Introduction

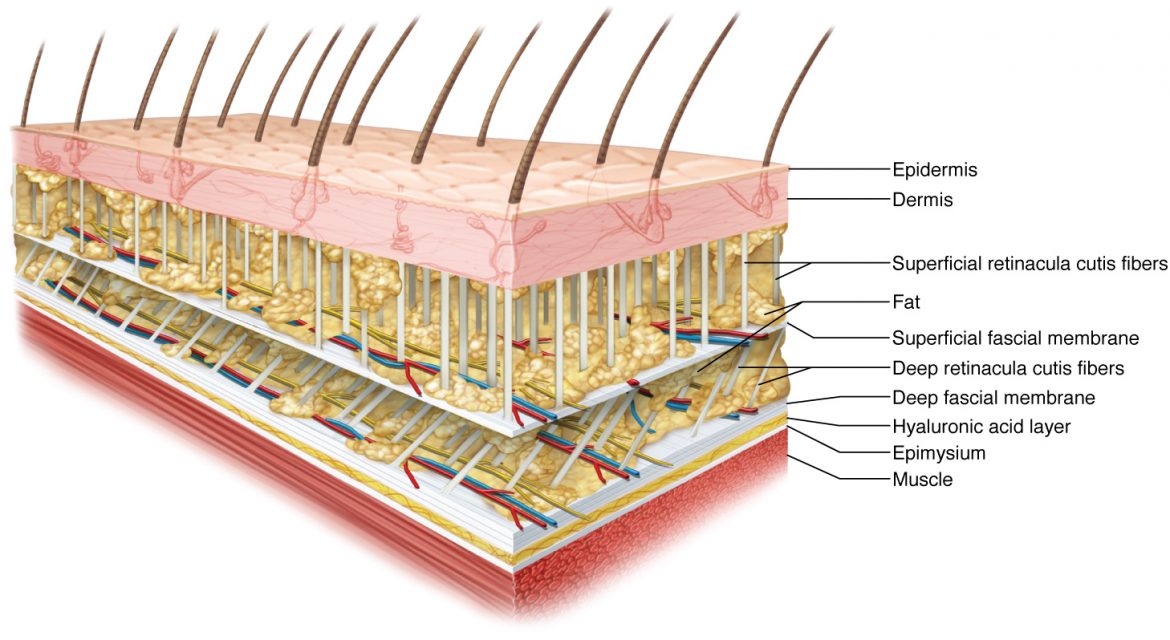
Subcutaneous fascia. Permission Joseph E. Muscolino. www.learnmuscles.com. Originally published in a massage therapy journal article: fascial structure (spring 2012).
There is “theory” popularized via the social media that because the skin-fascia interface onto underlying bone is frictionless, you cannot mobilize underlying bones unless the force placed into the patient’s/client’s body is perpendicular to the surface of the bone. The reasoning is as follows: because the interface between the skin-fascia and the underlying bone is frictionless, if a force is placed in any direction that is not perfectly perpendicular to the bone (in other words, the force is obliquely oriented such that a component of it is somewhat parallel with the bone and is therefore a shear force), the skin-fascia tissue layer would simply slide along the underlying bone instead of being transmitted into the bone to move/mobilize it. In effect, the theory holds that friction is needed between the fascia and bone in order for the force to be transmitted into the bone to move it.
This claim is “backed” by a 2002 Canadian study by Bereznick et al. Let’s walk through what recent studies say about this.
The 2002 Canadian Study
This 2002 Canadian study aimed to evaluate this frictionless concept with the chiropractic technique of joint mobilization / manipulation which, during thoracic manipulation attempts to apply obliquely oriented force vectors (oblique meaning being between perfectly perpendicular and perfectly parallel to the underlying bone) onto underlying vertebral spinous or transverse processes. As stated above, the premise of the study is that friction is required at the skin-fascia interface onto the bone for the applied shear force to grab/hook the bony process. The study assessed the friction at the thoracic skin-fascia interface onto the bone to determine the force that is actually transmitted onto the bones during thoracic joint mobilization.
