Assessment/Diagnosis of Sacroiliac Joint Dysfunction
Assessment/diagnosis of sacroiliac joint dysfunction (SIJ dysfunction) is done by motion palpation, in which the joint is challenged to move while the motion of the joint is assessed. This can be done two ways. One method is to directly challenge the joint by pressing on the sacrum or ilium. The other way is to indirectly challenge SIJ motion by having the client/patient move their thigh, which requires movement of the pelvic bone (via femoropelvic motion) and therefore movement at the SIJ.

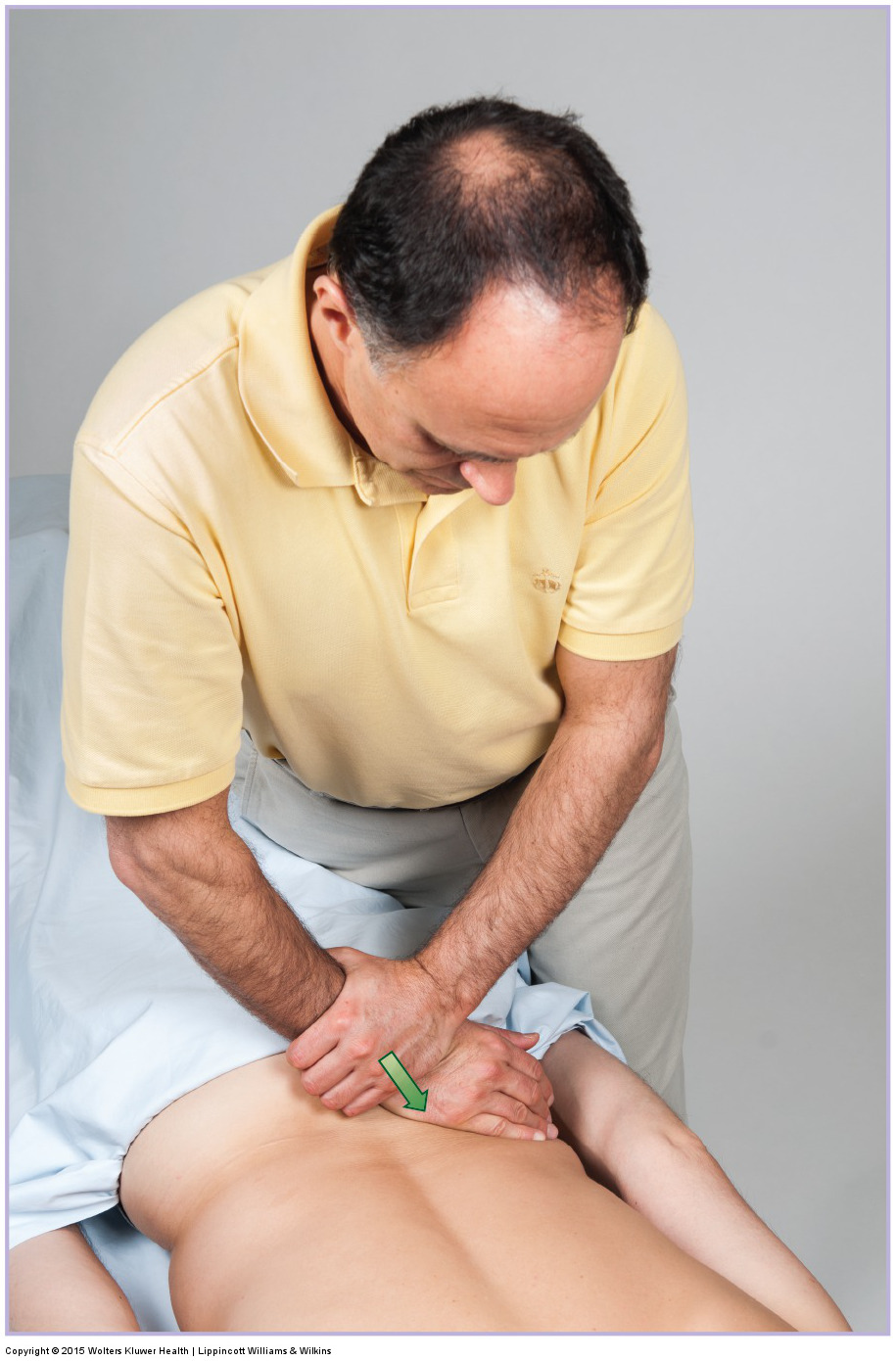
Motion palpation assessment (and joint mobilization treatment) for the left sacroiliac joint. Permission: Joseph E. Muscolino. Manual Therapy for the Low Back and Pelvis – A Clinical Orthopedic Approach (2015).
