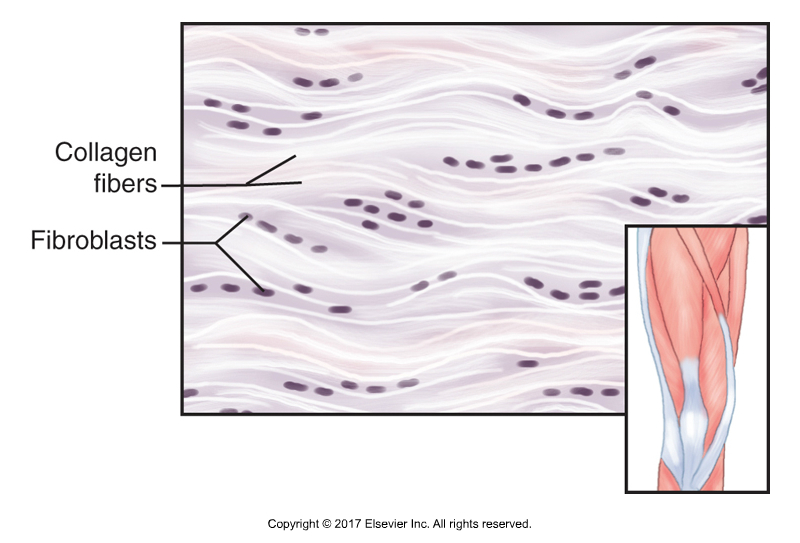
Are we really able to singularly and specifically isolate fascia…, to the exclusion of all other tissue… to create change? To that I am quite uncertain.
FASCIA – What It Is and Why It Matters… A New Book by David Lesondak
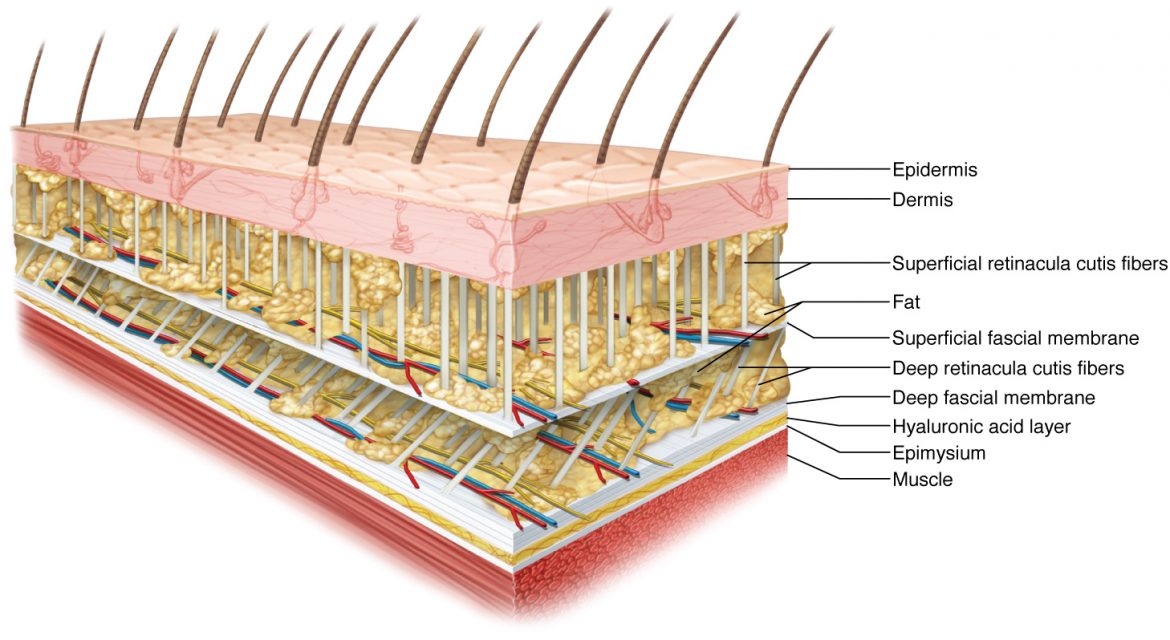
For me, fascia is the big picture. It’s a tissue and a system and it has connections from each individual cell all the way to the brain.