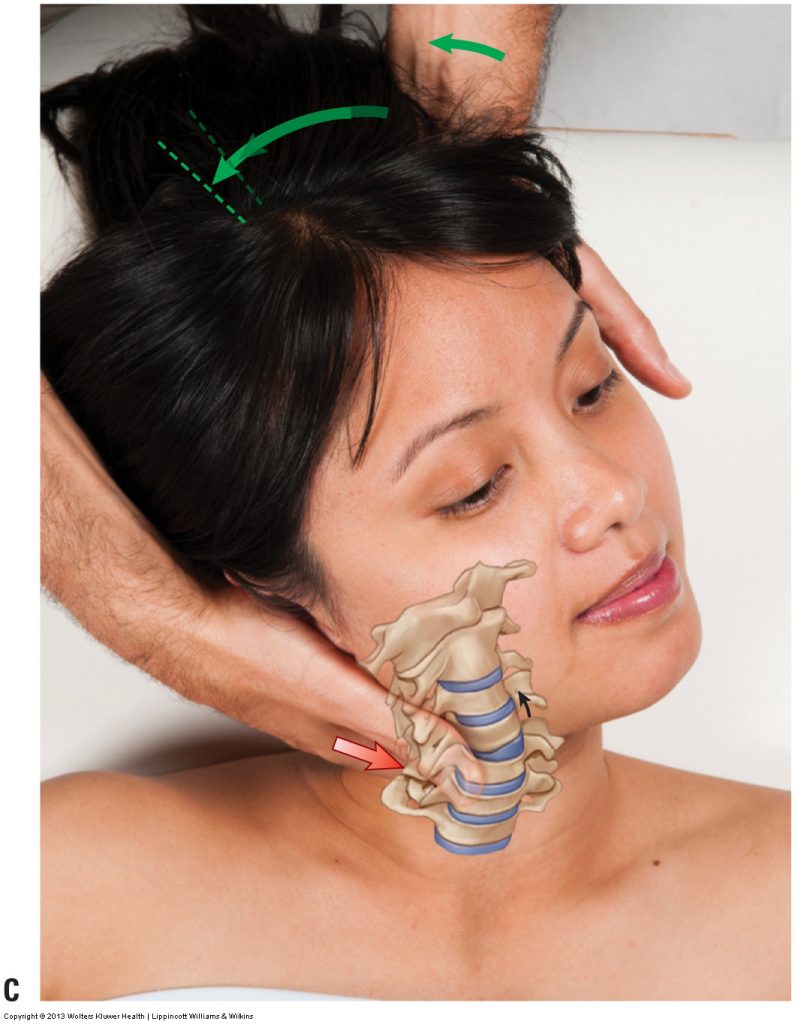
Cervical spine joint mobilization. Permission Joseph E. Muscolino.
Advanced Treatment Techniques for the Manual Therapist: Neck (2013).
Methods
Three male subjects were placed in the prone position with the thoracic skin exposed. The posterior thoracic region was loaded with perpendicular forces, incrementally from 125.3 N to 392.9 N. A force was then applied in the cephalad direction (in other words, a shear force was applied somewhat parallel to the underlying bony contour). The applied forces were measured using an infrared camera. Chiropractors then performed actual thoracic manipulation to determine if they could maintain their location of contacts (spinous process/ transverse process) on the underlying vertebra.
Results
The authors found that shear forces placed into the body over thoracic vertebral processes did not result in movement of the underlying bone. They concluded that skin-fascia interface over the thoracic spine exhibits negligible friction, so that during thoracic spinal manipulation, the practitioner cannot direct a force vector to a thoracic vertebra at a given angle by simply directing their thrust in that direction. The application of this study would seem to indicate that only perpendicular forces into bone can effectively move the bone.
