This blog post article is part of a series of articles on assessment of the low back and pelvis. Scroll to the end of this article to see the others in this series.
Postural Assessment
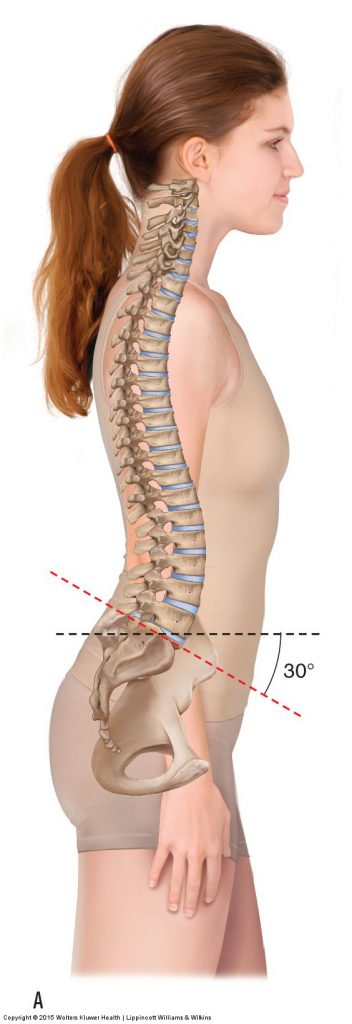
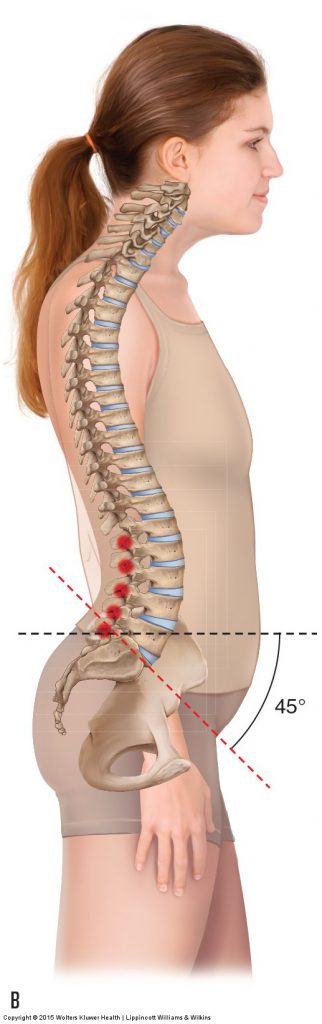
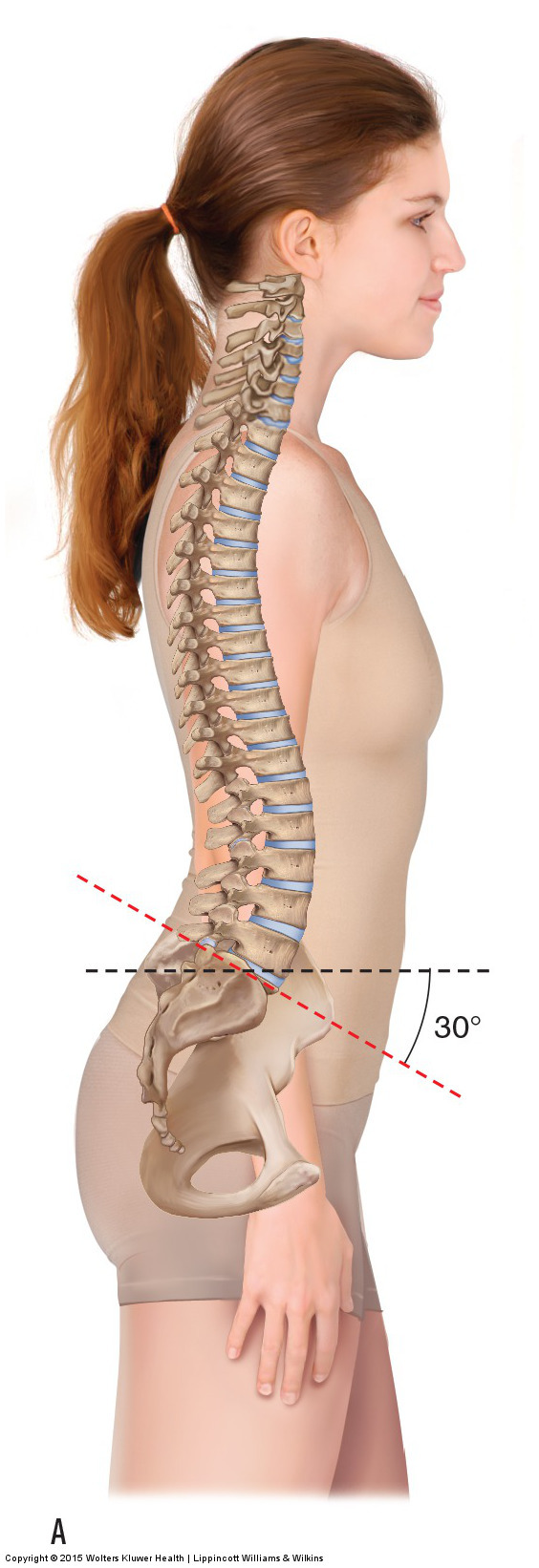
Figure 1. Good and bad low back posture. (A) The client’s posture is considered good because the sagittal plane tilt of the pelvis and the lumbar lordotic curve are within normal limits. (B) The posture could be called bad because the pelvis is excessively anteriorly tilted and the lumbar lordosis is increased. This places increased weight-bearing stress on the facet joints of the lumbar spine and creates shortening of some muscles and lengthening of others. Manual Therapy for the Low Back and Pelvis – A Clinical Orthopedic Approach (2015)
Postural assessment is usually the first physical assessment procedure that is performed. The term posture means position; therefore, in postural assessment, the client’s static position is evaluated. Before evaluating a client’s posture, it is important to understand what is meant by good posture and poor posture. Good posture is defined as a balanced posture that is symmetrical and does not place excessive stress on the tissues of the body (Fig. 1A). Bad posture, in contrast, is asymmetrical and/or imbalanced and places excessive physical stress on the tissues of the body (Fig. 1B). When evaluating a client’s posture, look for asymmetries and deviations, as these will indicate increased stress forces on the tissues of the body. When a client has a postural deviation, it is important to determine why it is occurring and what tissues are stressed as a result of the posture.