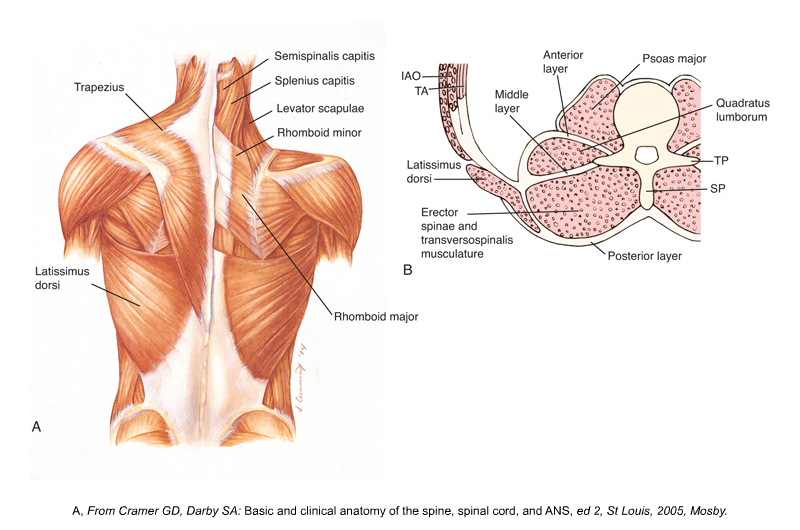
Can manual therapy alter the thoracolumbar fascia?
To believe that manual therapy cannot affect the structure of thoracolumbar fascia is to deny the fundamental characteristic of soft tissue known as creep!
What are the causes of sacroiliac joint dysfunction?
The sacroiliac joint is unique in that it is a transitional joint between the sacrum of the spine and the ilium of the pelvic bone of the lower extremity.
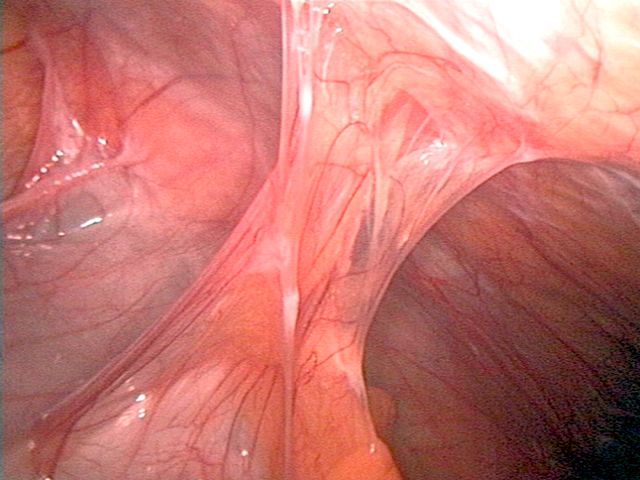
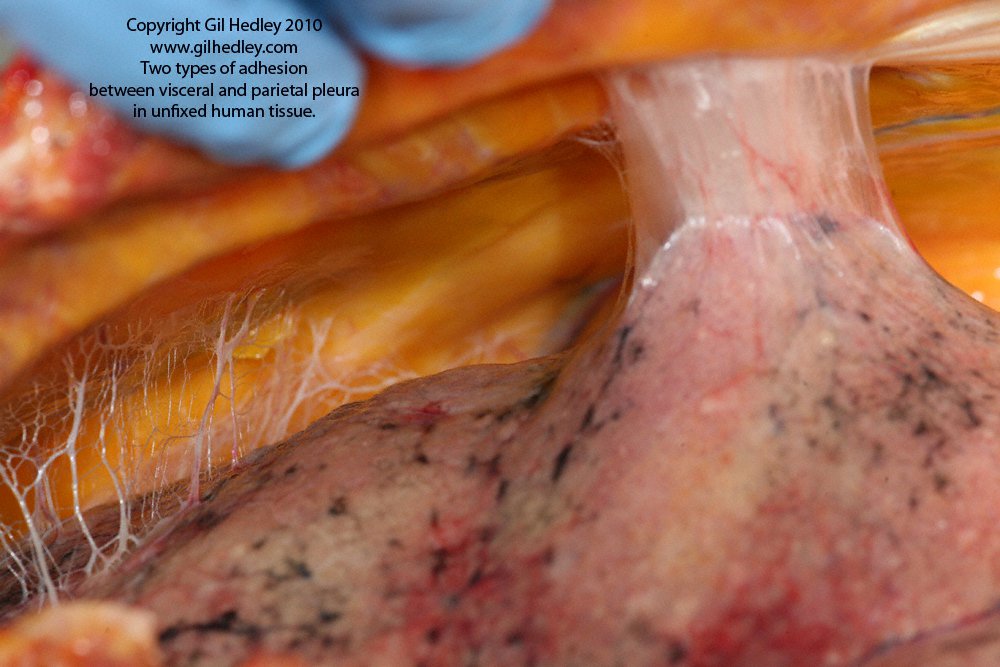
Decreasing Postoperative Abdominal Adhesions using Manual Therapy
