Self-care for the client/patient with ankle sprain:
Self-care for the acute ankle inversion sprain is RICE: rest, ice, compression, and elevation. The client/patient should be recommended to ice the ankle as long as swelling is present, whether that is three days, three weeks, three months, or longer. Instruct the client/patient to keep the ice on the ankle/foot until the area is numb and then remove it; this should be repeated as often as possible.
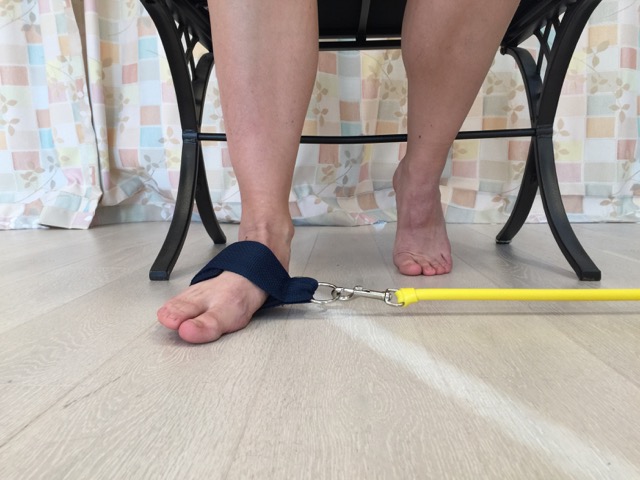
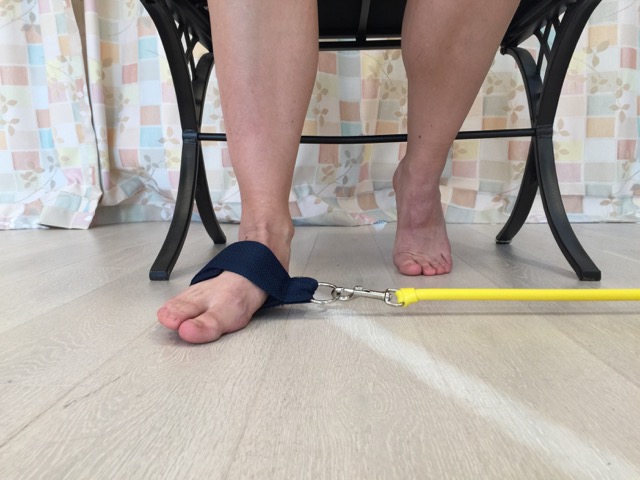
Thera tubing (Thera-ciser™ by Foot Levelers) resistance exercise for the evertors of the foot. Permission: Joseph E. Muscolino.
Self-care for the chronic ankle sprain involves strengthening the associated musculature, both generally because the client/patient is deconditioned/weaker from not having been active for some time, and specifically to strengthen eversion musculature to compensate for the lost integrity of overstretched lateral ligaments. An easy and inexpensive way to strengthen the evertor musculature is to use elastic thera tubing or thera bands. The client/patient should be made aware that no matter how much the eversion musculature is strengthened, strong musculature can only compensate for lax ligaments when the muscles are directed to contract. Therefore, during an unguarded moment, such as unexpectedly stepping on uneven ground that turns the foot into inversion, the musculature might not be able to contract quickly enough to protect the client/patient from another inversion sprain. For this reason, the client/patient who has experienced a moderate/marked inversion sprain must be careful into the future. Any manual or movement therapy that is directed toward increasing the client’s/patient’s proprioception would be valuable toward improving the reaction time of evertor musculature to protect the ankle joint into the future.
Medical approach to ankle sprain:
The medical approach to treatment of an ankle sprain (inversion sprain) depends on the severity of the injury. For a mild to moderate sprain, it is RICE (rest, ice, compression, elevation), and possibly the use of a brace/boot. Anti-inflammatory medication might be prescribed, or an injection of cortisone to decrease swelling is possible. Injection of platelet rich plasma (PRP) can also be done to help stimulate collagen growth for fascial ligament tissue regeneration. If the sprain is severe and/or if the ligament is ruptured, surgery can be done to sew the ligament back to its attachment.
Manual therapy case study for a client with ankle sprain:
Joe is an 18-year-old who runs cross-country for his high school team. During a race two weeks ago, he stepped on a tree root and sprained his right ankle joint into inversion. Because he was moving forward as the sprain occurred, the sprain was also into plantarflexion. The degree of the sprain was moderate and he was not able to complete the race. He experienced immediate pain, which was worst when weight bearing; his ankle began to swell within a few hours. Joe went to his chiropractic physician who ordered X-Rays, which were negative for fracture. Joe’s father is a regular client/patient of a clinical orthopedic massage therapist, so he brought Joe to the therapist to see if manual therapy would be of any help.
Upon visual examination, the therapist noted moderate swelling immediately distal to, and also distal and anterior to, the lateral malleolus; no ecchymosis was observed. Palpatory examination revealed exquisite tenderness over the anterior talofibular ligament, as well as mild/moderate tenderness over the calcaneofibular ligament. No pain was experienced with palpation of the posterior talofibular ligament. Palpation also revealed tightness and myofascial trigger points in the fibularis longus and brevis muscles, as well as in the gluteus medius and quadratus lumborum on the opposite (left) side. All passive ranges of motion of his right ankle joint were restricted, likely due to the swelling; Joe felt immediate pain with inversion.
Joe experienced a grade 2 inversion ankle sprain of the right ankle joint. The therapist recommended one to two half hour massages per week for four weeks. With the client/patient supine, the therapist performed approximately 5-10 minutes of gentle effleurage strokes to Joe’s right foot, ankle, and leg, distal to proximal in direction. While this was being done, moist heat was applied to his left gluteus medius. A flexible ice pack was then placed on the lateral side of Joe’s right ankle for 5-10 minutes while the therapist worked into the bellies of Joe’s fibularis longus and brevis musculature with moderate pressure. The therapist then spent the remainder of the time with Joe side-lying on the right side, working into the left sided gluteus medius and quadratus lumborum. The therapist reinforced what Joe’s chiropractic physician had recommended regarding self care with RICE.
At the end of four weeks, Joe’s pain was gone and the swelling was only mild in degree. With approval from the chiropractor, the therapist began to introduce gentle joint mobilization to the tarsal bones and fibula. Joe’s self-care program was also expanded to begin elastic tubing resistance exercise for the evertors, with icing to be done after each exercise session. The therapist continued to see Joe once per week for another four weeks, whereupon Joe was released from active care.