Signs and symptoms:
The first and most reliable sign of patellofemoral syndrome (PFS) (also known as chondromalacia patella) is roughness on the underside of the patella, which can be palpated when resistance is given to contraction of the quadriceps femoris musculature. Depending on the degree of severity of the condition, pain may be experienced by the client/patient. When pain is felt, it usually is experienced deep in the joint. It might be dull or sharp in quality, and it usually occurs during the gait cycle, especially when running/walking downhill/downstairs. Swelling around the patella might also occur if the condition is severe and/or aggravated.
Assessment/Diagnosis:
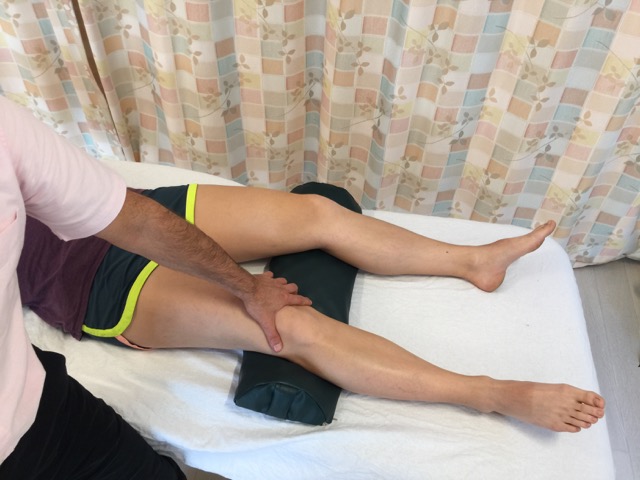
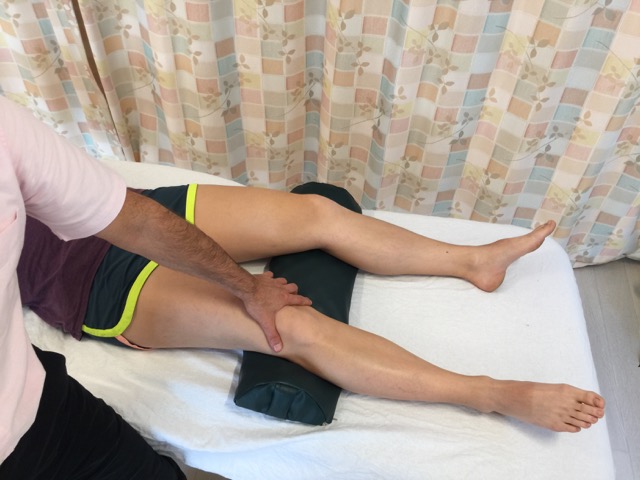
Patellofemoral syndrome can be easily assessed/diagnosed during the physical examination by employing the orthopedic assessment test known as patellofemoral syndrome test. Have the client/patient supine and cup your thumb web around the superior/proximal pole of the patella. For the first repetition, ask the client/patient to slowly contract their quadriceps with mild to moderate strength; as the client contracts the quadriceps, allow the client’s patella to track proximally with no resistance. For each successive repetition, incrementally add slightly more resistance to the patella in the distal direction, preventing it from tracking proximally; it is important to increase the resistance only a small amount each time. By the last repetition (approximately four to five repetitions are done in total), your resistance should equal the strength of the client’s contraction so that no motion of the patella occurs. With increased resistance, the patella is forced down against the femur, increasing the compressive and friction forces upon the joint surfaces. For this reason, it is extremely important that the client contracts slowly and with mild to moderate strength at most; this test can become increasingly uncomfortable/painful as the resistance increases. This test is considered positive if joint crepitus is felt or heard, or if the client experiences pain. Note: Once crepitus has been felt and/or the client has experienced pain with this test, it is not necessary to perform further repetitions with stronger resistance.
Simply directing anterior to posterior compression against the patella, perhaps also moving the patella proximally and distally while maintaining this pressure (again, the pressure should be applied slowly and with mild to moderate force at most), might also elicit pain. Patellofemoral syndrome might also show swelling around the patella.
Patellofemoral syndrome is often present without the presence of pain. Like osteoarthritis in other areas of the body, it can be present for years or decades without pain. However, as it progresses and become more severe, pain is more likely to occur. During verbal history the client/patient will often describe the presence of pain, especially when walking downstairs/downhill. Because patellofemoral syndrome is an osteoarthritic condition, it can also be definitively diagnosed with X-Ray radiographic examination.
Differential assessment:
The assessment of patellofemoral syndrome is straightforward and simple; crepitus and/or pain with the patellofemoral syndrome test is pathognomonic for patellofemoral syndrome; in other words, a positive result is definitive for patellofemoral syndrome. However, given that patellofemoral syndrome usually requires decades of use/overuse to develop, the physical stresses that caused patellofemoral syndrome might have also contributed to the development of other knee joint conditions. Therefore examination should not stop when a positive finding with patellofemoral syndrome test is found. It is important to rule in/out other knee joint conditions such as meniscus tear or spasm of surrounding musculature.
Further, if patellofemoral syndrome is found, then it is important to assess all conditions that could cause or contribute to patellofemoral syndrome. Amongst these are weakness and/or tightness of the quadriceps femoris musculature. Because patellofemoral syndrome is so often caused by dysfunctional patellar tracking, it is important to assess for this condition as well. With the client/patient supine and the knee joint extended, ask the client/patient to contract their quadriceps femoris musculature and observe the motion of the patella; deviation during the tracking motion is subtle, but should be looked for. And, if patellofemoral syndrome is found and dysfunctional patellar tracking is found or suspected, it is also worthwhile to check for all the conditions that can cause dysfunctional tracking: genu valgus, overpronation of the foot, weak hip joint abductor or lateral rotation musculature, and tight adduction or medial rotation musculature. And any involved musculature should be assessed for the presence of myofascial trigger points.
Finally, because patellofemoral syndrome is a joint dysfunction, it is important to perform joint motion palpation by gently challenging all glide motions of the patella, feeling for adhesions and looking for restrictions in motion.