This study demonstrates that manual therapy initiated immediately postoperatively is an effective preventive approach for postoperative abdominal adhesions.
The Frictionless Skin-Fascia Interface With Underlying Bone “Theory”
It would seem that taking any theory or ideology too far is dangerous. Certainly, the interfaces of soft tissues of the body are quite slippery…
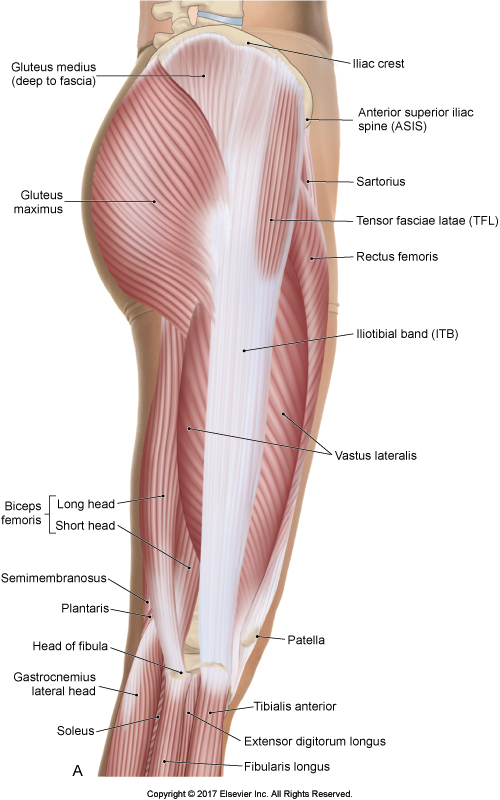
Can the Iliotibial Band (ITB) be stretched?
There seems to be a belief that the iliotibial band (ITB) cannot be stretched and thus manual treatment on the ITB is futile.
