Manual therapy treatment:
Manual treatment cannot directly heal a pathologic disc. Instead, manual treatment should be directed at decreasing the stress factors that can aggravate or perpetuate a pathologic disc. Soft tissue manipulation should be done to relieve any unnecessary compression due to spasming of the nearby paraspinal musculature. As a rule, light to medium pressure is used, but even deep pressure can be employed. It is virtually impossible for pressure to directly impact upon the disc because of the presence of the transverse processes. However, if the pressure results in movement of the vertebrae, that could place an unhealthy force through the disc. Therefore, avoid deep broad compression strokes directly over the spine.
Heat can be used if it facilitates relaxation of the paraspinal (erector spinae and transversospinalis) musculature. However, if it is believed that swelling is a strong factor in the client’s condition, ice would be preferable. Having said this, the effect of heat or ice upon a lumbar disc is minimal because of the depth of the discs from the surface; heat or ice will have a more direct effect in the cervical region.
Stretching can be very beneficial, but there is controversy as to whether to stretch the client/patient into flexion or extension. Each sagittal plane direction of stretch (flexion / extension) has pros and cons. The positive effects of stretching the spine into flexion are that it stretches the posterior paraspinal extensor musculature and it increases the size of the intervertebral foramina (IVFs). Therefore, if a large part of the client’s symptoms is due to tightness of the paraspinals or compression of the spinal nerve within the IVF, flexion might be indicated. However, flexion compresses the anterior aspect of the disc; this pulls the posterior annular fibers taut and drives the nucleus pulposus posteriorly against the taut fibers, stressing and weakening them and possibly furthering the bulge or herniation. The positive effect of stretching the spine into extension is that it drives the nucleus anteriorly away from the injured posterior annulus; however it narrows the IVF. Same side lateral flexion in the lumbar and cervical regions and same side rotation in the cervical region also decrease the size of the IVF.
Pin and Stretch Lumbar Spine Joint Mobilization with Pelvis Movement
Active ROM Assessment for the Thoracolumbar Spine
Joint Mobilization of the Lumbar Spine into Flexion
If stretching into flexion is chosen for the lumbar region, an effective stretch for the low back is double knee to chest. Flexion can also be incorporated into the treatment if the therapist has a table that breaks/bends in the middle, allowing for flexion of the spine; this treatment technique is often referred to as flexion distraction. Regardless of which stretching approach is taken, what is most important is that referral symptoms are not increased. For more on this, see the Precautions/contraindications section at the end of this blog post article.
On the assumption that the pathologic disc is overly stressed because it is a hypermobile joint compensating for other, usually adjacent, hypomobile joints, joint mobilization (arthrofascial stretching) can be performed. It must be emphasized that this mobilization must be specific and precise, and directed at the hypomobile joints. However, it is highly risky to perform joint mobilization at the level of a bulging or herniated disc.
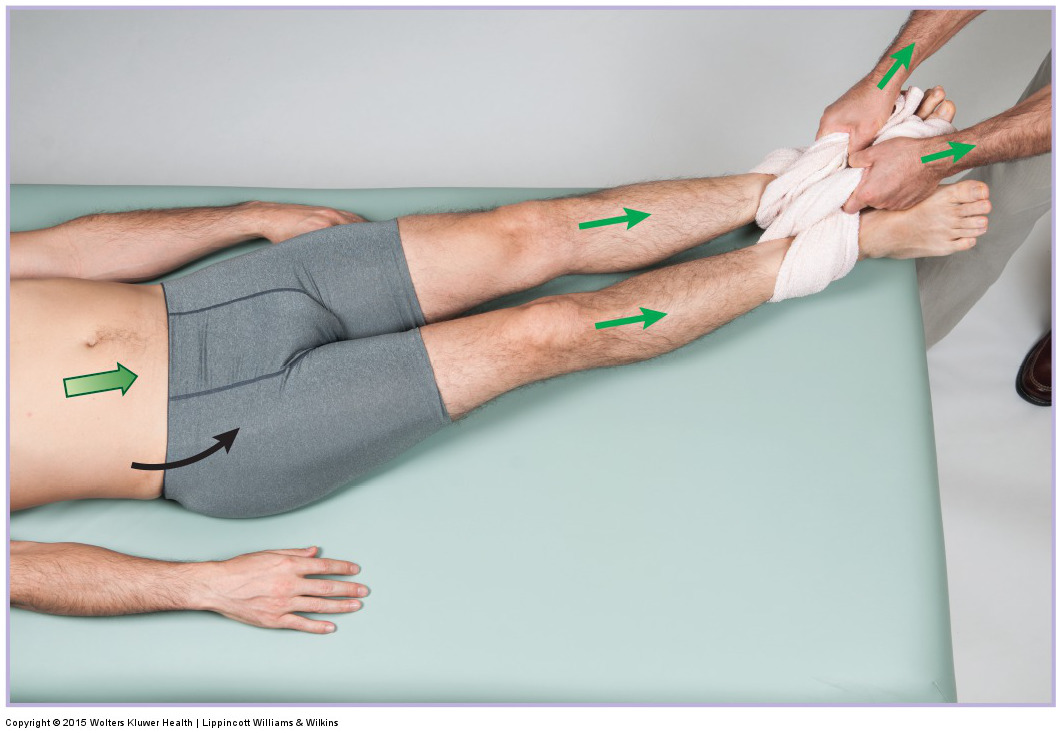
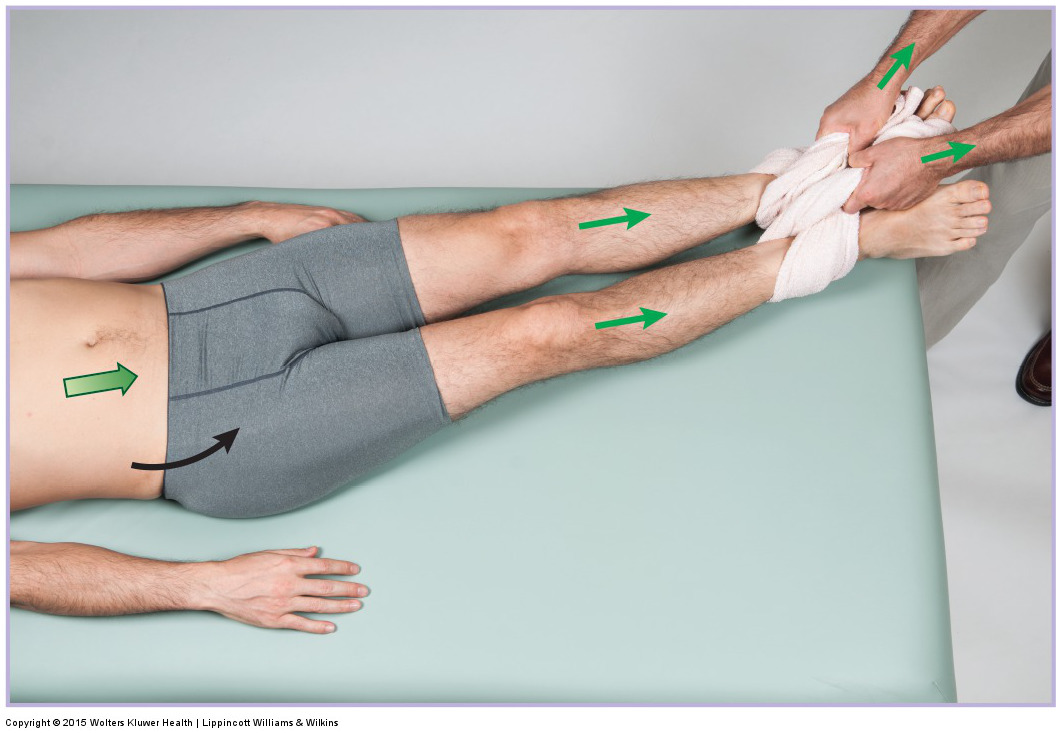
