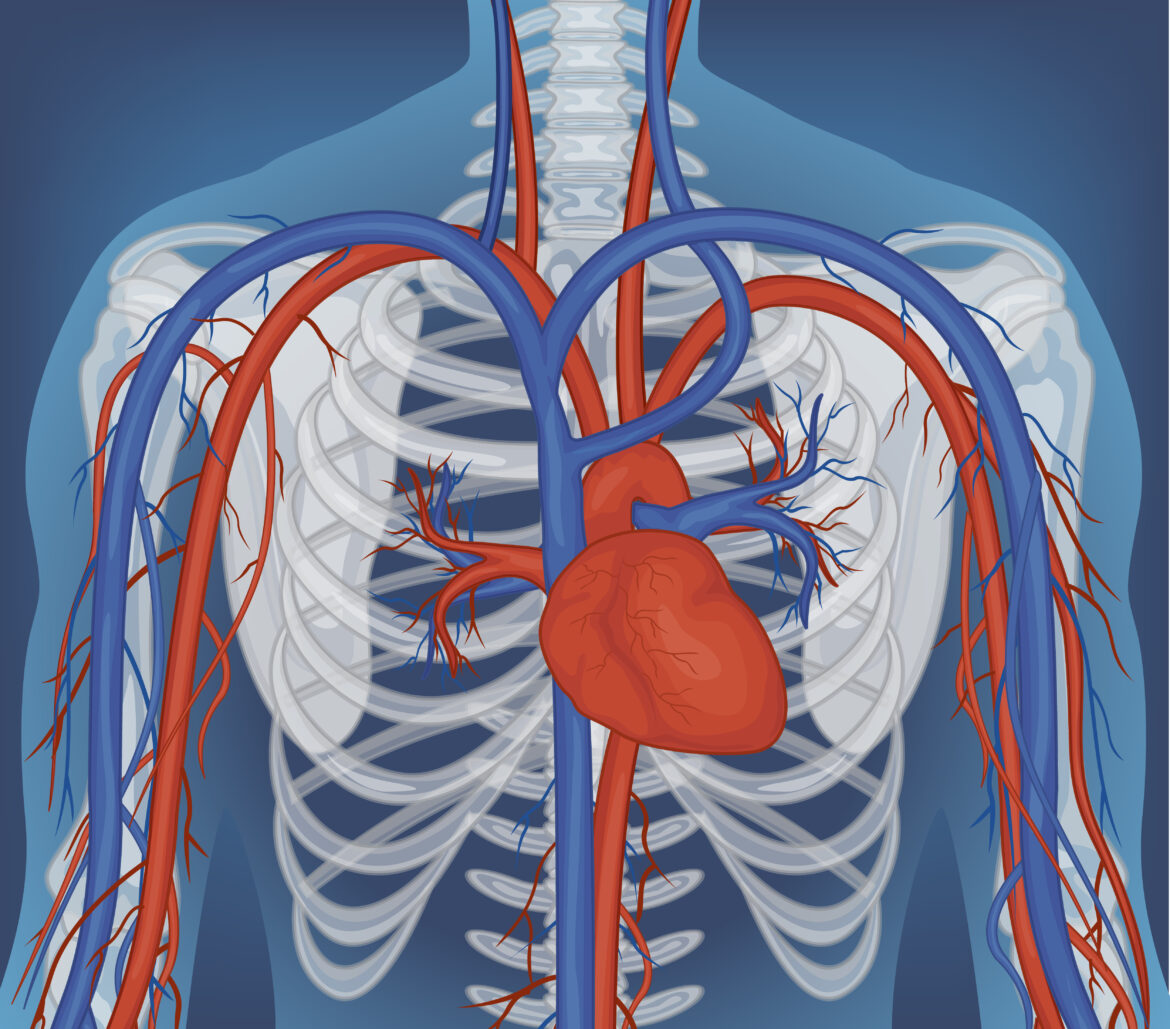
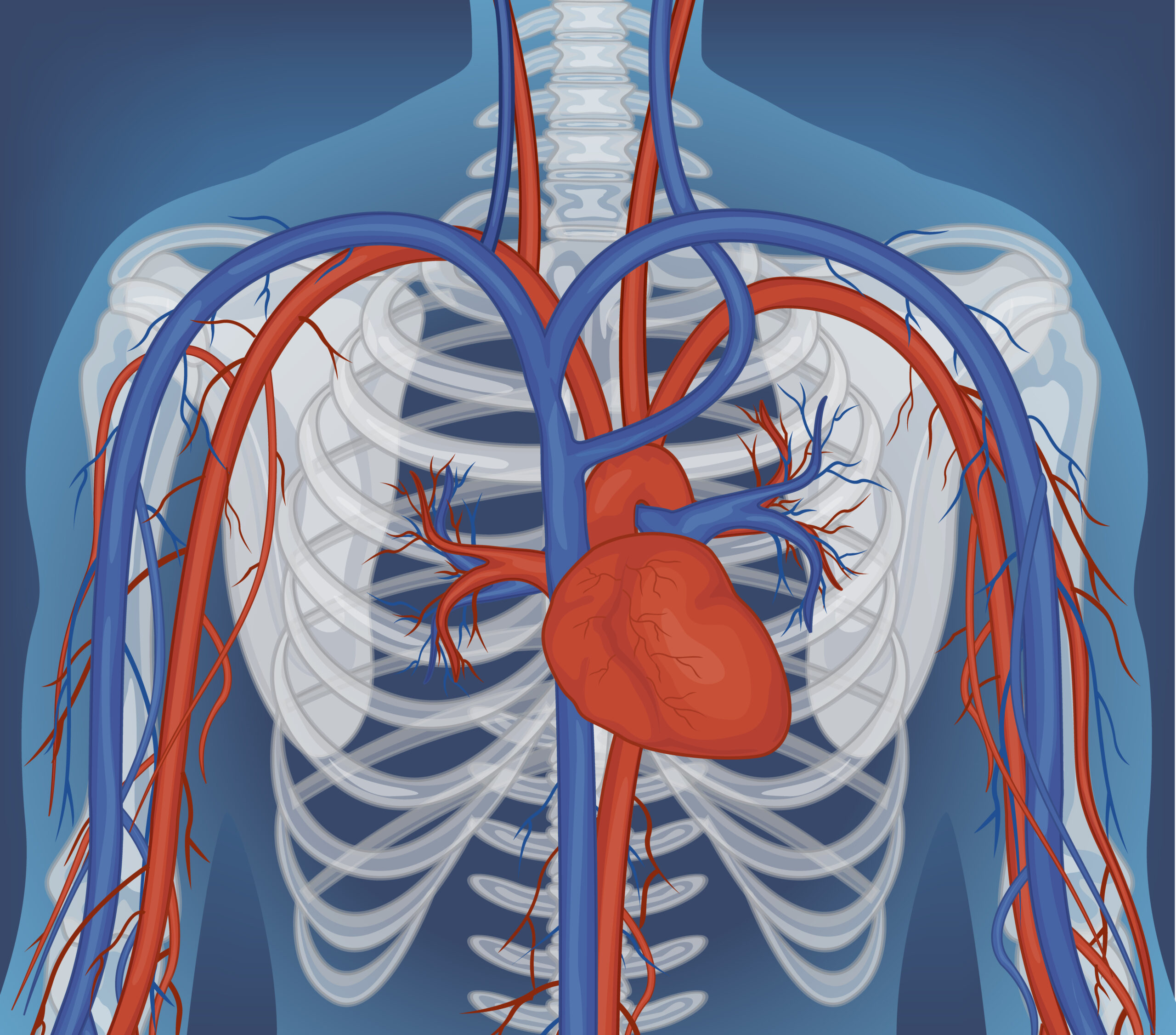
You may have heard that the circulatory system is a flow tube that pumps blood from the heart, through the arteries, making the blood flow, and then back through the veins to the heart. However, the veins do not return blood to the heart by simple passive flow; the skeletal muscle in our bodies is primarily responsible for returning blood from our legs to the heart. To return blood to the heart against the upward pull of gravity, it requires high pressure contractions of muscles surrounding the deep veins. Specifically, the calf muscles have a function of the muscle squeezing the blood in order to pump it up against gravity to the heart. This peripheral pump is essential for the circulatory system to function.
For manual therapists, movement educators and anybody else who gets their clients/patients/players to use their musculoskeletal system it would be useful to understand the consequences. The veins rely on the muscles for function and if they decline then it is likely the veins will follow.
