Introduction
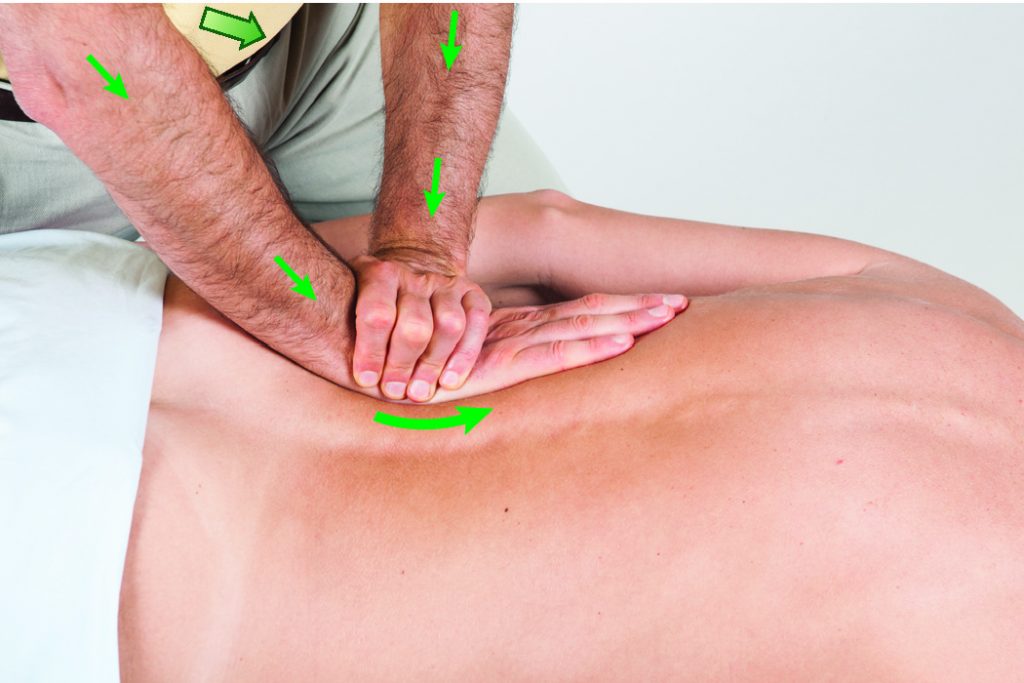
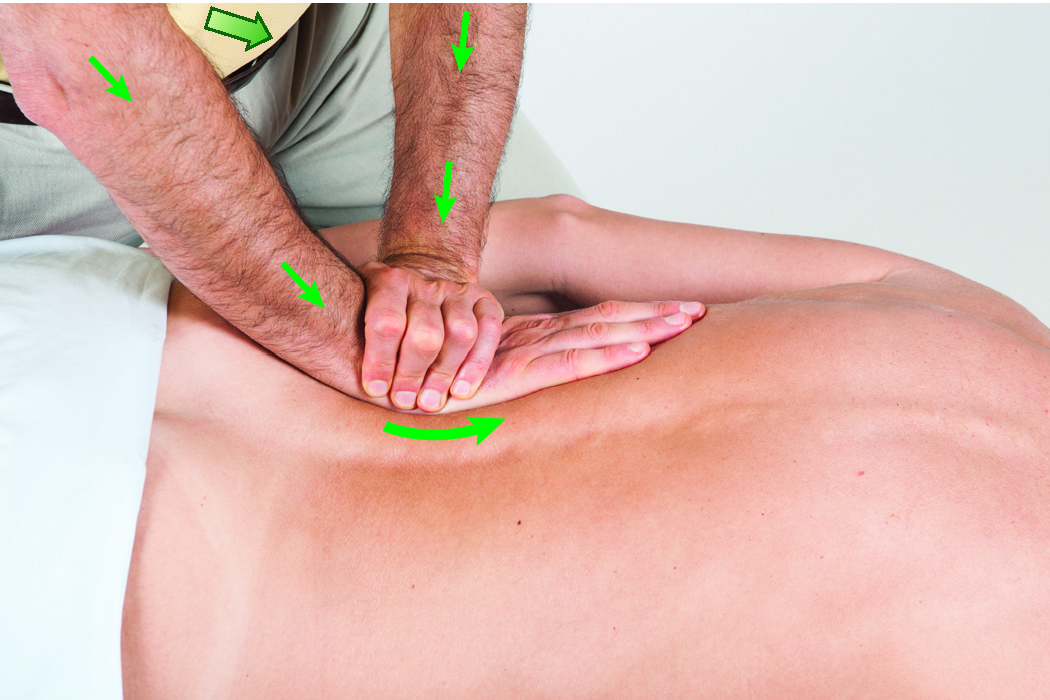
Supported flat palm contact to the paraspinal musculature of the low back. Permission Joseph E. Muscolino.
