Note: This is the thirteenth blog post article in a series of 14 articles on Assessment/Diagnosis of musculoskeletal conditions of the neck (cervical spine). See below for the other articles in this series.
Treatment Strategy
Once the health history and physical assessment examination have been performed, a treatment strategy can be developed. This involves creating a treatment plan for the client. Three principle components of a treatment plan must be determined:
- Treatment techniques that will be used during the sessions
- Frequency of sessions
- Home advice that will be given to the client
Treatment Techniques
The pathomechanics of the condition will determine the objectives of care, which in turn will determine the treatment techniques to be used. Most neck conditions involve tight/taut soft tissues (hypertonic musculature and fascial adhesions), so loosening these tissues is usually the primary focus of treatment. Most conditions that have been present for some time also involve joint dysfunction hypomobilities, so joint mobilization should be another focus. It is essential to address both of these aspects of the condition if the client’s musculoskeletal health is to improve.
The treatment techniques are designed to address tight/taut myofascial tissues, as well as joint dysfunction hypomobilities. These techniques tend to be most effective if performed after the client’s tissues have been warmed up. Choosing which technique to use is often a matter of both the therapist’s and the client’s personal preference. The fundamental treatment skillsets are soft tissue manipulation (massage), stretching, joint mobilization (Grade IV or V), and hydrotherapy. The most effective approach is usually to combine multiple techniques within the treatment plan. (Before employing any new technique in your practice, be sure that it is within the scope of practice of your profession.)
Frequency of Sessions
Once the techniques have been chosen, the next step is to decide the optimal frequency of care. Again, this depends on the circumstance. If a client is basically healthy and simply wants to maintain good health, the frequency might vary from once a week to once a month, depending on the client’s lifestyle and health. However, if a client has a musculoskeletal condition that needs to be remedied, physical rehabilitation requires a frequency of two to three times per week. This is common in physical therapy, chiropractic, Pilates, yoga, strength training, and sport training, and the same holds true for manual (and movement) therapy.
Note: For massage therapists, having a client come in for care once a week is usually considered to be the gold standard. However, a response to this might be: The client only comes in once per week? It must be emphasized that rehabilitative care requires a greater frequency. So if you are a manual/massage therapist and looking to do true clinical orthopedic manual therapy (what might be called medical massage), then the old mind-set of frequency of care of massage when it is thought of as a luxury for the body must be changed. Once a week means that there will be another 167 hours before the client returns. In this period of time, muscle memory (gamma motor system/muscle spindle) patterns for baseline tone will fall back to being hypertonic/locked/tight. And fascial adhesions will build up again due to the loss of mobility in the tissues. Asking the client to return twice (or even three times) per week is what is in the client’s best interest; please do not feel guilty about this. It will achieve the maximum response for the time, energy, and money spent. If you truly believe in the power of manual and movement therapy, frequency of care should be structured as it is in every other world of rehabilitative care. And part of your practice needs to be spent explaining this to your clients so that they understand this and they take clinical orthopedic manual therapy seriously as a true form of rehab therapy!
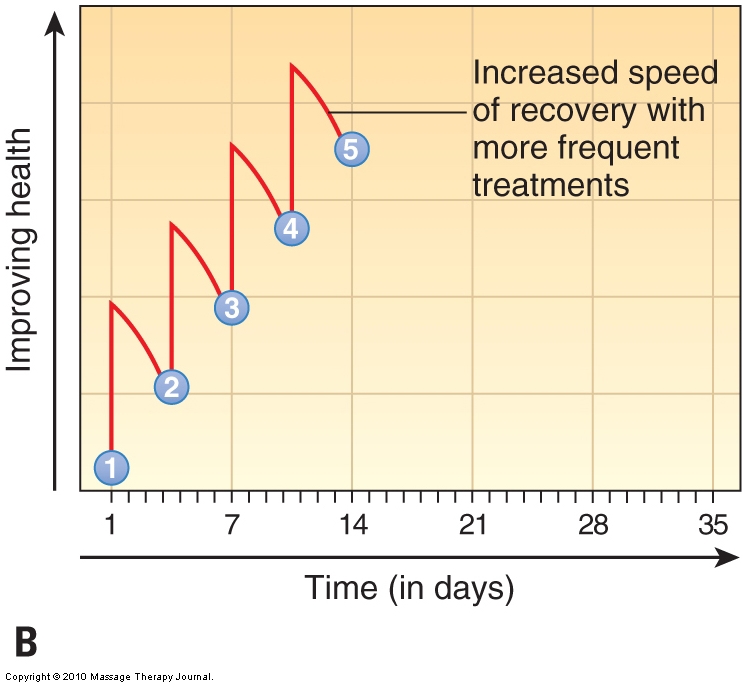
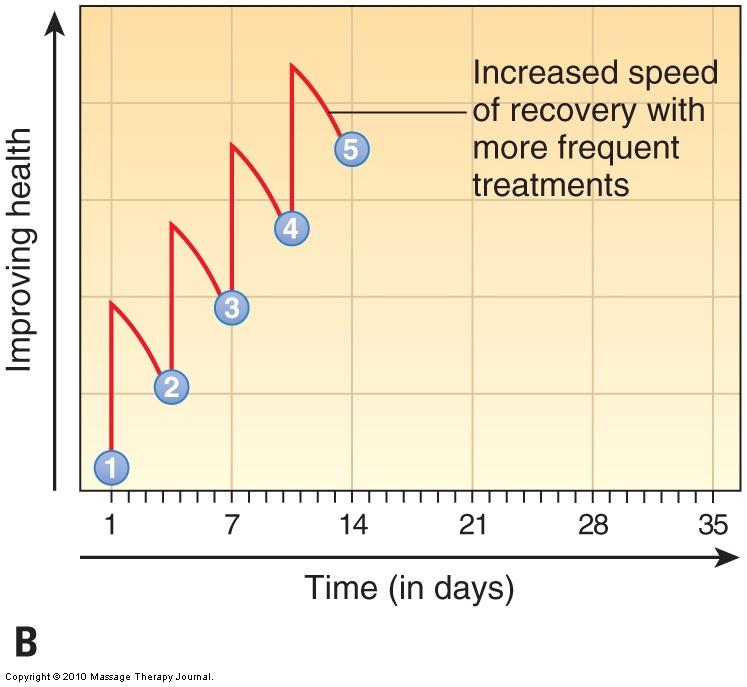
Each treatment session must build on the previous one if the client is to improve. Performing a treatment physically changes both the state of the tissues and the neural patterns for muscle contraction. As time passes after the session, these changes are gradually lost as the body reverts back to the pattern of its pathologic condition. If too much time elapses between visits, then the client continually regresses back to his or her dysfunctional pattern before the successive treatment occurs. Therefore, for care to be effective and efficient, treatments should be spaced no more than 2 to 3 days apart until the desired improvement has been achieved (Fig. 18). Although this may seem like a strong commitment to ask of a client, it is the most time- and cost-efficient approach.