The Calf Muscle Pump: Anatomy of Venous Return
The deep veins of the lower leg run through the muscle compartments of the leg. The posterior tibial, peroneal and anterior tibial veins run alongside the deep muscles of the lower leg, linking with the muscles (including the deep portions of the gastrocnemius and soleus muscles). Many connections exist between these veins and a number of venous sinuses within the soleus muscle. The soleal venous sinuses are large, thin walled structures that act as reservoirs of blood at rest, containing many times the normal venous blood volume.
When the calf contracts during walking, running, or any rhythmic lower limb activity, the muscle compresses these deep veins. Venous valves open upward and close downward, so the compressed blood moves toward the heart rather than flowing back down. The National Institutes of Health has published extensive material on the physiology of venous return, and the skeletal muscle pump is consistently described as the dominant mechanism for moving blood out of the legs against gravity (NIH on circulation).
Three anatomical facts matter for clinical practice.
- Venous valves are normally passive structures which require muscular contraction to open and function. In the absence of periodic contraction of the muscle to pump blood against back pressure, blood gravitates downwards and pools in the distal part of the limb.
- The soleus muscle accounts for most of the pump load and, with its large venous sinuses, is a major muscle involved in postural and locomotor activities of disproportionate importance to venous return.
- The ankle joint is part of the pump mechanism that contracts and relaxes similar to the gastrocnemius and soleus muscles. In efficient gait, the ankle needs to go up (dorsiflex) and down (plantarflex). An extremely powerful gastrocnemius or soleus may not be able to produce an equally powerful upland or downland contraction if the ankle joint is nonmobile or stiff.
In the healthy adult, the muscles, veins and blood vessels are arranged in a functional system that permits a person to walk for hours each day without developing painful swelling of the lower legs.
What Happens When the Pump Fails
When the skeletal muscle pump underperforms, venous blood stagnates in the lower legs. Over time this produces the clinical picture of chronic venous insufficiency, which includes leg heaviness, swelling, skin changes, and, at its most visible, varicose veins. The U.S. Centers for Disease Control and Prevention estimate that chronic venous disease affects roughly one in four adults, with prevalence rising sharply with age and with sedentary lifestyle (CDC on venous disease).
Pumps can fail for many reasons, many of which are relevant to musculoskeletal treatment. If muscles of the calf are not contracting for extended periods while standing or sitting, the venous circulation is bypassed allowing blood to pool in the soleal sinuses as well as the distal muscles of the lower leg.
Ankle restriction causes a person to loose dorsiflexion and therefore cause them to plantarflex, which restricts the ankle mortise, resulting in reduced mechanical compression of the lower calf muscles.
Effects on Foot Orthotics – Calf Muscle Weakness. Calf muscles that are deconditioned, atrophied or neurologically weakened will produce less compression per step than their more conditioned counterparts. Currently available exercises for the management of chronic venous insufficiency are unable to overcome incompetent venous valves, which typically fail within 5 to 10 years. When these valves fail, regardless of the underlying cause, whether because of chronic dysfunction of the associated pumping mechanism or thrombotic obstruction, the incompetent portion of the venous system becomes a zone of abandoment where blood can pool downward into it without any muscle activation of the calf.
Other body systems such as connective tissue, vascular tissue and muscle all go through age related tissue changes that can also affect the problem caused by cervical head pressure. These changes include loss of elasticity, decreased vascular wall strength, and decreased muscle strength. The causes of increased risk for venous insufficiency are additive and include factors related to habit, mechanical factors, muscle status and venous valvular status. As such, the “stuffy” ankles of the inactive office worker can be due to a combination of weak calf muscles and incompetent venous valves. It is not simply a cosmetic problem.
Why Manual Therapists Should Recognise Venous Dysfunction
When working with bodyworkers, a variety of presentations of venous dysfunction are demonstrated in the clients they treat, including older individuals, the sedentary and athletes recovering from injury to the lower limbs.
- Superficial varicose veins are visible on the skin’s surface and can be related to either the long saphenous or short saphenous veins.
- Reticular veins and telangiectasias of the thigh and lower calf. These can be removed with Ambulatory Phlebectomy, Laser Pitting or indentated oedema at the lower leg and ankle which disappears overnight.
- Hemosiderin staining and skin thickening in chronic cases.
