Self-care for the client/patient:
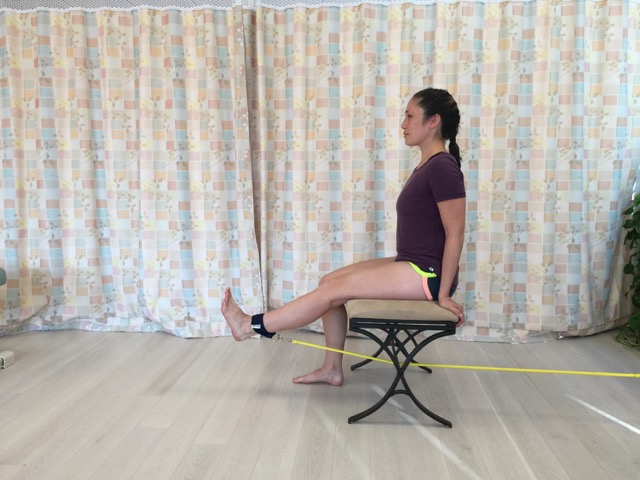
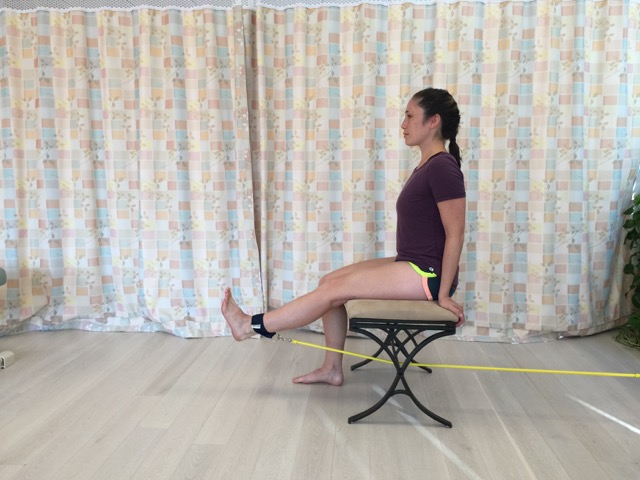
Resistance exercise using elastic tubing (Thera-ciser by Foot Levelers™). Permission: Joseph E. Muscolino.
Perhaps the one most important aspect of self-care for patellofemoral syndrome (PFS) is to strengthen the quadriceps femoris musculature. But it is important to slowly incrementally build up the resistance of the quadriceps exercise so that excessive stress is not suddenly placed on the patellofemoral joint. Self-care for the client/patient is to decrease postures and activities that add stress to the patellofemoral joint, including losing weight if the client/patient is overweight. Heat and stretching of the hip joint adductors and medial rotators is often helpful, as is strengthening the hip joint abductors and lateral rotators.
Medical approach:
The first step in the medical hierarchy for PFS is usually physical therapy. Strengthening the weak musculature that is contributing to PFS is most often the goal of physical therapy. If it is found that there is an imbalance between the vastus lateralis and vastus medialis, then strengthening the vastus medialis is often an exercise goal. However, there is controversy over whether or not exercise can be targeted toward only the fibers of the vastus medialis. If physical therapy does not work, the next step is usually non-steroidal anti-inflammatory (NSAID) medication. If this is not successful, then oral prednisone is given or a cortisone injection is usually done. If these are not effective, arthroscopic surgery to scrape the underside of the patella is usually done and quite effective with minimal recovery time needed. However, it is important for the client to realize that this surgery cannot be repeated multiple times, so it is important for them to remove whatever causes contributed to the PFS in the first place. If dysfunctional lateral patellar tracking is present, a surgical procedure called a lateral release is often done: the goal being to release the tension of the retinacular fibers of the quadriceps femoris proximal and lateral to the patella.
Manual therapy case study:
Heidi is a 42-year-old office worker who went to a massage therapist for a full body massage. During the history, she mentioned to the therapist that she has been experiencing mild left knee pain over the past few months. The pain is dull in quality and feels deep in the joint; she especially notices the pain when walking downstairs.
During static postural assessment, the therapist noticed that Heidi’s left iliac crest is mildly/moderately low, her left knee has a slightly increased genu valgus angle, and her left foot slightly overpronates. Palpation assessment revealed tight tensor fasciae latae and adductors on her left side, as well as myofascial trigger points in her left quadriceps femoris, gluteus medius, and deep lateral rotators. Manual resistance to Heidi’s hip joint abductors and lateral rotators showed them to be weak and moderate discomfort was experienced when resistance was given. PFS test was positive; mild crepitus was present and pain was experienced.
Given the assessment of PFS, the therapist recommended two one-hour massages per week for three weeks and one one-hour massage per week for the following five weeks. The therapist also recommended that Heidi go to either a fitness trainer or a Pilates instructor to strengthen her hip abductors and lateral rotators, and the muscles that support her arch, as well as her quadriceps femoris and general conditioning.
With the client/patient supine, moderate to deep soft tissue manipulation was performed for the left-sided quadriceps femoris for 5-10 minutes. Heat was then placed on the quadriceps while deep tissue work was done to the retinacular fibers around the patella and then gentle joint mobilization (arthrofascial stretching) was performed for the patella. Deep tissue manipulation was then done on the left tensor fasciae latae and adductor group. Heidi was then placed in side-lying position to work the myofascial trigger points in her left gluteus medius and minimus, and then prone position to work the myofascial trigger points in her left deep lateral rotators. The quadriceps, tensor fasciae latae, and adductors were then stretched.
Each session was carried out in a similar manner, with increasing depth of pressure and assertiveness of stretching as Heidi gradually improved. Heidi was given self-care stretches for the hip adductors and tensor fasciae latae; and she was told to perform these stretches two to three times per day after hot shower or other form of moist heat application. Finally, the possibility of wearing shoes that have good arch support was discussed.
At the end of eight weeks, Heidi’s knee pain was improved 50% and her genu valgus showed the beginning of improvement. For proactive self-care with the goal of continuing to improve her genu valgus and PFS, Heidi continues to receive clinical orthopedic massage once or twice each month and continues to work out once per week with an instructor and twice per week at home on her own.