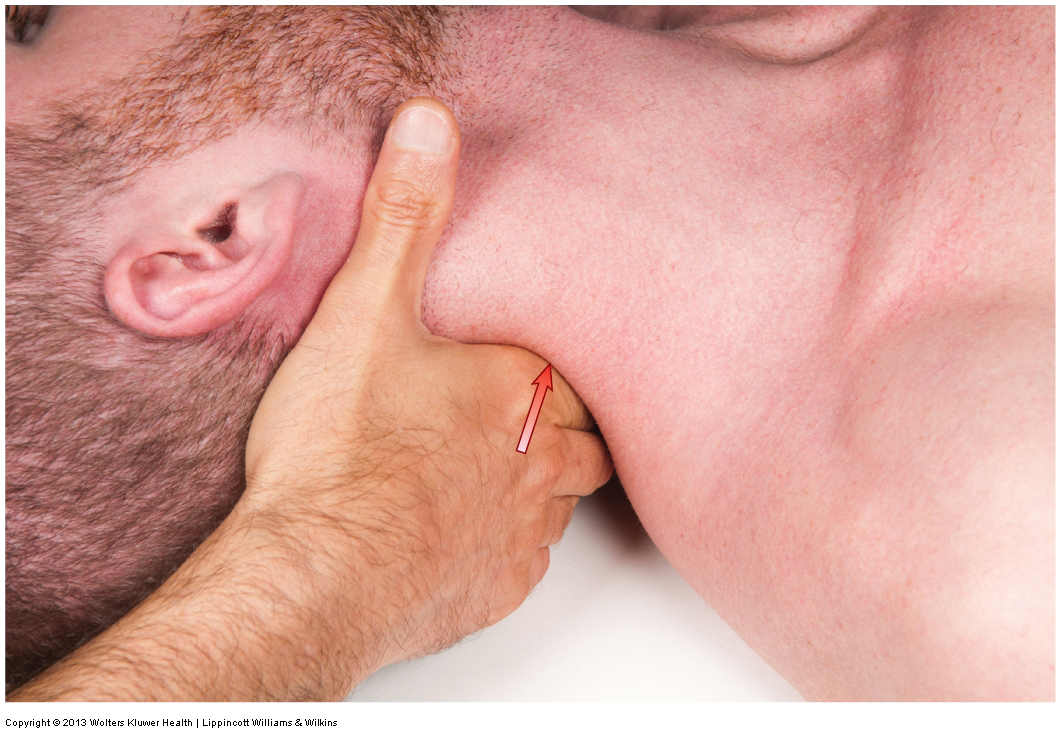
Joint mobilization of the cervical spine with the client in the supine position. Permission: Joseph E. Muscolino. Advanced Treatment Techniques for the Manual Therapist: Neck (2013).
Joint mobilization is described as a Grade IV joint manipulation. Essentially, joint mobilization treatment technique is identical to joint motion palpation assessment technique. The only difference is that motion palpation is done for the purpose of assessment, and joint mobilization is done for the purpose of treatment. But the mechanics are the same: one vertebra is pinned while the adjacent vertebra is moved relative to it, thereby requiring motion at the joint located between them. The force that is placed into the vertebra that is moved should be gently but firm, the bone should be moved a very small distance (literally a fraction of a centimeter), the movement should be slow, and the position of mobilization should be held for less than a second. This mobilization is usually repeated for a set of 3-5 oscillations; and anywhere from one to three sets of oscillations are often done. Or another guideline is to perform the joint mobilization for 10, 15, or perhaps 20 seconds. The final determinant should always be the response of the client’s/patient’s tissues.
In effect, joint mobilization is a very specific form of soft tissue stretching. It is extremely important to emphasize that a Grade IV mobilization should never involve a fast thrust. Implementing a fast thrust is defined as a Grade V manipulation and is usually only legal for Chiropractic and Osteopathic physicians.
Because joint mobilization is a type of soft tissue stretch, it is most effectively performed during the treatment session after the area has first been warmed up. Therefore, it should be done after moist heat, soft tissue manipulation, and perhaps after regular full range of motion stretching have been done. There are a couple of exceptions to this guideline. One exception is if extremely deep soft tissue manipulation is done, then the client/patient might guard when it comes to stretching and mobilizing the joint afterward. Guarding will prevent the client/patient from relaxing and allowing the therapist to stretch their tissues. For this reason, very deep work should be done after stretching and mobilization.
