Introduction to sciatica
Sciatica is a condition in which the sciatic nerve is compressed, causing referral symptoms (often pain or numbness) into the lower extremity. The referral symptoms can be sensory and/or motor depending on whether sensory or motor neurons are compressed.
The sciatic nerve is formed when the L4, L5, S1, S2, and S3 nerve roots merge in the abdominopelvic cavity. The sciatic nerve exits through the greater sciatic foramen into the posterior pelvis / gluteal region between the piriformis and superior gemellus muscles. There is a fairly common variation (found in approximately 15% of people) in which part or all of the sciatic nerve exits/pierces through the piriformis muscle itself. The sciatic nerve then travels down the posterior thigh, innervating the musculature of the posterior thigh (hamstrings and posterior head of adductor magnus) along the way. Just proximal to the knee, the sciatic nerve splits into the tibial nerve (L4, L5, S1, S2, and S3) and the common fibular nerve (L4, L5, S1, and S2) (Note: The common fibular nerve used to be called the common peroneal nerve.)
The tibial nerve continues down the posterior leg and innervates all the muscles in the superficial and deep posterior compartments of the leg. It then enters the foot posterior to the medial malleolus of the tibia and divides to become the medial and lateral plantar nerves, innervating the plantar intrinsic musculature of the foot.
The common fibular nerve splits to form the superficial and deep fibular nerves (old names: superficial and deep peroneal nerves). The superficial fibular nerve innervates the muscles of the lateral compartment of the leg (fibularis longus and brevis). The deep fibular nerve innervates the muscles of the anterior compartment of the leg (tibialis anterior, extensor hallucis longus, extensor digitorum longus, and fibularis tertius). It then travels into the foot, crossing the ankle joint anteriorly, and innervates the dorsal intrinsic musculature of the foot (extensor hallucis brevis and extensor digitorum brevis).
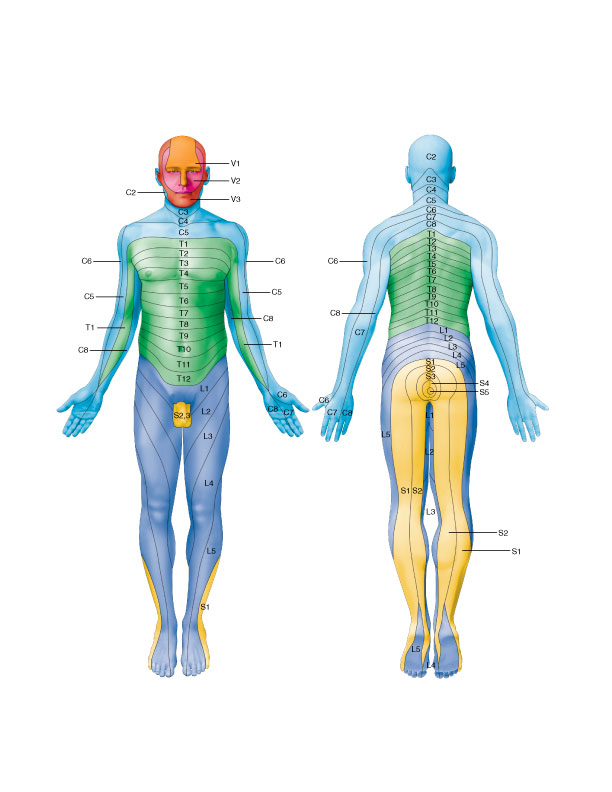
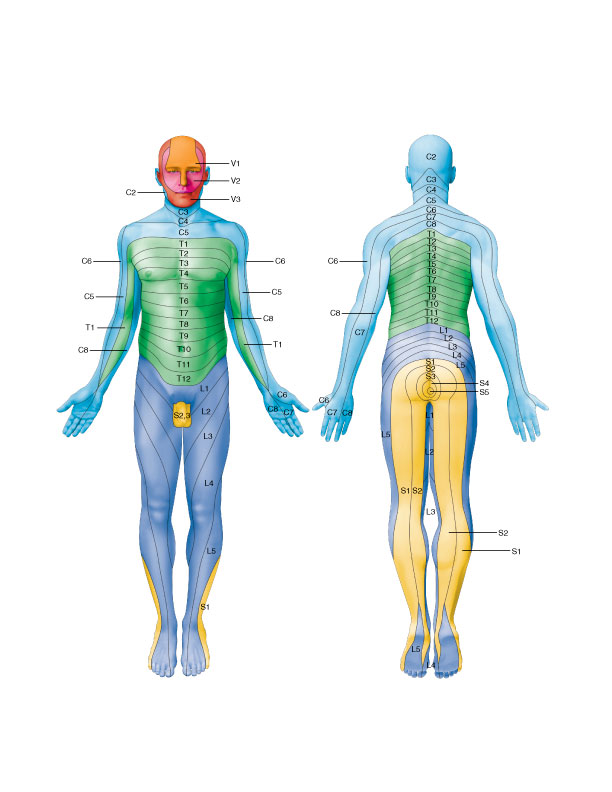
The sciatic nerve provides both motor and sensory innervation. The sciatic nerve and its branches innervate the musculature of the posterior thigh and all musculature distal to the knee joint. Its sensory innervation distribution is to the lateral leg (posterior and anterior sides) and the entire foot. A dermatomal map can be used to map out where the sensory innervation is for each of the spinal nerve roots of the sciatic nerve.
