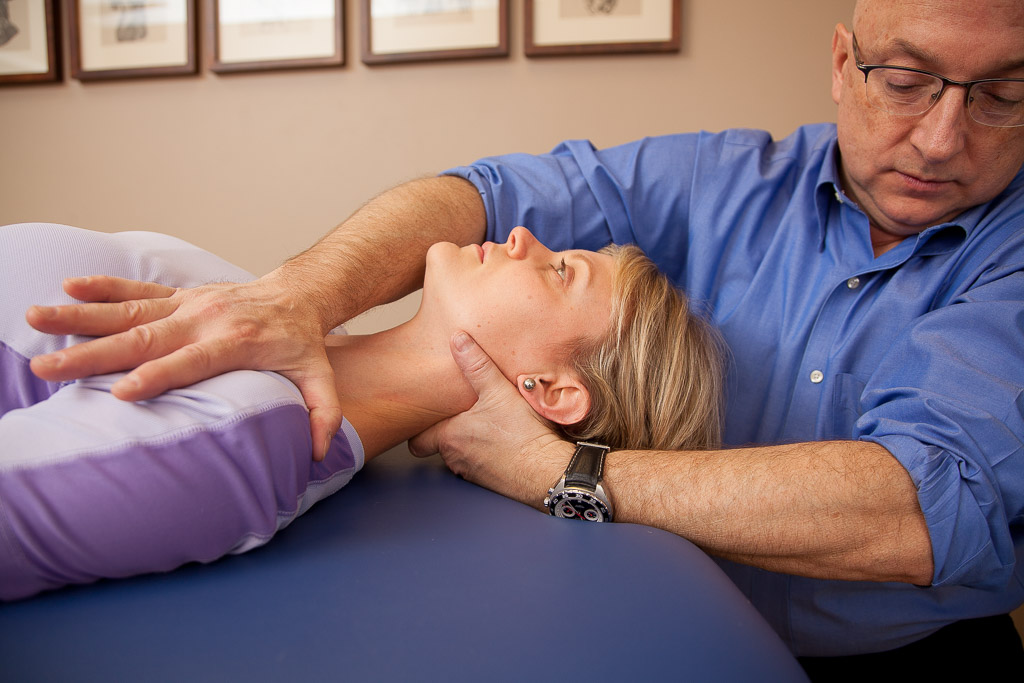
Walt Fritz, Physical Therapist and Manual Therapy Continuing Education Instructor. Permission Walt Fritz.
The following is an extended interview that was held by Terrarosa.com.au with Walt Fritz, renowned physiotherapist (physical therapist), myofascial release therapist, and manual therapy continuing education instructor. Walt talks candidly about how he began his Foundation of Myofascial Release Seminar, and the challenge to break away from the unproven narratives held dearly by many, which branded him as a heretic by some… and why “because it works” is no longer good enough for him as a rationale for the efficacy of manual therapy work.
When and how did you decide to become a bodyworker?
After a few false starts at university, I shifted my sights toward physical therapy, graduating from the University at Buffalo (NY) in 1985. In theory, physical therapy includes bodywork/manual therapy, there is often little resemblance to what I now do. I would have never predicted that I would be a continuing education educator, as public speaking was not my strong point. In 1992, I began my first few continuing education seminars in myofascial release (MFR) and craniosacral therapy (CST) and I was hooked. I was so impressed with the changes that I could make in my clients, even after only one weekend seminar, that I took all of the classes I could and spent the ten years instructing at myofascial release seminars for another teacher (John Barnes). John is well-regarded by many in the manual therapy community, but we no longer saw eye to eye on many things and it was time to move on. After we parted ways, I slowly began my own line of myofascial release workshops, the Foundations in Myofascial Release Seminars, in 2006.
So, you began to develop your own work?
At first, my workshops closely resembled the MFR I was taught but, over time, I reflected upon why I chose to leave my original training/teacher and began to craft my workshops with my own vision of providing less of a new-age driven experience and utilize the best available science to explain all aspects of the work.
