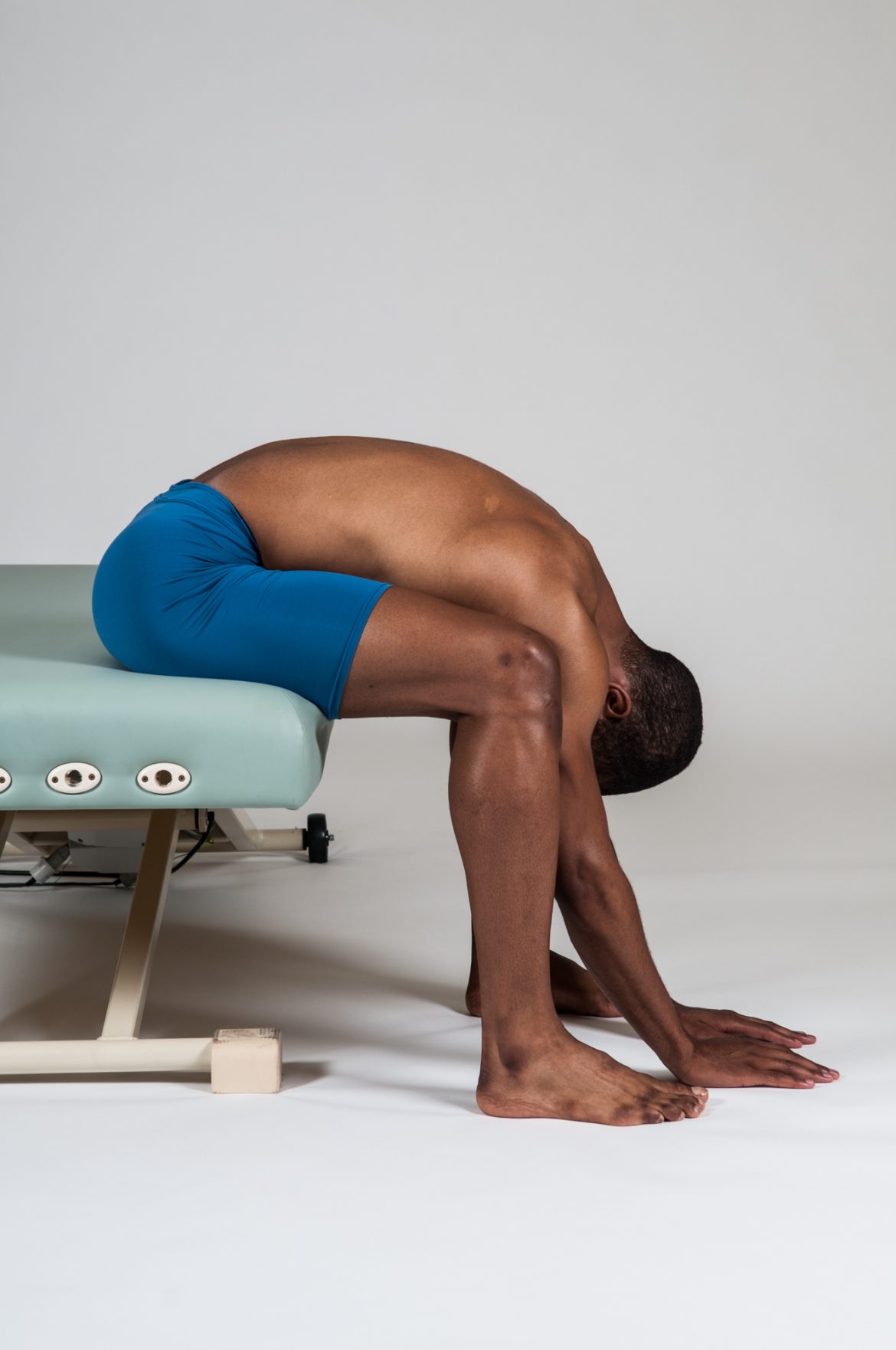
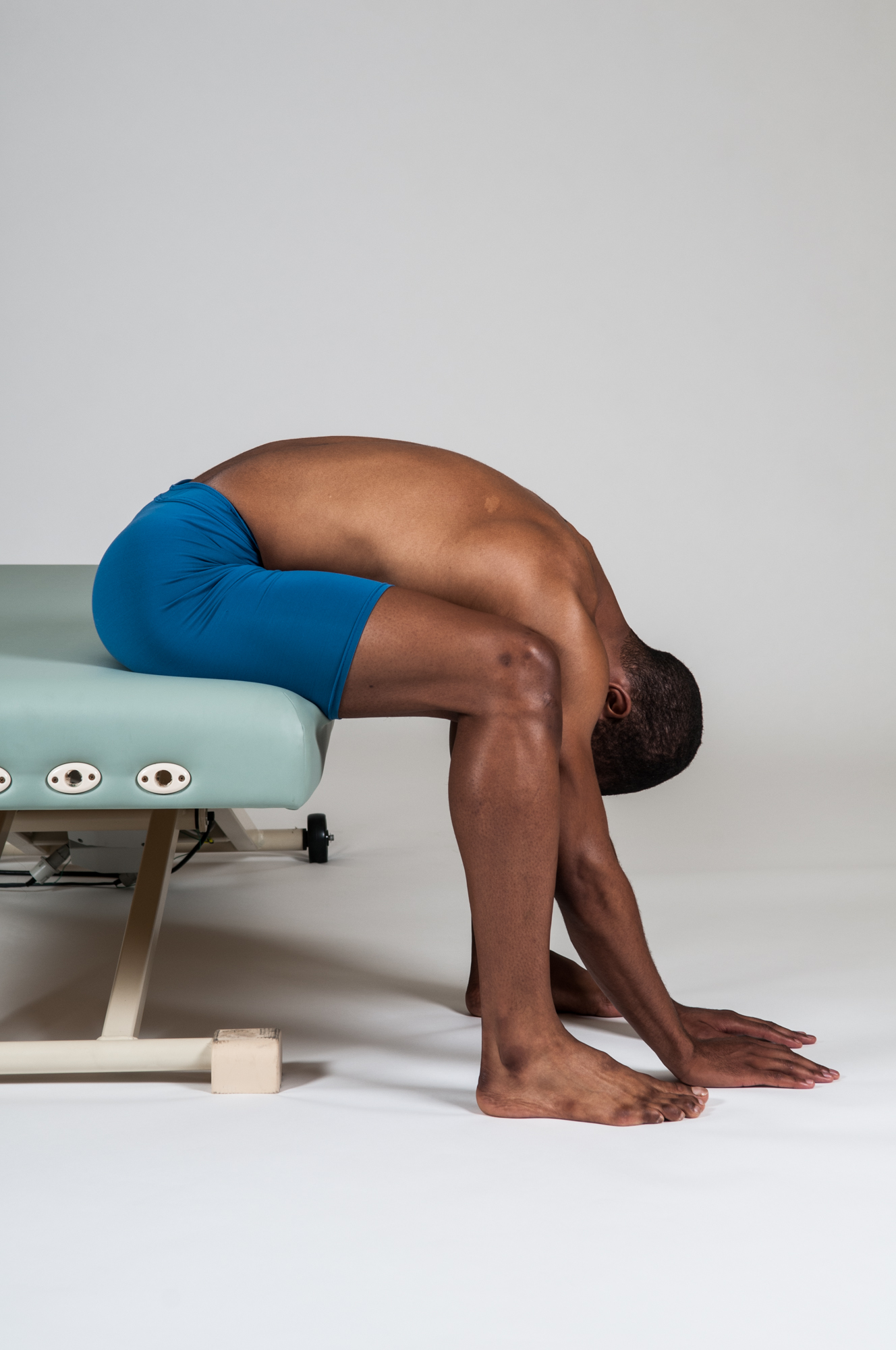
Self-care for the client/patient with lower crossed syndrome:
When working with a client/patient for the treatment of lower crossed syndrome, the importance of client self-care is critical. First, the client must be advised to avoid collapsing into the lower crossed rounded posture as much as possible. However, given the initial weakness of the anterior abdominal wall and posterior gluteal musculature with which they will present, it is important to explain to them that improving their posture will take time and patience. Therefore, they should not expect to suddenly sit and stand totally upright. Rather, it will be a gradual transition from their present posture to “ideal” posture as the tight/facilitated muscle groups are gradually loosened and the weak/inhibited muscle groups are gradually strengthened.
A good postural habit to recommend from the beginning is to ask the client to think about engaging the anterior abdominal wall to pull the belly button up and in toward the spine. Performing this exercise frequently throughout the day will begin the strengthening of the anterior abdominal wall and posterior gluteal muscles, and will also give them proprioceptive feedback about what it feels like to attain a more posteriorly tilted posture, in other words, a neutral pelvic posture. Another good posterior tilt exercise is to ask the client to lie supine on a mat (or carpeted floor), place a hand under the small of their back, and then flatten their back down against their hand and the floor.
Next, be sure to discuss with the client all the scenarios in which they might be collapsing into the lower crossed posture. These might include sitting posture at a computer, driving a car, or simply standing.
It is also important to recommend moist heat followed by stretching of the low back and hip flexor musculature. An effective stretch for the low back extensors is the double knee to chest stretch. Another effective self-care stretch for the low back can be performed while sitting at a chair (“seated low back stretch”). The client stabilizes their lower body by placing their feet flat on the floor. They then slowly flex their trunk down toward the floor until they