Causes
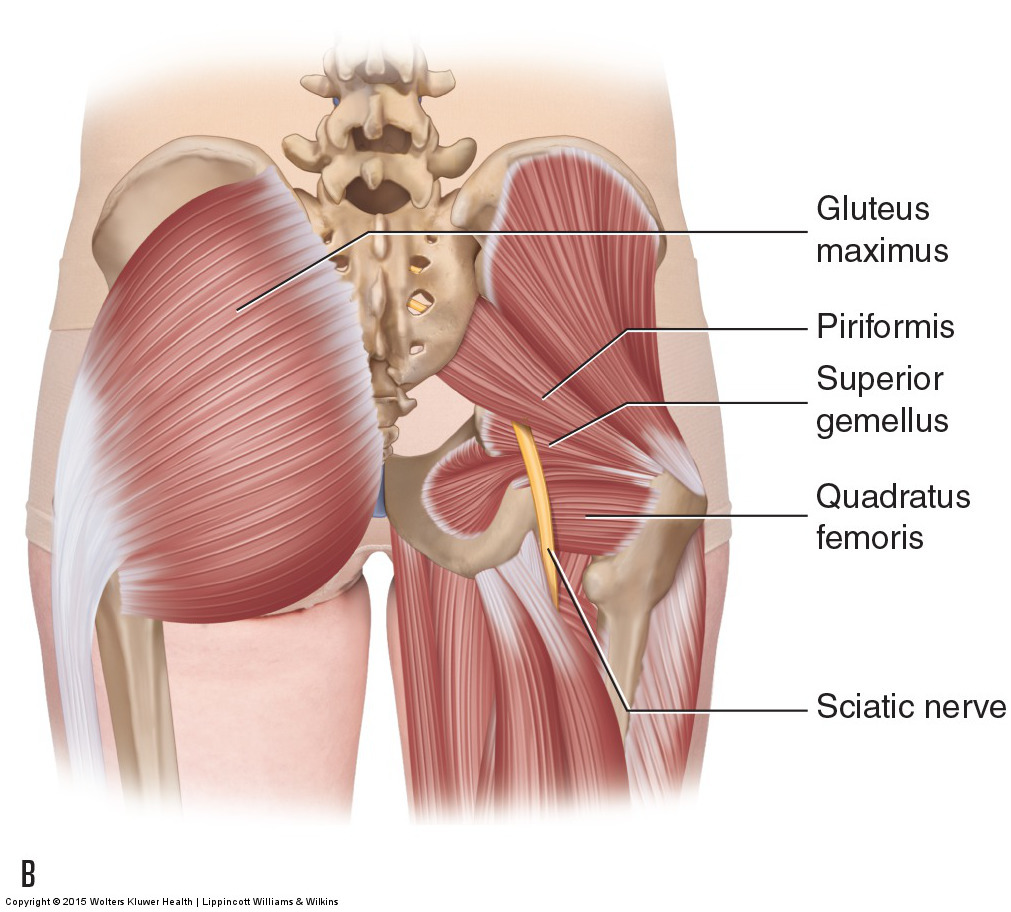
The Sciatic Nerve. Permission Joseph E. Muscolino. Manual therapy for the Low Back and Pelvis – A Clinical Orthopedic Approach (2015)
Given that sciatica is caused by compression of the sciatic nerve, anything that can compress the sciatic nerve can theoretically cause sciatica. The two most common causes of sciatica occur at the spine and are a pathologic disc (bulging or herniated) or an osteoarthritic bone spur. These space-occupying (nerve impingement) lesions can compress a nerve root of the sciatic nerve as it passes through the intervertebral foramen (IVF). The term lateral stenosis is used to describe stenosis within the IVF. A pathologic disc can also cause direct compression against the spinal cord in the central canal. Stenosis within the central canal is termed central canal stenosis. The exact symptoms that the client/patient experiences will depend upon which neurons of the spinal cord or nerve roots are compressed.
Another fairly common cause of sciatica is piriformis syndrome in which a tight piriformis compresses against the sciatic nerve. This compression can occur regardless of the sciatic nerve’s presentation in the gluteal region. Therefore, anything that tends to increase the baseline tone of the piriformis can contribute toward piriformis syndrome as the cause of sciatica. The baseline tone of the piriformis will increase with all postures and movement patterns that place an excessive demand upon lateral (external) rotation of the thigh at the hip joint.
A number of other factors can contribute to sciatica. Swelling often accompanies a pathologic disc and can further the sciatic compression within the IVF or central canal. Ligament hypertrophy within the central canal is another fairly common cause of sciatica; this usually occurs in elderly people. Although not very common, a cyst or tumor could potentially cause compress the sciatic nerve and cause sciatica with its characteristic referral symptoms. Even trauma to the sciatic nerve in the gluteal region or lower extremity can cause sciatica.