Removing myself from my original peer group of MFR therapists, I had a chance to sample many of the explanatory narratives other manual therapists had shared with me. While immersed in a closed culture of any sort there is little exposure or acceptance of conflicting/contrasting views. I was having great success with the MFR I was taught, but began to understand that the supposed science presented in those workshops had little credibility or understanding beyond that peer group. Results were proof enough in my MFR family (and in most other modality groups) but this can lead to post hoc reasoning errors. I have success so the story I was taught and retell myself as to the “why” must be true. Once I left that MFR group I saw that most every modality line had similar claims of success, each laying claim to being the most effective/efficient modality for pain. “They don’t know what we know, so science be damned; they will catch up to us eventually” was a phrase often repeated in my trainings and those are pretty heady concepts to believe, but I did. I’ve gotten a lot of public flack since I left my MFR community over 10 years ago, many feeling I was disrespecting my teacher/mentor and criticising other MFR therapists who still follow that model. Those statements cannot be farther from the truth but are believed as fact when repeated frequently enough. I have gratitude to those who taught me the wonderful things I can do with my hands, though I now realize those things are probably not accomplished for the reasons I was taught.
Permission Walt Fritz
What do you find most exciting about bodywork therapy?
Simply put, it is being able to help those who others were not able to help. I love being able to positively influence the lives of others, whether it is my clients or the therapists that I teach. I find it exciting that so many therapists are following paths such as mine, seeking more accurate and inclusive explanatory narratives to explain the effects of a manual therapy engagement. I always found it odd that every modality pushed an agenda of tissue-specific effect, or tissue-specific pathology (real or metaphoric pathology), but all are simply touching the skin. While I do not rule out potential evidence to come in the future, I see most of those tissue-specific models as lacking full validation. This may sound odd coming from an MFR practitioner and educator, but I continue to refer to my work as MFR due to the hands-on actions I’ve done with my hands for over 25 years, rather than feeling I need to fall in line behind one or more of the traditional, historical fascial narratives.
What is exciting to me is the realism that bodywork/manual therapy is not the only means of reaching people for their pain or movement dysfunction. Exercise and education are often crucial aspects of positive outcomes. But I now understand that a patient’s beliefs also drive the possible outcomes of our interactions. If a patient comes to me for therapy (I’m a physical therapist) and is expecting me to teach them extensive exercises and hammer into them beliefs about the need for core strengthening and postural improvement, I may sadly disappoint and not be able to help them as much as another patient who feels they would benefit most from a touch-based, manual therapy approach to get at what others have missed. But when my patient’s beliefs and expectations resonate and align with what I can offer, that is the magic of our work.
Permission Walt Fritz
What is the most challenging part of your work as a physical therapist?
As a physical therapist in private practice, I have many obstacles to overcome in dealing with stereotypes of just what physical therapy is. In many ways, massage therapists have it easier. A touch-based, bodywork-centered approach is what new clients expect, even though the modality and delivery may vary. Trying to move to more symptom-specific work is not always easy for the massage therapist. Mention physical therapy to the average person and their vision is very different than the way I practice. It is a pleasant surprise to most new clients, as they are not used to being touched and given so much one-on-one treatment by their physical therapist. But others may expect to be told their posture, weak core, or overall lack of physical exercise is the reason they have pain and expect to be given remedial exercises, postural training, etc. to address these problems. The scientific literature leaves little doubt that movement is one common denominator when aiding someone in reducing their pain, but movement takes many forms. A person in pain often comes in stating things, such as, “My back pain makes me feel so weak”. The therapist may even perform manual muscle testing (with rather poor levels of reliability) and find that the person is indeed weak, at least according to their tests. But are they testing a movement or muscle group that is truly weak/deconditioned/inhibited and is the root cause of pain, or are they asking a person in pain to resist the therapist’s testing in a movement that hurts? Exercise, one of many forms of movement, often helps the pain and the person will even feel and test stronger when the pain dissipates, validating the therapist’s beliefs, but probably one of many post hoc reasoning errors we easily make. It is challenging to deal with these sorts of beliefs. Movement is beneficial, whether it takes the form of strengthening or dancing. To many, being given the ability simply walk is the movement or exercise that helps to complete the circle of wellness, and I feel blessed to be able to play a part in that process.
And the challenges as an educator?
