Self-care for the client/patient:
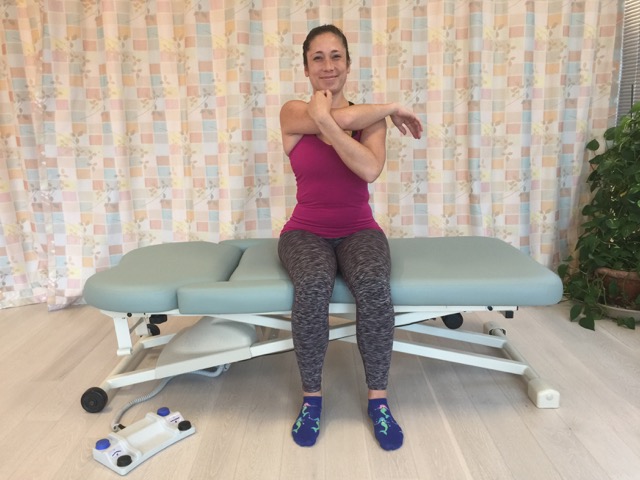
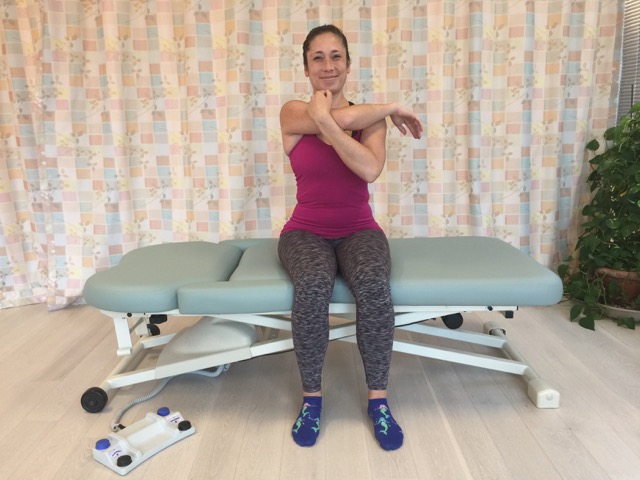
Self-care horizontal flexion shoulder stretch for the teres minor and infraspinatus muscles. Permission: Joseph E. Muscolino.
Self-care for the client/patient with rotator cuff pathology depends on the specific musculature that is affected and the specific pathology that is present. For tendinitis, icing should be recommended. For any type of rotator cuff pathology, the client should avoid any offending postures and activities. Proper postures at the computer are particularly important. The keyboard and mouse should be close to the edge of the desk so the client does not have to isometrically contract shoulder musculature to reach them. When sleeping, it is best to sleep on the other side and rest the injured arm on a large pillow in front of the patient’s/client’s trunk. For any tight musculature, it is valuable to stretch the hypertonic muscle. Stretching is performed by doing the joint action that is antagonistic to the joint action of the target muscle. For example, the teres minor and infraspinatus muscles are a lateral (external) rotators, so they would be stretched with medial (internal) rotation. Because the teres minor and infraspinatus muscles are horizontal extensors, they can also be stretched with horizontal flexion.
Patients/clients may also choose to take over-the-counter anti-inflammatory medication. If and when signs and symptoms of the condition have resolved, strengthening the shoulder and upper trunk musculature should be recommended.
Medical approach:
Medical management of rotator cuff tendinitis usually involves prescription non-steroidal or steroidal anti-inflammatory medication such as cortisone, as well as cortisone injections. If the degenerative phase is present, prolotherapy injections, including platelet rich plasma (PRP) injections are beneficial. If a mild tear is present, prolotherapy injections may also be beneficial. For a larger tear, surgery is an option depending on the degree of the tear and its functional impact on the patient’s/client’s life.
Manual therapy case study:
Bill is a 55-year-old right-handed executive who plays hockey recreationally once per week. Recently, while playing, he collided with another player and hit his right shoulder. He felt immediate pain in his right shoulder but kept playing. By the end of the game, his shoulder was very painful and it hurt to raise it to the side. His pain gradually lessened as the week went by, but playing hockey again the following week reaggravated it so he went to a clinical orthopedic manual therapist for care.
The therapist performed active and passive range of motion of the shoulder joint. Active range of motion into abduction and manual resistance to abduction reproduced his pain. Active range of motion into abduction with flexion (scaption) and manual resistance to abduction with flexion (scaption) also reproduced his pain. An oblique passive range of motion into adduction and extension also caused a mild increase of pain. All other active and passive ranges of motion were negative. Palpatory pain was also found at the distal tendon of the supraspinatus, immediately distal to the acromion process. Myofascial trigger points were also found in the belly of the supraspinatus and the middle deltoid. No joint crepitus was evident with any of the ranges of motion.
Given the diagnosis/assessment of tendinitis of the supraspinatus portion of the rotator cuff, the therapist recommended two one-hour massages per week for three weeks. Each session began with approximately 15 minutes of soft tissue manipulation (massage) to the right shoulder musculature, with emphasis on the supraspinatus and deltoid. This was followed by approximately 10-20 minutes of cross fiber work to the distal tendon of the supraspinatus, as well as to the distal tendons of the infraspinatus and teres minor. The right shoulder joint was then mobilized and approximately 15 minutes was spent working the patient’s/client’s upper thoracic region and the musculature of the left shoulder. The therapist ended the session by icing the distal tendon and belly of the supraspinatus.
For self-care, the therapist recommended that Bill stop playing hockey and avoid all strong exertions with his right upper extremity. To keep the right shoulder moving, the therapist recommended that Bill perform the wall stretch. Bill was instructed to stand away from the wall and place his fingers on the wall. He then gradually “walked” his fingers up the wall or up and out to the side on the wall, going as high as he could. Over time, as he progressed, he could gradually stand closer to the wall. Bill was told that it would be helpful for him to mark in pencil how high he reached with the date that mark was reached, with a goal of gradually increasing the excursion of his movement each day or so. It was also recommended that Bill ice the shoulder every night.
At the end of three weeks, Bill’s symptoms had abated approximately 70%. Care was continued at once per week for another four weeks, with stretching of the rotator cuff muscles added to the session, to remedy the remaining symptoms. For proactive self-care, Bill continues to receive clinical orthopedic manual therapy once or twice each month, and has begun a strengthening program at the gym to build up the musculature of his shoulder joint before beginning hockey again.