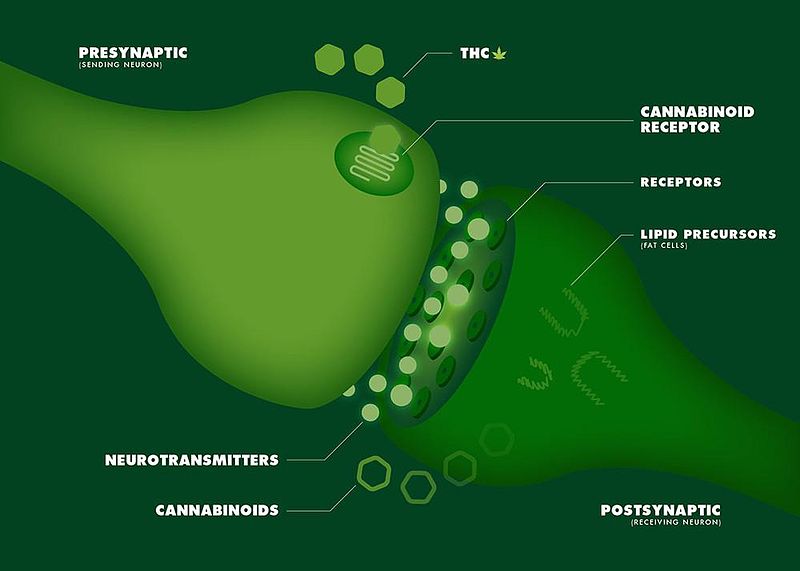
Expression of the Endocannabinoid Receptors in Human Fascial Tissue
Confirmation of endocannabinoid receptors in fascial tissue greatly bolsters our understanding of the mechanism of how manual and movement therapies work.
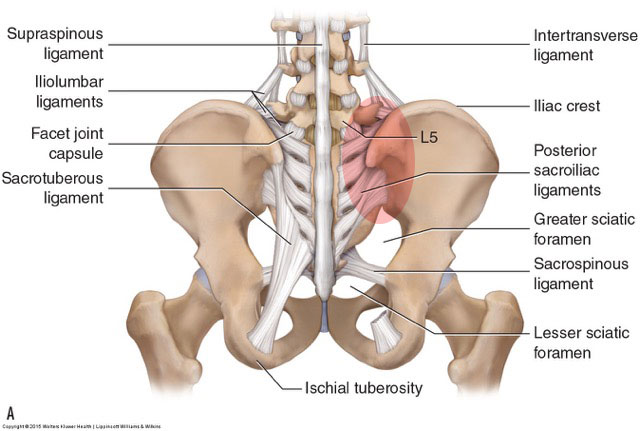
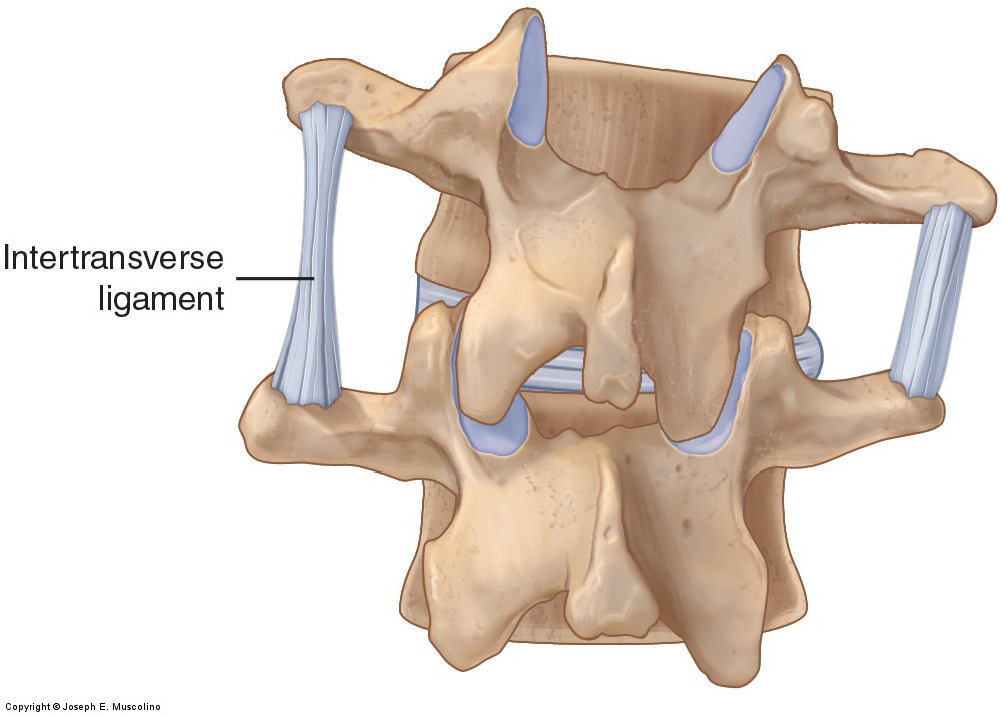
Ligaments of the Lumbar Spine and Pelvis
The “action” of a ligament is similar to that of an antagonist muscle. If either is tight/taut, it restricts motion to the opposite side.