Manual Therapy for the Low Back and Pelvis – A Clinical Orthopedic Approach (2015).
The American College of Physicians (ACP) has recently published clinical recommendations on non-invasive treatment of low back pain such as massage and other manual and movement therapies based on current evidence consisting of a review of more than 150 studies.
Published in the April 2017 issue of Annals of Internal Medicine, a committee from ACP conducted a systematic review of randomized, controlled trials and systematic reviews published through November 2016 on non-invasive pharmacologic and nonpharmacologic treatments for low back pain, such as massage and other manual and movement therapies.
The guideline provides the following recommendations:
Recommendation 1:
Given that most patients with acute or subacute low back pain improve over time regardless of treatment, clinicians and patients should select nonpharmacologic treatment with
superficial heat (moderate-quality evidence), massage, acupuncture, or spinal manipulation (low-quality evidence).
If pharmacologic treatment is desired, clinicians and patients should select nonsteroidal anti-inflammatory drugs or skeletal muscle relaxants (moderate-quality evidence). (Grade: strong recommendation.)
Recommendation 2:

Exercise on a gym ball. Permission Joseph E. Muscolino.
For patients with chronic low back pain, clinicians and patients should initially select nonpharmacologic treatment with exercise, multidisciplinary rehabilitation, acupuncture, mindfulness-based stress reduction (moderate-quality evidence), tai chi, yoga, motor control exercise, progressive relaxation, electromyography biofeedback, low-level laser therapy, operant therapy, cognitive behavioural therapy, or spinal manipulation (low-quality evidence). (Grade: strong recommendation.)
Recommendation 3:
For patients with chronic low back pain who have had an inadequate response to nonpharmacologic therapy, clinicians and patients should consider pharmacologic treatment with nonsteroidal anti-inflammatory drugs as first-line therapy, or tramadol or duloxetine as second-line therapy. Clinicians should only consider opioids as an option in patients who have failed the aforementioned treatments and only if the potential benefits outweigh the risks for individual patients and after a discussion of known risks and realistic benefits is had with patients (moderate-quality evidence). (Grade: weak recommendation.)
Importance?
Robert Shmerling, MD from Harvard Health publishing wrote:
“These new guidelines endorse an approach to treating a common ailment that only a few years ago would have seemed outrageous. The remedies recommended are not brand new; but discouraging medication use as an initial step is a big departure from prior recommendations.”
“Medical practice rarely changes right away, and these guidelines may have relatively little impact in the short run. But I would not be surprised if non-pharmacological treatment of back pain becomes the norm over time. Many of my patients already seek out these treatments regardless of whether I recommend them. After all, the “usual” medications for low back pain are not all that effective and often cause trouble. It’s time we recognize that there are other, better ways to help.”
Conclusion
This might seem like a small step, but ideologically this is a very large step in that the medical world is finally beginning to recognize the efficacy of the therapeutic value of massage therapy and other manual and movement therapies in lieu of pharmacologic drugs.
This blog post article was created in collaboration with terra.rosa.com.au.