Understanding structural fundamentals prevents catastrophic failures, protects members, and preserves the integrity of your facility.
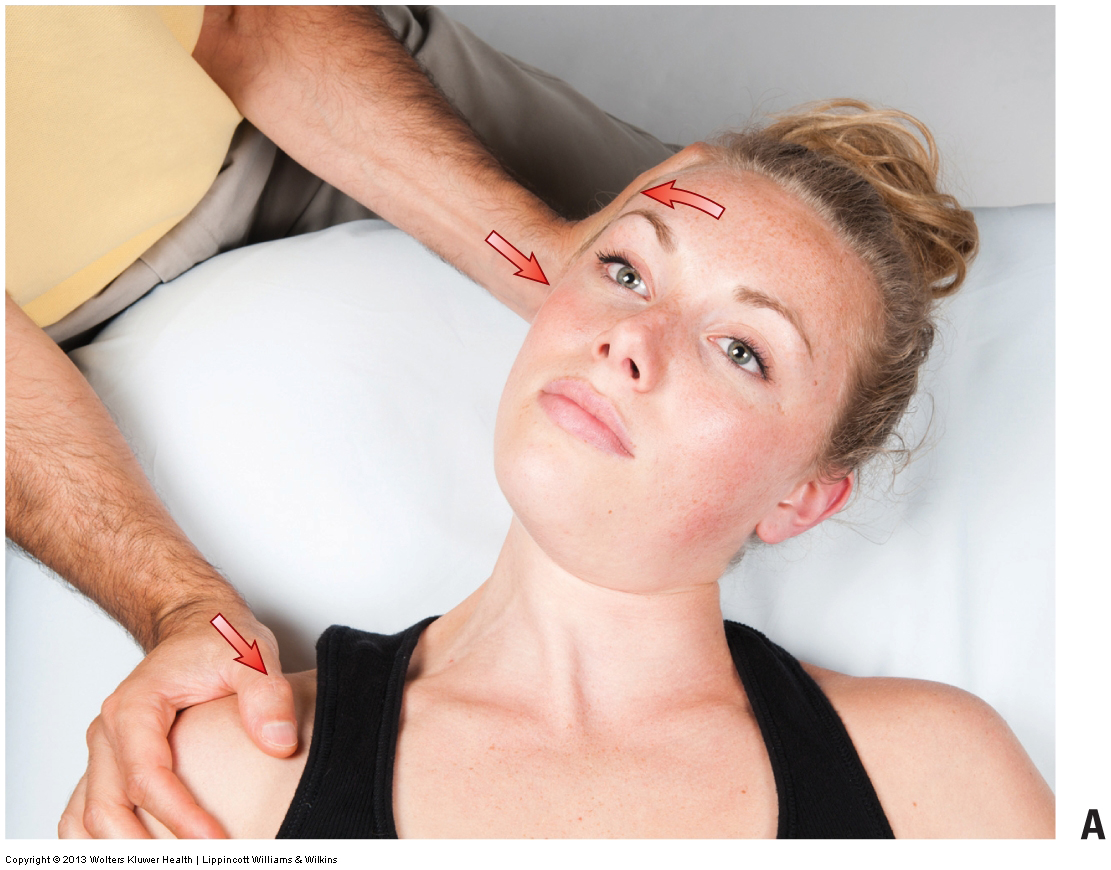
The Cross-Over Effect of Stretching
Results showed that there were significant shoulder joint ROM increases following both lower body static stretching and lower body dynamic stretching.
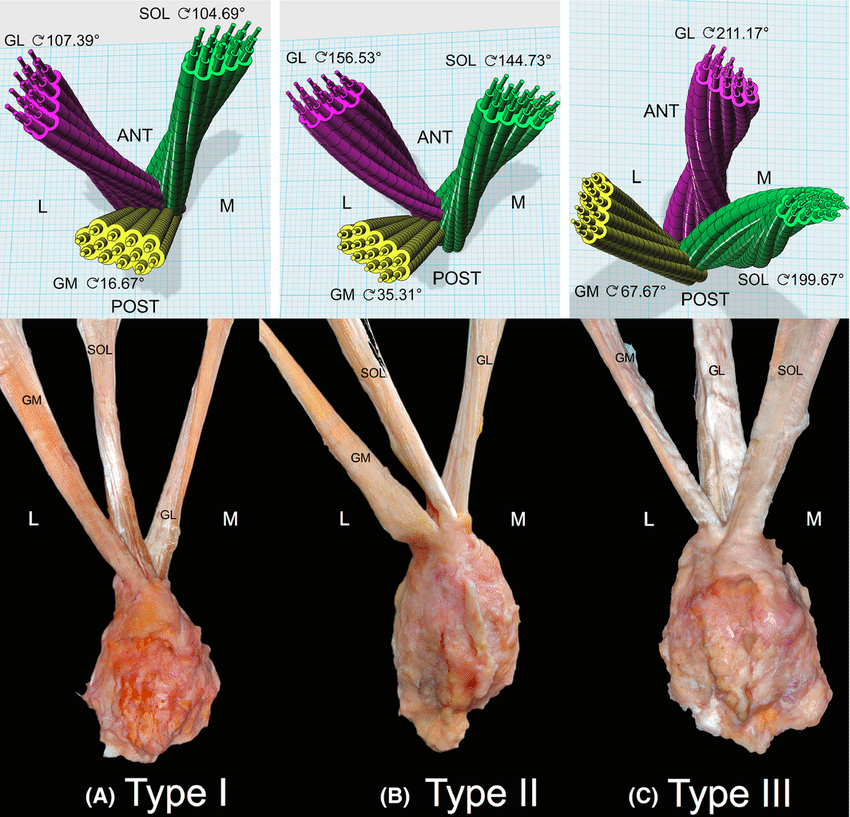
The Twisted Structure of the Achilles Tendon
A study from Belgium also showed that the Achilles tendon displayed a twisted structure, with the greatest twisting found in the deep (anterior) layer of the tendon (lateral gastrocnemius and soleus).