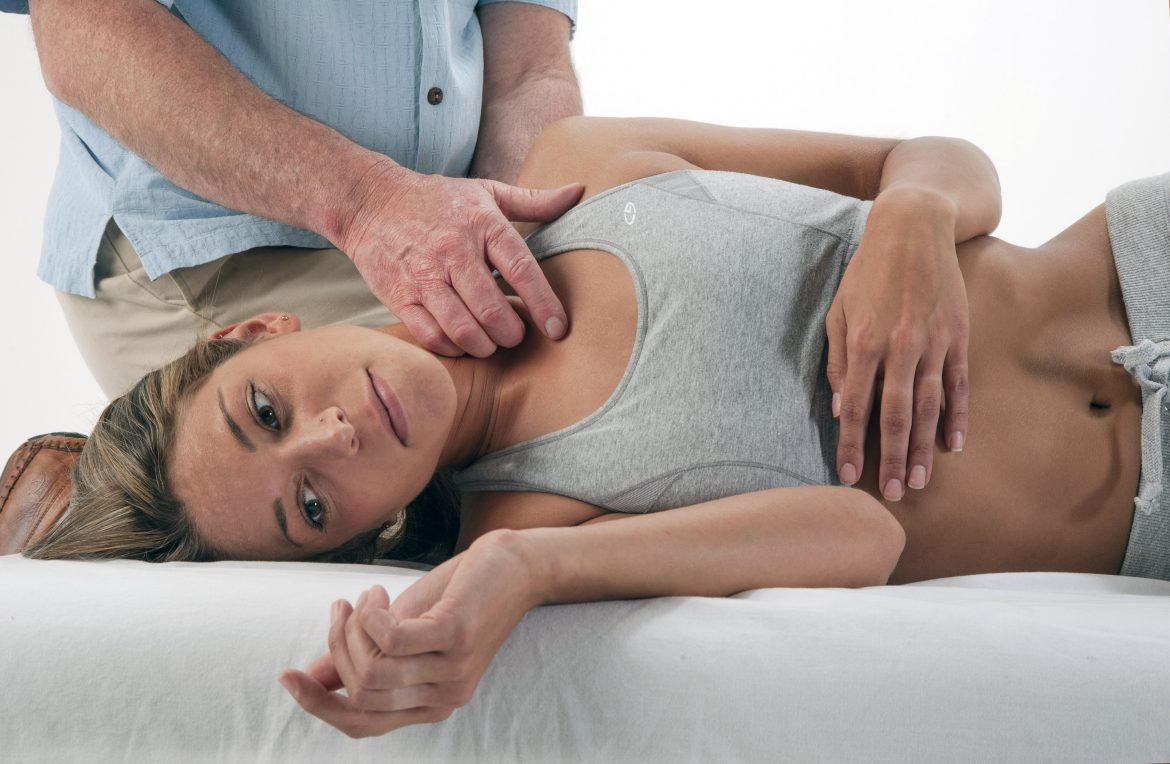
Myofascial Techniques… Working with the Sternocleidomastoid – by Til Luchau
SCM Differentiation Technique: delicate, comfortable, finger placement around the medial border of SCM, feeling for fascial elasticity & differentiation.
Interstitium: “Rediscovery” of the Connective Tissue System of the Body
It is ironic and bittersweet that this article recognizing the importance of the interstitium, reveals its ignorance of any research already published about that very soft tissue. By describing it as “previously unrecognized,” this demonstrates the long-standing bias against soft tissues by the Western Medicine.
