Manual therapy treatment for overpronation:
Because overpronation, whether it is a supple or rigid flat foot, does not directly cause pain, and even its effects farther up the body will likely not cause pain for many years or decades, it is likely that the client’s/patient’s condition will be chronic by the time that it is addressed. For this reason, it will likely be stubborn and resistant to treatment. Therefore, manual therapy care will have to be consistent.
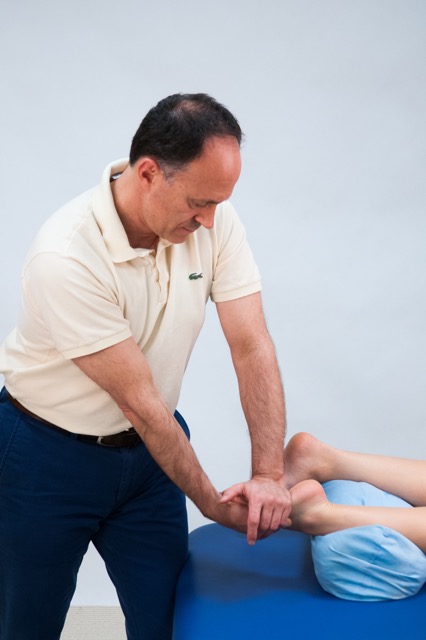
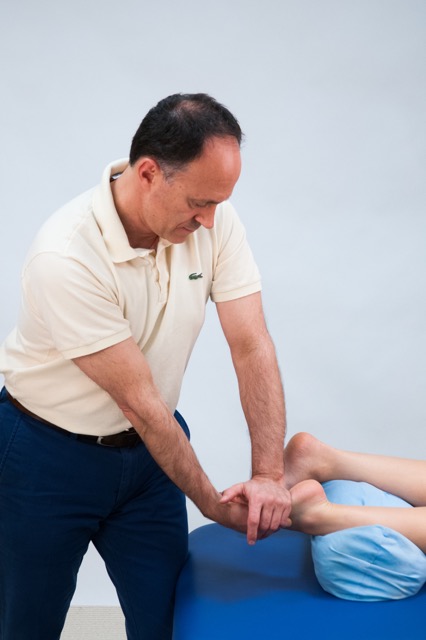
Joint mobilization (arthrofascial stretching) of the foot from plantar to dorsal. Permission: Joseph E. Muscolino.
For a supple flat foot, manual therapy’s role is indirect. By employing both soft tissue manipulation and stretching (specifically to the plantar fascia and plantar intrinsic musculature of the foot), the goal is to loosen tight musculature and eliminate TrPs. This can both relax the baseline tone of muscles that are pulling toward pronation as well as strengthen muscles that support the arch by increasing the efficiency of their contraction. Manual therapy should also be directed toward any sequelae of overpronation, such as tight lateral rotation hip joint musculature or tight paraspinal (erector spinae and transversospinalis) musculature as a result of scoliosis, if present.
For the rigid flat foot, or even the supple flat foot that is becoming more rigid, manual therapy’s role is more direct. It is performed to loosen fascial adhesions that are locking the bones in a position of pronation. In these cases, deeper soft tissue manipulation into the plantar side of the foot, stretching of the tight muscles, and joint mobilization (arthrofascial stretching) of all the joints of the foot (especially the tarsals) is called for. Most often, because the navicular and cuboid bones have “dropped”, they need to be mobilized from plantar to dorsal. And because stretching and joint mobilization are always more effective if the soft tissues are first warmed up, moist heat is also valuable as a modality. Depth of pressure should always begin as light to moderate, but will usually have to transition to deeper pressure to access long-standing fascial adhesions and deeper tighter musculature that is likely with a rigid flat foot or even a chronic supple flat foot.
As important as manual therapy can be for overpronation, it can never fully and permanently resolve the condition. The objective of these therapies is to loosen the tight musculature and other taut soft tissues. However, this only addresses one part of the problem, and usually the lesser part. The other aspect of this condition is the weakness of the musculature that must support the arch structure against the forces that cause overpronation. These muscles must be strengthened. Therefore, referral to a fitness trainer, physical therapist, yoga or Pilates instructor, or the recommendation of specific exercises to strengthen the muscles that support the arch is imperative (for more on the strengthening of these muscles, see Self-care for the client/patient in another blog on this condition).
Summary of Manual Therapy Treatment Protocol for Overpronation
| 1. Soft tissue manipulation to the plantar foot |
| 2. Moist heat and stretching of the plantar fascia and intrinsic musculature |
| 3. Soft tissue manipulation and stretching of the rest of the lower extremity and spine as needed |
| 4. Joint mobilization of the foot, especially the tarsals, most often the navicular and cuboid |
| 5. Strengthen the musculature of the arch structure of the foot |
Precautions/contraindications:
There are a few precautions when working on a client/patient with overpronation. Care must be exercised if working near the fibular head because of the presence of the common fibular nerve, and if working the medial ankle region because of the presence of the tibial nerve and artery. If work is being done in the gluteal region for the deep lateral rotators of the hip, be aware of the location of the sciatic nerve near the piriformis and lying over the quadratus femoris.
One precaution and possible contraindication is to be careful when attempting to make any structural change to an elderly person’s foot. Their tissues are less elastic than a younger person’s, and if they have been overpronating for decades, it is likely that all the tissues throughout their body have adapted to this structure. Changing something as fundamental as the foundational posture of the foot might cause unwelcome compensatory adaptations above. Beyond these precautions, for all clients, be sure to gradually transition to deeper pressure because many people are tender in the plantar region of the foot.