A client may assume an infinite number of postures during the day. Unfortunately, therapists usually perform only standing postural assessment, often using a plumb line. (A plumb line is a string that has a weight attached to it [“plumb” comes from the Latin word for lead] so that the string hangs perfectly vertical, allowing the therapist to check for symmetry relative to the vertical line.) Although standing posture may be important to evaluate, it is not the only posture that should be assessed. In fact, depending on the client’s profession, hobbies, and activities, it may not even be pertinent to the client’s condition. It is important to assess all postures that the client assumes. For clients with low back and pelvis problems, sitting posture is especially important, such as when sitting at a desk or driving a car. For this reason, it is important to inquire about what types of seated postures the client engages in and how many hours of the day the client spends in each. Given that most people spend 6 to 8 hours a day sleeping, it is also important to find out what position or posture the client usually sleeps in (this is usually done during the health history).
Examples…
A few examples will illustrate the critical reasoning skills involved in a client’s postural assessment in which a postural deviation is found.
- Example 1: A common postural deviation occurs when one iliac crest is higher than the other. This is often caused by increased tension of some of the muscles in the region, for example, hip joint abductors (e.g., gluteus medius) on the low iliac crest side and/or elevators of the pelvis (e.g., quadratus lumborum) on the high iliac crest side. The therapist would need to know to specifically evaluate for these tight muscles during the palpation and ROM assessments. If these muscles are tight, treatment might target these muscles and include home advice for the client regarding stretching and/or hydrotherapy. A high iliac crest may also result in a compensatory scoliosis; therefore, the therapist should know to assess for this condition. Other recommendations to help alleviate unlevel iliac crest height might include avoiding certain postures or modifying postures, and activities that cause or perpetuate this condition.
- Example 2: If the client’s posture shows that the pelvis is excessively anteriorly tilted, it would be reasonable to suspect that the hip flexor muscles and/or low back extensor muscles are tight because these are muscles that pull the pelvis into anterior tilt. The therapist would then focus on assessing these muscles; if they are revealed to be tight, the therapist would direct treatment and home advice toward their care.
Given the focus and scope of this set of blog post articles, only postural deviations of the low back and pelvis have been mentioned. However, postural deviations often involve the entire body, with a problem in one area causing secondary consequences and compensations in other regions. For example, a dropped arch in the foot may lead to an iliac crest height that is low on one side with a compensatory scoliosis that may reach to the cervical spine. For this reason, postural assessment should always address the client’s entire body from the feet to the head. After the therapist has taken a look at a full body assessment of the client’s posture, then appropriate treatment can be performed.
(Click here for a blog post article on postural assessment of the neck.)
This blog post article is the 4th in a series of 18 blog posts on the subject of assessment of the low back and pelvis.
The blog post articles in this series are:
- Introduction to Assessment of the Low Back and Pelvis
- Health History
- Introduction to Physical Assessment Examination of the Low Back and Pelvis
- Postural Assessment of the Low Back and Pelvis
- Range of Motion and Manual Resistance Assessment of the Low Back and Pelvis
- Muscle and Bone Palpation of the Low Back and Pelvis
- Joint Motion Palpation Assessment
- Overview of Special Orthopedic Assessment Tests of the Low Back and Pelvis
- Straight Leg Raise Tests for Space-Occupying Lesions
- Cough Test and Valsalva Maneuver
- Slump Test
- Piriformis Stretch Test
- Straight Leg Raise and Manual Resistance Tests for Strains and Sprains
- Nachlas and Yeoman’s Tests
- Sacroiliac Joint Medley of Tests
- Treatment Strategy for the Low Back and Pelvis
- Self-Care Advice for the Client with a Low Back / Sacro-Iliac Joint Condition
- Brief Review of Assessment and Treatment of Conditions of the Low Back and Pelvis