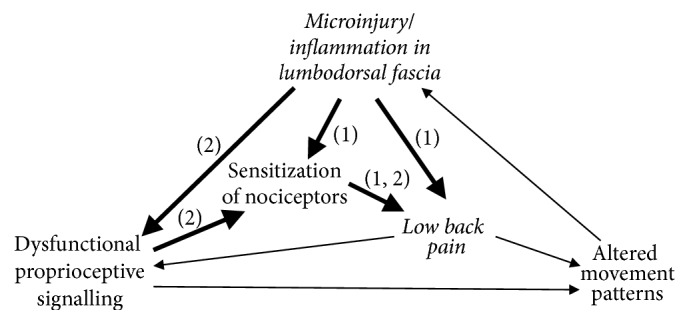
Lumbodorsal (Thoracolumbar) Fascia as a Source of Low Back Pain
In histological studies, the lumbodorsal fascia has been found to be densely innervated with nociceptive afferent pain fibers.
Painful Connections: Densification Versus Fibrosis of Fascia
The authors postulated that the deep fascia could be subjected to at least two different kinds of alterations: fibrosus and densification.
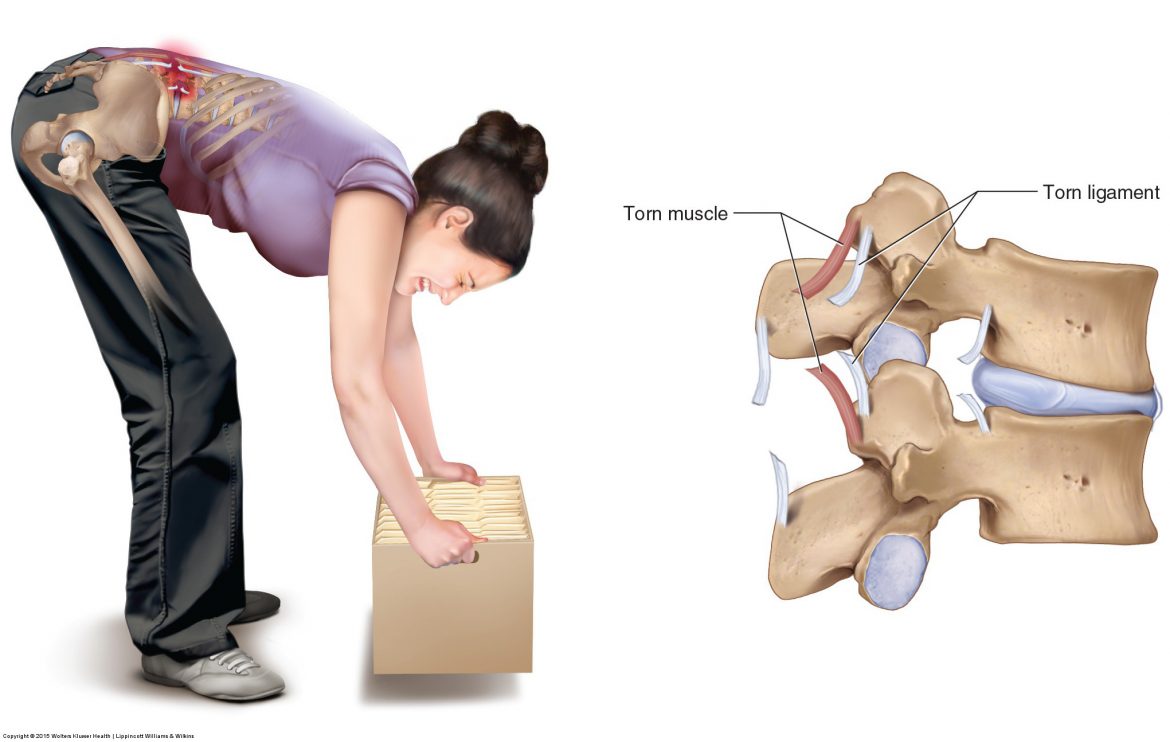
What are the causes of low back strains and sprains?