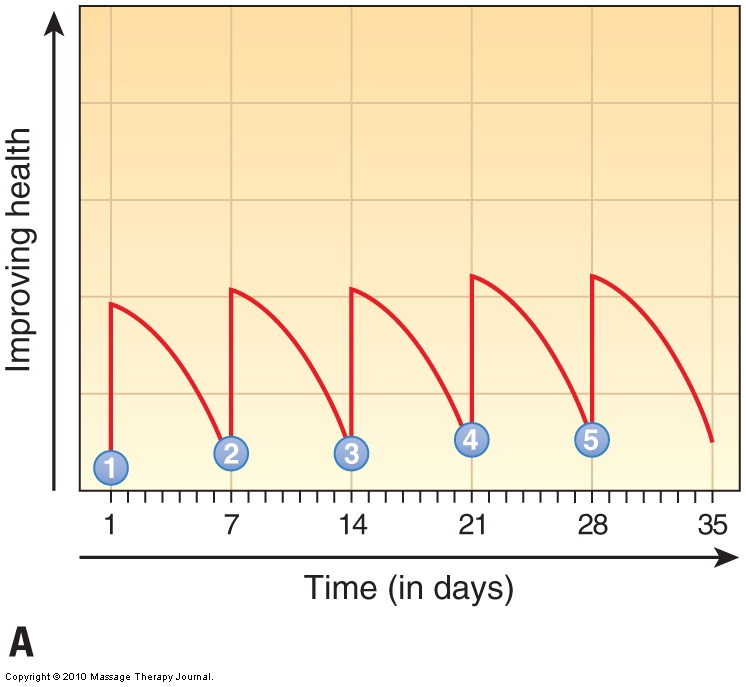

Figure 18. Effects of frequency of care. (A) Treatments frequency of once per week. (B) Treatments frequency of twice per week. Note the increased speed of recovery of the client’s condition when treatments are more frequent. Numbered treatments are indicated in blue circles. (Courtesy Joseph E. Muscolino. Originally published in the massage therapy journal (mtj): treatment planning and client education. Winter 2010.)
Home Self-Care Advice
Regarding home self-care advice, it is extremely valuable to offer the client suggestions about postures, hydrotherapy (hot and cold), stretching, and strengthening (if your scope of practice permits). It can also be very helpful to involve the client in his or her own treatment plan. After all, even if a client sees the therapist three times a week for an hour at each session, the client is still on his or her own for the other 165 hours of the week. If the client is engaging in unhealthy postures and activities at home and work, this can easily overwhelm the therapist’s ability to assist. If instead the client uses that time to further the objectives of the treatment plan, then recovery will proceed more quickly. For more on home advice, see Chapter 11.
Note: Giving Home Self-Care Advice
It is best to avoid over-recommending when giving home advice to clients. Whereas many clients will do one, two, or perhaps three recommended stretches, if the therapist gives them four, they will probably become overwhelmed and do nothing. Whether the threshold for being overwhelmed is 4 or 10, in general, the best rule regarding home advice is to give the client as much as he or she will do, and no more. The exact amount will vary according to the client’s level of self-discipline and enthusiasm. Having said this, clients who are athletes, dancers, Pilates, yoga people generally are very disciplined and welcome more self-care recommendations.
This blog post article is the thirteenth in a series of 14 blog post articles on Assessment/Diagnosis of musculoskeletal (neuro-myo-fascio-skeletal) conditions of the neck (cervical spine).
The articles in this series are:
- Introduction to Assessment/Diagnosis of the Neck
- Verbal and Written Health History
- Overview of Physical Examination Assessment
- Postural Assessment
- Neck General Orthopedic Assessment: Range of Motion and Manual Resistance
- Palpation Assessment
- Motion Palpation (Joint Play) Assessment
- Special Orthopedic Assessment Tests for the Neck – Space Occupying Conditions
- Special Orthopedic Assessment Tests – Space Occupying Conditions – Slump Test
- Orthopedic Assessment of Thoracic Outlet Syndrome – Adson’s, Eden’s, Wright’s
- Orthopedic Assessment of Thoracic Outlet Syndrome – Brachial Plexus Tension Test
- Special Orthopedic Assessment Tests – Vertebral Artery Competency Test
- Treatment Strategy and Treatment Techniques
- Assessment and Treatment of Specific Musculoskeletal Conditions