Traction for the lumbar spine with left lateral flexion added in. Permission: Joseph E. Muscolino. Manual Therapy for the Low Back and Pelvis – A Clinical Orthopedic Approach (2015).
Traction, also known as axial distraction can be beneficial for the client/patient with a pathologic disc because it opens up the IVFs of the spine, thereby relieving possible compression of the spinal nerves. It also decompresses the spine, thereby unloading the disc and possibly decreasing the size of the bulge/ herniation. Logistically, traction is more easily and effectively performed for the cervical region, and is facilitated by using a towel or king-sized pillow case.
It is important to perform cervical traction extremely gently so as to not overstress and possible tear fibers of the discs and facet joint capsules. It is also important to build up the time of cervical traction over a number of sessions. Gentle traction held for five seconds or less is recommended for the first session. Each successive session can gradually and slowly add to the force and time of traction, up to mild/moderate tension that is held approximately 20-30 seconds. Traction should never exceed the comfort of the client.[1]
Traction can also be done for the lumbar spine by using a towel of pillowcase to pull on the client’s/patient’s lower extremities. However, this is contraindicated if there is hypermobile instability at the knee joint.
Summary of Manual Therapy treatment Protocol for Pathologic Disc
| 1. Soft tissue manipulation to loosen nearby paraspinal musculature |
| 2. Heat to relax musculature (if swelling is not a concern) |
| 3. Ice if swelling is a concern |
| 4. Joint mobilization (arthrofascial stretching) to other hypomobile joints. |
| 5. Traction |
| 6. Stretching into flexion (generally during the acute stage) |
| 7. Self-care stretching into extension for the lumbar spine (generally in the post-acute stage). |
Precautions/contraindications:
The major precaution for clients/patients with a pathologic disc condition is to never do anything that increases neural compression and therefore referral into the extremity. This contraindication must be strictly observed!
Generally, for acute disc episodes, it might be safer to avoid positions of extension, especially in the cervical spine. Same side lateral flexion and same side rotation should generally also be avoided in the cervical region, and perhaps the lumbar region as well. Many clients/patients with lumbar disc pathologies do well with self-care extension exercises, but these exercises might be safer to begin and perform after the client/patient is out of the acute stage.
If joint mobilization of nearby hypomobile joints is performed, extreme care must be exercised to avoid mobilization of the pathologic disc. If cervical traction is carried out, be sure to perform this technique extremely gently at first, and build up its intensity slowly over many sessions. Beyond concern for the integrity of the annular and facet capsular fibers, cervical traction can lead to dizziness and nausea if performed too forcefully (due to irritation of the deep proprioceptors of the neck).
Note: If you suspect that a client/patient has a pathologic disc that is compressing neural contents and causing referral into an extremity, immediate referral to a physician is indicated. You may continue to provide adjunct care for the client, but involvement of a physician is important.
[1] Before employing traction, be sure that it is within the scope of your practice by checking with your local association or governing body.