The two most common causes for a low back sprain / strain are macrotrauma and repetitive microtraumas, often involving bending and lifting.
What is in a name? – “Myofascial Release” or “Myofascial Induction”?
At the muscular level, myofascial release (MFR) is commonly believed to ease fascial gliding motion, releasing adhesions between fascia.
Signs, symptoms, and assessment of low back strains and sprains
A low back sprain and strain present a similar clinical picture. The client/patient will have low back spasming and pain, which will increase with motion.
Effect of Stretching on Fascial Injury and Movement Restriction
Research has shown that fascial injury with resultant movement restriction caused loss of fascial mobility on the opposite side of the body..
Fascial Thickness and Aging
The authors suggest that increased fascial thickness in the lumbar spine of elderly implies that the fascia dynamically adapts to the forces acting upon it.
Marjorie Brook – Proactive Ways to Prevent Postoperative Adhesion Formation
Gentle appropriate movement helps to prevent excessive scar tissue and keep scar tissue from limiting future movement.
Hypertonic / Tight Muscles of the Low Back and Pelvis
Four of the most common causes of tight muscles of the low back (or anywhere in the body) are: overuse, splinting, adaptive shortening, and overstretching.
Signs, Symptoms, and Assessment of Plantar Fasciitis
The most common symptom of plantar fasciitis is pain, usually worst in the morning, on the plantar side of the foot, located near the calcaneal attachment.
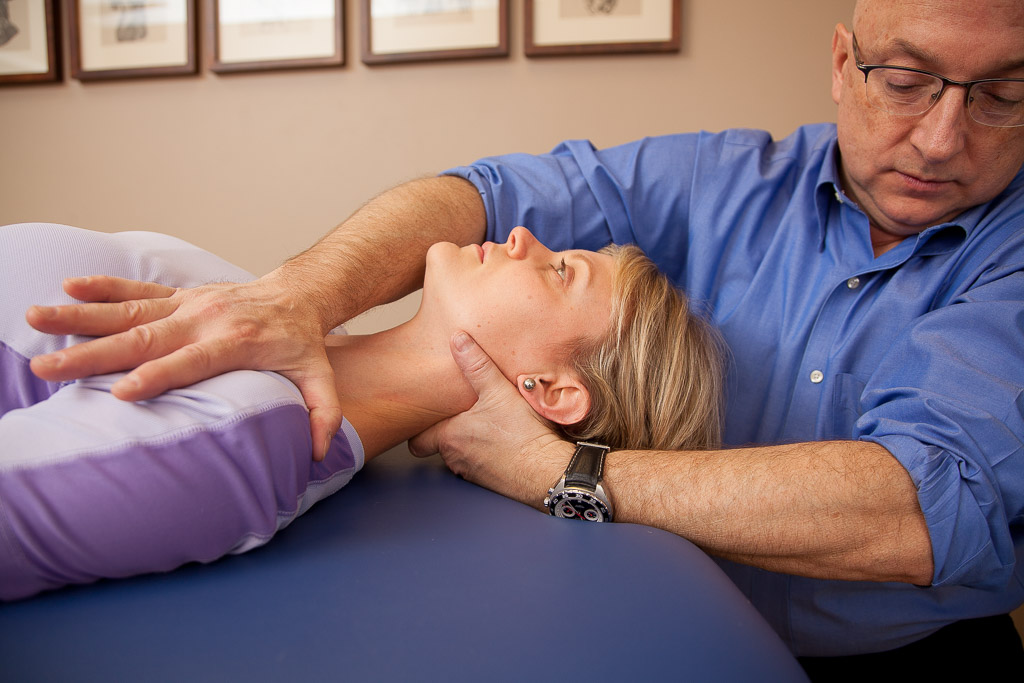
Fascial Adhesions of the Neck
Fascial adhesions may bind together the two opposing surfaces of a soft tissue interface, resulting in restricted mobility.