The authors also listed various limitations of the study, and provided a caution when applying the findings of this study to other areas of the spine or during other manipulative procedures.
However, some people have taken this small study as definite theory for the application of the frictionless theory. Greg Lehman shows in a youtube video how this theory would be applied to manual therapy. He shows that to open a sliding glass door, one cannot slide their hands along the glass (in effect, a shear force) to move it because if there were no friction, then the force applied would simply slip and slide along the glass instead of transferring that force into the glass to move it.
However…
However, the “absolute” manner in which this concept is sometimes applied might not be 100% correct for the following four reasons:
- First, the application of this theory would be true only if the surface interface is 100% frictionless, which a later study (see below) would seem to contradict.
- Second, once the slack has been entirely removed by moving the skin-fascia tissue along the bone at the skin-fascia interface with the bone, then the therapist’s pressure should translate through the skin-fascia tissue layer and translate to the underlying bone. And regardless of the friction/frictionless aspect of the interface, if there is no longer any ability for the skin-fascia layer to move (in Greg Lehman’s video this would translate to his hands having no further ability to slide along the glass – after all, there must be some limit to this movement), then the force must continue to travel through the skin-fascia tissue to the underlying structure, in other words the bone. How much force translates through should be a component of the oblique force that is perpendicular (see next section).
- Third, the movement in the video along the glass is shown as being perfectly parallel to the glass. However, if the force is applied obliquely, in other words anywhere between perfectly perpendicular and perfectly parallel, then the force of that oblique direction could be resolved (resolution of vectors) into the perpendicular force and a parallel force. Whatever % of the force is perpendicular should be able to be transmitted into the bone to move/mobilize it. Let’s expand on this idea for a moment. The argument seems to be that a perfectly perpendicular (perfectly compressive) force , in other words a force oriented 90 degrees to the contour of the underlying bone, requires no friction at the skin-fascia interface with the bone to be able to move/mobilize that bone. But what if the direction of the force instead of being 90 degrees were 89.9 degrees. Would all force to move the bone be lost because of this change of .1 of a degree as this argument seems to state? How about if the direction were 89.5 degrees? Or 88.6 degrees? Or 82 degrees? Or 77 degrees. Or 69.437 degrees? My point is that it would seem very unlikely that any there is any threshold that would cause the effective force to move the bone to suddenly drop to zero. Instead, if would seem much more likely that there is a gradual diminution of force applied to move the bone as the component direction of perpendicular force decreases and consequently the component direction of parallel (shear) force increases. The point here is that any obliquely oriented force has a component that is perpendicular and a component that is parallel. Whatever the perpendicular component is should be able to be applied against the bone to move/mobilize it. The all or nothing argument espoused by some seems to be clearly impossible. They use extremes to make a point, but then paint the entire spectrum with the extreme.
- Fourth, once the slack of the superficial skin-fascia tissue is taken out, then the tension in that superficial tissue would have to be exerted onto underlying deeper structures at their attachment sites. If these attachment sites are anywhere along that bone, then the force would be transmitted into the bone. To be fair, this transmission of force is indirect, which is briefly mentioned in the video as possible, but it is passed over much too quickly.
