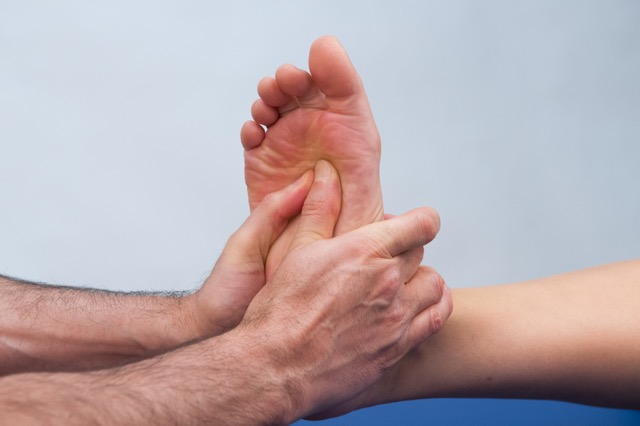
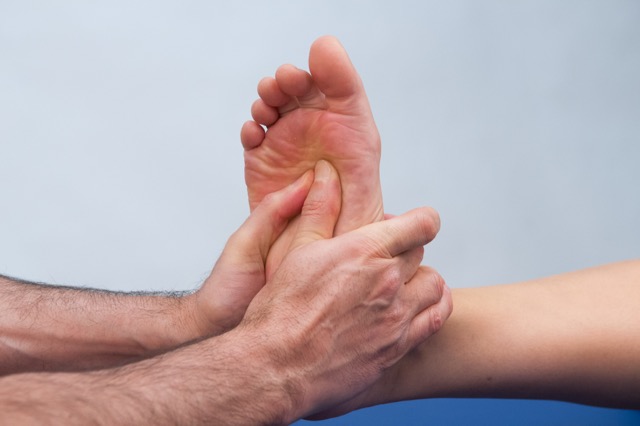
Manual therapy treatment for plantar fasciitis:
Manual therapy treatment for plantar fasciitis is geared primarily toward reducing the inflammation of the condition, loosening any tautness/tightness of the plantar fascia and associated intrinsic musculature, and correcting the underlying cause.
For the condition itself, ice is indicated to reduce the swelling. Gentle effleurage strokes from distal to proximal might also be helpful. Also, the client/patient should be advised to decrease weight-bearing activities and wear shoes with comfortable arch supports.
Soft tissue manipulation should also be performed for any tautness of the plantar fascia as well as any muscular hypertonicity (global tightness / myofascial trigger point) or myofascial adhesions that are found. To prevent the soft tissue manipulation from increasing swelling, it is probably best to use mild or moderate pressure. Be especially careful and gentle near the calcaneal attachment. If deeper pressure is used, then it might be desirable to ice afterward to prevent an increase in swelling. Treating tight musculature and myofascial adhesions is also facilitated by applying moist heat before soft tissue manipulation is performed. However, if there is a lot the swelling, it might be best to avoid the use of heat. If it is deemed important to warm up the musculature and myofascial tissues with moist heat before working the soft tissue, then as with deeper pressure it might be wise to apply ice after soft tissue manipulation.
If tightness is a pressing concern, then stretching should also be performed. Because the stretching/tensile force from overpronation is usually the cause or an aggravating factor of this condition, any stretching done should be gentle and performed with caution. When stretching, the therapist should always be assessing for the response of the client’s/patient’s tissues to the stretch.
Note: Whenever there are competing effects of treatment, for example deeper pressure and heat help alleviate soft tissue tightness and adhesions but might increase swelling, a clinical decision must be made based on the priorities of the condition of the client/patient lying on the table. If the swelling is the more pressing concern, then these treatment techniques should be avoided. However, if the soft tissue tightness and adhesions are of greater concern, then heat and deep pressure might be indicated. The fear of increased swelling can be avoided if icing is done afterward.
Once the plantar fascia and other myofascial tissues of the foot have been treated, it is important to address other myofascial tissues along the superficial posterior myofascial meridian (anatomy train). These include the gastrocnemius, hamstrings, sacrotuberous ligament, and erector spinae musculature. Then address the intrinsic tissues of the ankle and foot joints with joint mobilization (arthrofascial stretching). Begin mobilization at the ankle and subtalar joints, and then mobilize the bones/joints of the foot.
The chronic stage of any pathologic condition of fibrous fascia might transition from inflammation to degeneration. If this is the case, then the type of treatment administered should also transition. Instead of lighter work and icing, much deeper soft tissue manipulation can be done, especially near the attachment site on the calcaneus. It is usually recommended to perform cross-fiber strokes. The intention of this treatment is to increase circulation to the area so that fibroblasts are brought to the area to mend the degenerated collagen structure of the fascia.
Finally, because the underlying cause so often involves overpronation of the foot, this condition must be assessed, and if present, addressed.
Summary of Manual Therapy Treatment Protocol for Plantar Fasciitis
| 1. Acute stage: Ice and gentle distal-to-proximal effleurage |
| 2. Chronic stage: Moist heat, soft tissue manipulation (usually mild to moderate pressure), and stretch to the plantar foot (perhaps followed by icing) |
| 3. Work the superficial posterior myofascial meridian in the leg, thigh, pelvis, and back |
| 4. If the condition has transitioned to collagen degeneration, much deeper cross-fiber work is indicated |
| 5. Joint mobilization (arthrofascial stretching) of the ankle and foot |
| 6. Address overpronation of the foot if present |
Precautions/contraindications when treating plantar fasciitis:
During the acute stage of plantar fasciitis, nothing should be done that would increase swelling; therefore, any soft tissue manipulation or stretching should be gentle in force. Care should be taken when working near the calcaneal attachment.