As an educator, I see one my greatest challenges are attempting to break down the walls between the deeply seated beliefs and narratives set forth by others in our (fascial) field. If one spends time on social media, reading comments from therapists and advertisements from continuing education educators, the claims are dizzying, with each modality claiming overall superiority with the only measurement being the popularity of that brand of manual therapy. I/we are easily sold on modality claims, all seeking the holy grail of therapy. I’ve taken as a personal and professional challenge to educate therapists that there are universal aspects of our work, despite claims to the contrary, which make us able to reach our patients through simple concepts of pain science and safe touch. I was and still am regularly challenged to remove the words myofascial release from my course titles, as some feel that releasing the fascia is biologically plausible and others feel my heretical views should cause me to stop using the words and concepts that they hold dear. Having push back from both extremes tells me I am on to something, if so much emotion can be generated from both sides of the fascia belief spectrum.

Permission Walt Fritz
What makes your Fundamental Myofascial Release Seminar unique?
I use the hands-on actions of myofascial release, embedded in what I believe to be a more plausible and inclusive model of potential physiological/neurophysiological action to reach my students and patients. In some ways, I am using the words myofascial release metaphorically, using them to represent the actions I do with my hands, rather than the belief that we are singularly and specifically impacting fascia to the inclusion of all else. I know that much of what I teach and believe conflict directly with many of the beliefs and teaching of those in the fascia field, but diversity of thought is good and keeps us strong. No one has all of the answers, but we get closer each day.
I start my class exploring some of the possible limitations of the various fascial explanatory narratives and then try to build a simple, inclusive model, one that acknowledges the possibility of tissue-specific change, but also acknowledges the neurological and contextual factors inherent in our work. Understanding neurological possibilities opens the door for exploring new or different interventions.
I teach a form of myofascial release recognizable by its physical appearance as similar to what many learn and teach. But the keystone of my approach is utilizing a patient-directed, feedback loop driven model of evaluation and treatment. I see too many therapists relying on their experience, vast continuing education training, and self or externally ascribed intuitive abilities to determine what is at fault and what is needed in treatment. They may think they are including patient feedback in the equation, but not to a degree that I feel is safe. I teach and work from a perspective that strongly values and demands patient feedback to direct treatment. When was the last time you asked a patient, “is this stretch/pressure replicating a familiar experience” or “does this stretch feel like it may be helpful/useful?”. I would guess that it does not happen all that often.
My Foundations Approach comes from a unique perspective of teaching the therapist to apply greater value from patient input and feedback. We spend the entire workshop learning these principles, all wrapped up in an MFR blanket of techniques. MFR has great effect. Studies seem to confirm this, at least the things that we do with our hands that we call MFR. Most of these efficacy studies, however, harken back to the old, historical narrative of facial change to explain why MFR works, without ever examining these beliefs. Are we really able to singularly and specifically isolate fascia as the source of pain/movement dysfunction and then selectively target it, to the exclusion of all other tissue/nerves/the brain to create change? To that I am quite uncertain.
What is your most favourite bodywork book?
Just one? Netter’s Atlas of Human Anatomy might be one of them. The artistry is magnificent and every time I pick it up I am amazed just how well we function given the complexity of our body and brain. It is also one of my favorite teaching tool for clients. I always find it interesting how the various manual therapy professionals seem to learn from only one part of an anatomy/physiology book. If muscles were stressed in your training or continuing education, then all problems are explained and addressed from this muscle-based perspective. Fascial therapies are not different, which is testament to the newer fascial anatomy texts that have been recently published. None are totally inaccurate, in fact they show fascia to greater detail than ever pictured. But if you are presenting a segmented view of the body you are invariably overlooking the interaction of all of the parts. Netter’s may be a really nice way to move back from the ledge of tissue-specific beliefs and into a more wholly integrated view of the body. I again realize I am writing words which will cause disagreement, as fascial therapists often believe and state that they are working with the forgotten tissue. Unfortunately, that only serves to once again artificially, and inaccurately, elevate one tissue to a position of greater importance than the rest of the body.
How do you see the future of bodywork and massage therapy?
I believe that the science-based approach to bodywork will continue to spread, replacing unfounded modalities and approaches. Therapists will need to keep up with the changes or get left behind. Massage schools will need to better address this science and continuing education will need to keep pace as well. “Because it works” and post hoc reasoning errors will no longer be good enough. And I hope that I am able to leave my imprint on the manual therapy community by moving us toward a less ego driven model and into patient driven/directed models.
Walt Fritz, PT
Pain Relief Center and Foundations in Myofascial Release Seminars
Rochester, NY, USA
(Click here for a blog post article on pain neuroscience.)