- Calf heaviness or aching after prolonged standing. That changes things quite a bit clinically. None of these issues are within the manual therapist’s scope of practice as a treatable issue, but they do inform how a treatment session might be structured. For example, areas of the skin that are severely varicose would not be appropriate places to perform deep tissue work, brisk effleurage or firm petrissage.
- A history of DVT is an absolute contraindication to performing deep tissue work of the lower leg until cleared by a vascular specialist.
Even with mild venous disease, the manual therapist can play a vital role in supporting muscle tone and increasing range of motion of the ankle as well as addressing gait patterns that interfere with the function of the venous pump.
Movement, Manual Work, and Medical Referral
There is a three way partnership that serves clients with compromised venous function well.
Movement and exercise. The single most effective non medical method of improving compression and pump function is performing rhythmic activity of the calf muscles on a daily basis. Activities such as walking, cycling, performing calf raises and doing full range ankle movements (dorsiflexion and plantarflexion) can all increase venous return. However activities such as performing resistance exercises on the calf and ankle stabilisers can provide long term structural support.
The manual therapy for the ankle includes the release of the triceps surae (gastrocnemius and soleus) and deep posterior compartment (tibialis posterior) contractions in order to restore normal dorsiflexion of the ankle and enhance the pump mechanism. The manual therapy for the foot includes the release of the contraction of the peroneals, and the intrinsic muscles of the foot, as well as the tibialis posterior to release muscles that restrict venous return. The release of the posterior chain (gastrocnemius, soleus, and plantar fascia) increases the functional length of the contracted calf muscles and facilitates venous return.
The time for medical referral for structural vein disease is after failed veins due to valvular dysfunction or development of varicose veins. No amount of exercise or manual therapy will repair failed venous valves or alleviate painful varicose veins. Patients with such conditions require specialty care in vein management. Many of the traditional venous surgeries have been updated with less invasive alternatives including Endovenous laser therapy and radiofrequency ablation as well as ultrasound guided foam sclerotherapy. All of these procedures are performed in the Vascular Surgery and Venous center on an outpatient basis under local anesthesia.
A representative example is the specialty level assessment available at a vein clinic in Scottsdale or a comparable vascular centre elsewhere. What these clinics share is a specialty workflow built around duplex ultrasound diagnostics, physician led assessment, and minimally invasive treatment of symptomatic varicose veins. For manual therapists, recognising when a client’s presentation has moved beyond the scope of musculoskeletal intervention and referring accordingly is part of responsible practice.
Integrating the Muscle Pump into Everyday Practice
Several practical habits make the muscle pump central to musculoskeletal work with adult and aging clients.
- Assess ankle dorsiflexion early. Less than roughly 10 to 15 degrees of weight bearing dorsiflexion is a pump limiter as well as a gait problem.
- Palpate the posterior calf in standing and in partial weight bearing. Dense, restricted calves and sluggish fascial glide between gastrocnemius and soleus affect both mechanical output and venous compression.
- Screen for venous signs during intake. Visible varicosities, oedema, skin staining, and patient reported leg heaviness should all inform the session plan.
- Encourage everyday pump activation. Ankle pumps at the desk, hourly standing breaks, and short walks after meals all produce measurable improvements in venous return.
- Build calf conditioning into rehabilitation and maintenance plans. Bent knee and straight knee calf raises load the soleus and gastrocnemius differently and both are worth addressing.
- Refer appropriately when presentations suggest structural vein disease.
The underlying message is that the skeletal muscle pump is not a peripheral detail of lower limb anatomy. It is the primary mechanism by which blood gets back to the heart from the feet and lower legs, and it is structurally dependent on the muscles, joints, and movement patterns that bodyworkers spend their careers studying.
Conclusion
Venous return from the lower limbs is as much a musculoskeletal event as it is a cardiovascular event. The calf muscle pump involves the gastrocnemius and soleus muscles and the ankle joint, and is primarily controlled by muscle contraction. The influence of decreased muscle tone, reduced joint mobility, and aberrant movement habit on lower limb venous return are discussed.
Manual therapists and other professionals who work with older adults have a critical role in supporting this pump in the years prior to significant structural vein disease. They can support optimal return of blood, recognise when support is failing, and refer patients for specialist evaluation and management of chronic venous disease.
Written by info@linkpublishers.com