are gently hanging downward. When returning upright, it is important to help their spinal extensor musculature by using their arms to push up and off their thighs. Performing a lunge stretch is an effective way to stretch the hip flexors. With the standing lunge stretch, be sure to advise to the client to avoid bending the forward knee so much that it is anterior to the toes of the foot; if this occurs, advise the client to simply move the forward foot a little more anteriorly. Performing the lunge stretch with the leg in back kneeling on the floor is easier for balance and stability, but because the knee joint tends to be in more flexion, this position preferentially stretches the rectus femoris muscle (and therefore not stretching the other hip flexors). For comfort, placing a pad or cushion under the knee is helpful. Because lower crossed syndrome often results in tight hamstrings, recommending a hamstring stretch is also wise.
Finally, self-care exercises for strengthening are just as important as the moist heat and stretching component. Strengthening should be directed at the inhibited weaker musculature listed in Table 1. Following are the two primary objectives of the strengthening program: 1. Flexion exercises aimed at the anterior abdominal wall; curl-ups/crunches can be used to accomplish this. 2. Strengthening the gluteus maximus and other posterior gluteal musculature; extension of the thigh against gravity with the knee joint flexed to 90 degrees is one effective exercise to accomplish this. Certainly, Pilates is an excellent method of body conditioning for all postural distortion patterns, including lower crossed syndrome.
Medical approach for lower crossed syndrome:
Lower crossed syndrome is a postural dysfunction pattern. As such, there really is no “medical” approach. Typically, if a medical doctor addresses this condition, it would be to refer the patient to physical therapy. Physical therapy would likely work with the patient with the same objectives of stretching and strengthening the musculature advocated here; moist heat and manual therapy might also be done. In addition, physical therapy modalities such as ultrasound and electrical muscle stimulation might also be performed for the facilitated/tight musculature.