The other exception is if the client/patient feels an obstruction on the side to which their spine is moved. When stretching the client’s/patient’s spine in one direction, the client/patient should feel the restriction to movement on the opposite side of the joint because these tissues are being lengthened and stretched. If the client/patient feels an obstruction on the side to which they are being moved, then the stretching should be stopped and joint mobilization done first (the stretching can then be done after the mobilization). For example, if the client’s/patient’s neck is being stretched into right lateral flexion and the client’s/patient’s motion is decreased and they feel a restriction on the left side of the neck, then it is taut soft tissue on the left side of the neck that is stopping the motion and stretching would be the appropriate treatment. If instead the client/patient feels an obstruction on the right side of the neck, then it is not taut soft tissue restricting the motion; rather it is a hypomobile joint dysfunction that needs to be addressed before stretching can be effectively done.
Because much of the restriction of a hypomobile spinal joint is due to tight musculature and fascial adhesions, moist heat and soft tissue manipulation can also be extremely effective. The soft tissue manipulation must be done with deep pressure to reach the deeper intrinsic tissues around the facet joints. As always, begin with light to medium pressure and gradually transition to deeper pressure. Pay specific attention to laminar groove musculature (semispinalis, multifidus, rotatores). It can also be beneficial to prep the hypomobile joints with cervical traction to further loosen the joint tissues. As helpful as these other therapies can be, it must be emphasized that if grade IV joint mobilization is not part of the treatment regimen, it is unlikely that hypomobile joints can ever be truly remedied.
Joint mobilization is the appropriate treatment for a hypomobile joint dysfunction, not a hypermobile segment. If a hypermobile spinal joint is found, look for adjacent hypomobile joints for which the hypermobile joint might be compensating. Treating and removing the hypomobility might alleviate the demand for excessive motion at the hypermobile joint and alleviate some of the problem. Unfortunately, as stated earlier, once fascial ligamentous tissues have been overstretched, they rarely fully resolve and become appropriately taut again. For this reason, strengthening of nearby musculature is important toward restoring stability to a region of the spine where hypermobile joints are located.
Because joint dysfunction typically causes no pain or decreased range of motion in the early to middle stages, clients often do not present for treatment until this condition is very chronic and progressed, and therefore stubborn and resistant to treatment. However, if consistent care is given, the condition can respond well to manual therapy. There are two aims of manual therapy for this condition. The first is to mobilize any and all hypomobilities. The second is to address any other conditions, including postural distortion patterns that the client/patient might have that are contributing to the joint dysfunction.
Summary of Manual Therapy Treatment Protocol for Spinal Joint Dysfunction
| For Hypomobile Joint Dysfunction: |
| 1. Heat, soft tissue manipulation, and stretching of the associated musculature, with special attention paid to the laminar groove muscles. |
| 2. Joint mobilization (arthrofascial stretching) of hypomobile spinal joints |
| 3. Assessment and treatment of any concomitant condition that is contributing to the joint dysfunction. |
| 5. Counsel the client/patient regarding posture |
| For Hypermobile Joint Dysfunction: |
| 1. Treat any adjacent hypomobilities (as indicated above) |
| 2. Assess and treat any concomitant condition that is contributing to the joint dysfunction. |
| 3. Counsel the client/patient regarding posture |
| 4. Strengthen the associated musculature of the spine to increase stability |
Precautions/Contraindications for Treatment of Spinal Joint Dysfunction
Any time that a spinal joint is stretched, a major precaution/contraindication is the presence of a space-occupying condition that might cause compression upon a spinal nerve in the intervertebral foramen. This is especially true for joint mobilization stretching because it introduces a very focused and powerful movement force into the joint. Therefore, before performing spinal joint mobilization, be sure to first assess for pathologic discs and bone spurs in the client’s/patient’s spine. If assessment testing results in nerve compression and referral into an extremity, mobilization into extension and/or lateral flexion to the side of referral is contraindicated. Joint mobilization is also contraindicated if the physical integrity of the client’s/patient’s spinal tissues is compromised, in other words, there is an acute sprain, strain, or osseous facture. It is also contraindicated for any joint hypermobility. Beyond space-occupying conditions and lack of physical tissue integrity, as a general rule, mobilizing the lumbar and cervical spine into extension should always be done with caution.