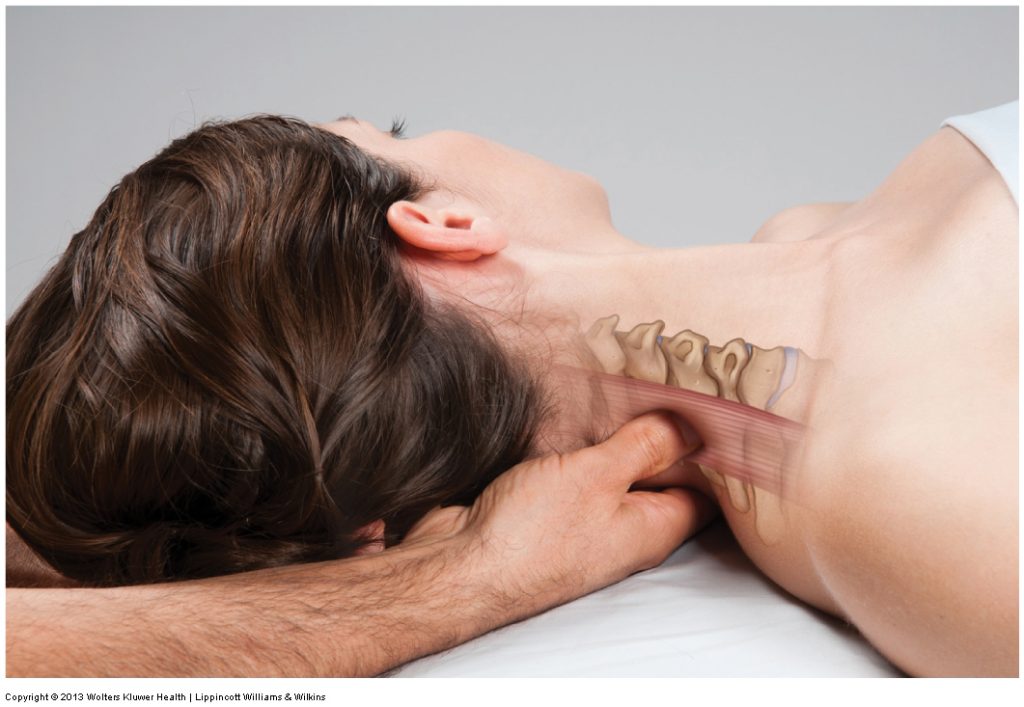 Application to Soft Tissue Manipulation (Massage)
Application to Soft Tissue Manipulation (Massage)
The authors in the paper also suggested that in soft tissue massage, the practitioner, in some instances, determine the direction of muscle fibres and then apply a stripping type motion to stretch one attachment of the muscle away from its other attachment. This study seems to indicate that this cannot be accomplished due to the frictionless nature of the soft tissue interfaces. However, this does not make sense. In fact, in Greg Lehman’s youtube video, he makes the argument that what moves the bone is the skin being tractioned, which he states attaches to bone on the other side of the joint; therefore the traction in the skin is what pulls on and moves the bone. But skin does not attach into bones. Between the skin and the bones would be facial layers, and if the argument that the interface between the skin and the fascia is frictionless, then it would not be possible for this tension force in the skin to actually translate to and pull on the bones. So by Greg Lehman’s own argument in the video, if tractioning the skin can move bones, it must mean that there is friction between the skin and the fascia deep to it (and in other videos, Greg Lehman propose that not only is it impossible to translate an oblique force into underlying bone, but it also impossible to translate an oblique force into a muscle to tension it because of the frictionless interfaces between skin and underlying tissues). However, as the following 2014 American study and the 2016 Canadian study show, forces do transmit between the skin and deeper fascial layers, so these interfaces are not 100% frictionless! Hence, it is possible for manual therapy/massage to transmit force into superficial and deeper myofascial tissues to tension and move them.
The 2014 American Study
This study was in the context of osteopathic techniques, which usually involve compressive (perpendicular) and tangential (shearing) forces to target the fascia. These forces are transmitted to the skin and adipose tissue before the fascia is encountered. The authors calculated using a mathematical model the extent of deformation of these two tissue layers relative to the fascia.
Based on a mathematical model, the authors found that the compression and shearing forces required to produce a deformation of 9% compression and 4% shear for the skin (the most superficial layer) were 50 N and 11 N, respectively. For adipose tissue (the second layer), these forces were 36 N and 8 N, respectively. Whereas for the underlying fascia (the deepest of the three layers), compression and shearing forces of about 100 N and 22 N were necessary for a similar deformation.