To directly palpate the SIJ, have the client/patient prone and place the client’s/patient’s posterior superior iliac spine (PSIS) in the intereminential groove (between the thenar and hypothenar eminences of your hand). Now gently press downward on the PSIS with body weight and feel for the resultant motion of the PSIS, and therefore the SIJ on that side. Pressure can be placed directly downward (anteriorly) toward the table, or anteriorly and superiorly toward anterior tilt of the pelvic bone, or anteriorly and laterally to gap the SIJ, or anteriorly, superiorly, and laterally along the plane of the joint. Similarly, SIJ motion can be assessed by using the ulnar side of the hand (“knife edge”) to press directly on the sacrum. If pressure is placed toward the (superior) base of the sacrum, nutation (anterior tilt) of the sacrum is challenged and assessed. If instead pressure is place toward the (inferior) apex of the sacrum, counternutation (posterior tilt) of the sacrum is assessed.
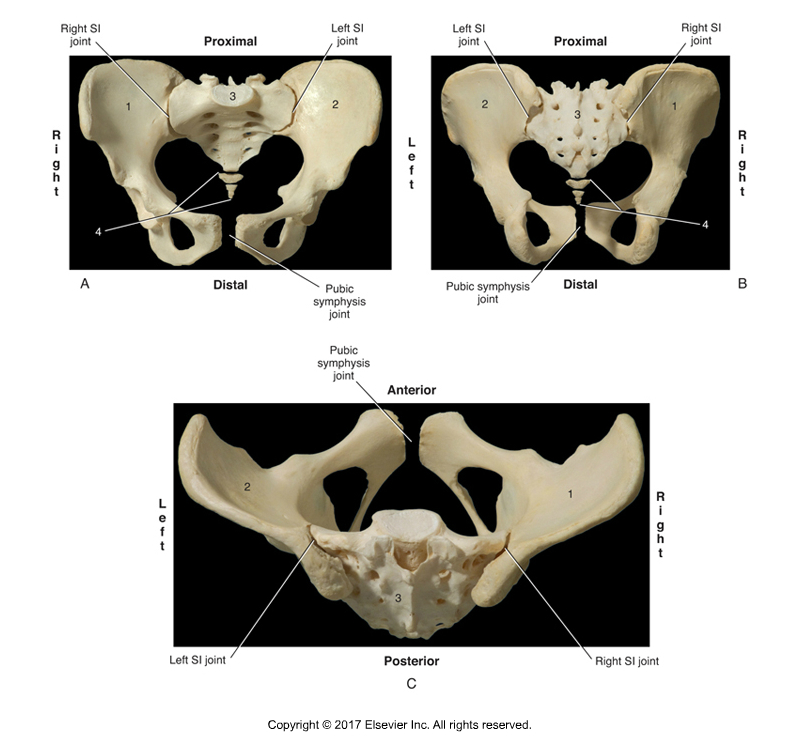
Sacroiliac Joint. Permission Joseph E. Muscolino. Kinesiology – The Skeletal System and Muscle Function 3ed (Elsevier) 2017.
Indirect motion palpation assessment of the SIJ can be done with the client/patient standing. This orthopedic assessment test is often referred to as the Stork Test. Have the client/patient standing facing a wall, far enough away to have room to flex the thigh to ninety degrees with the knee joint flexed to ninety degrees, but close enough to be able to place finger tips on the wall for a little bit of balance. Place palpating thumb pads on the client’s/patient’s PSISs (best is to contact the inferior aspect of each PSIS). Now ask the client/patient to alternately flex each thigh to ninety degrees and feel for the relative motion of the PSISs. The PSIS on the side of thigh flexion should be felt to drop inferiorly. This palpation assesses combined motion of both SIJs. To assess motion of one SIJ at a time, instead palpate one PSIS as explained above, but place your other thumb pad on a sacral tubercle and ask the client/patient to flex the thigh on the side the PSIS is being palpated; again, the PSIS being palpated should be felt to drop relative to the sacral tubercle palpation contact. Then repeat this for the other side. These motions can be very subtle so have the client/patient move slowly and repeat the palpation procedure a few times. It is also important to make sure that the client/patient flexes the thigh all the way to 90 degrees, but no farther.
The static position of the bones of the SIJ can also be statically palpated. This is usually best assessed by feeling for the position of the sacrum. Although static positioning does not necessarily imply movement dysfunction, there often is a parallel because static palpation often reveals soft tissue tension forces on the joint that hold the bones of the joint in a position that is not symmetrical (i.e., not anatomic position), which might also affect motion patterns. Feel for whether the sacrum is asymmetrically tilted anteriorly toward the right or left side. Feel also for the general degree of positional anterior tilt (nutation) of the sacrum. Static palpation can be a helpful addition to motion palpation but should not replace it.
Differential Assessment of Sacroiliac Joint Dysfunction
Assessment of sacroiliac joint dysfunction is straightforward; if motion palpation reveals that the joint’s motion is restricted or excessive, the assessment of joint dysfunction can be made. What is just as or more important is to find the cause of the dysfunction. Look to determine whether it is a compensation for the contralateral SIJ, and/or is related to a SIJ sprain or strain, or muscle spasm. Look also for habitual postures and movement patterns that the client/patient is assuming that might be contributing to the problem.