What does this mean?
The authors concluded that the forces applied to the surface of the skin WERE transmitted through the skin and adipose into the fascia. What is most important here is that the “shearing” force did transfer from the skin to the fascia. Or at least a component of its force did. More force was necessary for the same shear deformation of the fascia compared to the skin to occur (22 N compared to 11 N), but the force did transfer to the fascia.
2016 Canadian Study
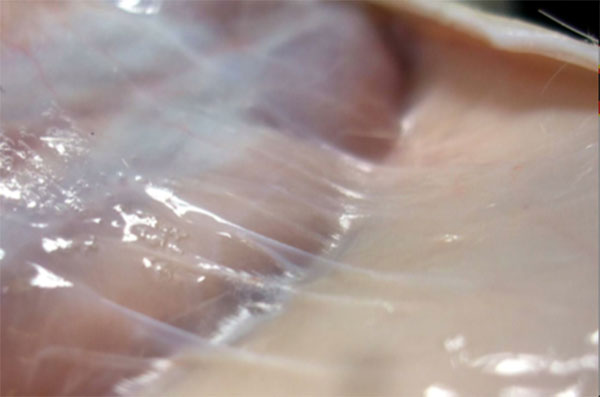
Subcutaneous fascia
A study from Ontario, Canada aims to clarify how loads due to manual therapy are transmitted into deeper tissues of the body. This investigation monitored tissue displacement at sequential depths in thoracic paraspinal tissues parallel with surface load directions (in other words, shear forces).
Now with an advanced ultrasound technology, this study addressed limitations of the 2002 study, which suggested that during a load, only pure perpendicular compression force is transmitted deeper into the body into the bone.
Twenty-four healthy participants were prone and manual therapy shear forces were applied to the body. Ultrasound speckle tracking synchronously monitored displacement and shear deformation of tissue layers in a region of interest adjacent to load application to a depth of 4 cm. Cumulative and shearing displacements were quantitatively estimated. The results show that the cephalocaudal cumulative displacement in layers parallel to the surface were, in order of depth, 1.27, 1.18, and 1.06 mm, respectively.
What Does This Mean?
Shear forces placed into the body DID transmit into deeper tissues. As with the 2014 American study, the shear displacement was less in the deeper tissues than in the superficial ones (1.27mm most superficially compared to 1.06 deeper), but this would be expected as forces applied to the body would be expected to dissipate as they travel deeper into the tissues of the body. Therefore, it is reasonable to assume that these forces could plausibly affect underlying bones (spinal vertebrae, which were examined in the 2002 Canadian study).

Subcutaneous fascia. Permission Joseph E. Muscolino. www.learnmuscles.com. Originally published in a massage therapy journal article: fascial structure (spring 2012).
How Might This Force Transfer Occur?
Displacements of tissues most likely arises passively, consistent with load transmitted by the retinacula cutis and epimuscular force pathways. “Retinacula cutis” is a complex of fibrous structures that traverse the subcutaneous fat linking the skin to the deep fascia and capable of transmitting loads from multi-directional forces (in other words loads that are not perfectly compressive/perpendicular).
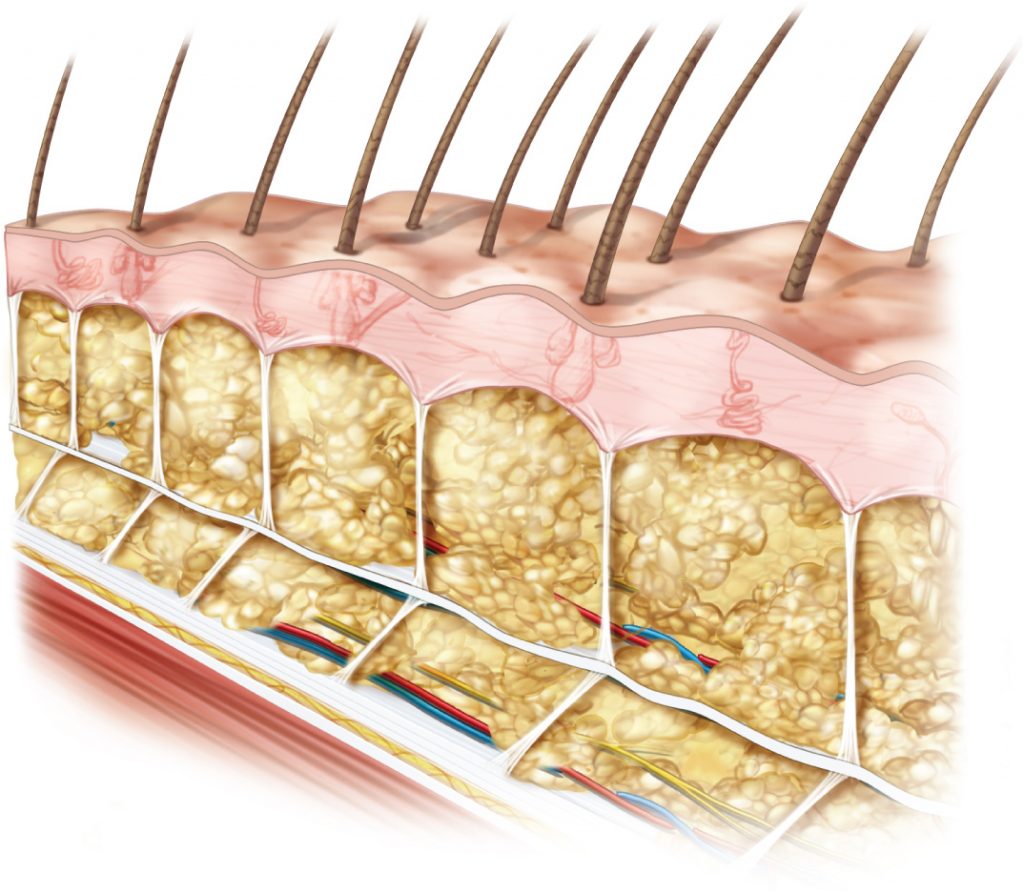
Shearing of subcutaneous fascia. Note the tension in the deeper retinacula cutis fibers. Permission Joseph E. Muscolino. www.learnmuscles.com. Originally published in a massage therapy journal article: fascial structure (spring 2012).
So What Does This All Mean?
It would seem that taking any theory or ideology too far is dangerous. Certainly, the interfaces of soft tissues of the body are quite slippery, in other words, have very little friction. After all, they are meant to be sliding surfaces. It is also worth keeping in mind that the skin examined here functions as just one mechanical layer among several, yet as the body’s largest organ it carries clinical concerns of its own that fall well outside manual therapy, which is why conditions affecting its surface are assessed and treated by dermatologists in Salt Lake City, Utah and other regions. However, they are not perfectly frictionless, so oblique forces (that are not perfectly perpendicular) can transmit into deeper tissues. Further, as stated above, the oblique force should be able to be resolved into its perpendicular (compressive) component, which would grab and move underlying tissue. And once the slack of the more superficial tissue has been removed, then the therapist’s force should be able to penetrate through the superficial tissue into the deeper tissues. And that superficial tissue being tensioned should transmit that tension into the underlying structures, likely the underlying bone, via its eventual (direct or indirect) attachments into the bone. Certainly, the magnitude of the force transmission does decrease as it travels deeper into the body, but it does transmit. So we should not have, as proponents of frictionless theory state, an “all or nothing” world of soft tissue force application wherein if the force is not perfectly perpendicular to underlying tissues/structures it will have zero ability to affect the underlying tissues of the body.
This blog post article was created in collaboration with www.TerraRosa.com.
(Click here for the blog post article: What is Joint Mobilization.)