How to Make Dental Visits Fun for Kids
Visiting the dentist does not need to be a scary experience; it can be fun, exciting, and even something that the kids may enjoy.
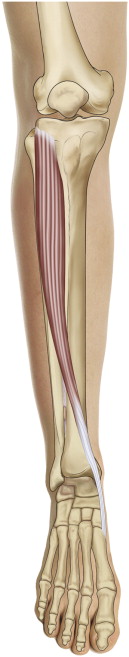
What is shin splints and what are it causes?
The term shin splints is a lay term that usually refers to a periostitis (inflammation of the periosteal lining) of the tibia.
Emerging Trends in Men’s Health and Wellness Today
Let’s explore the top male health progression trends that promote a healthy lifestyle.
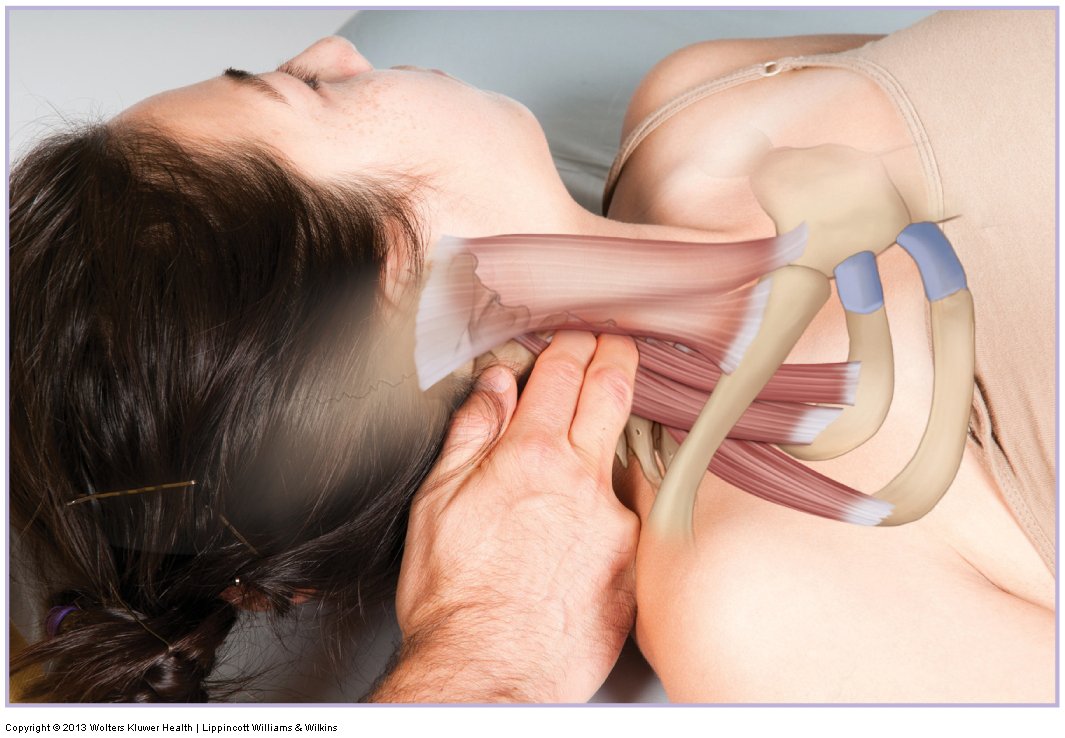
Advanced Stretching Techniques
Advanced stretching technique include pin and stretch technique as well as neural inhibition techniques (CR, AC, PIR, PNF) that relax / inhibit musculature.
From Bodywork to Bedside: A Guide to Transitioning into a Nursing Career
Thinking of becoming a nurse? Learn how to shift from bodywork to bedside with practical steps, training tips, and mindset advice for the journey.
How Chiropractic Care Can Boost Your Performance and Help Prevent Injury?
If you take your fitness seriously, you already know the importance of chiropractic care. It is essential if you want to perform at the optimum level.
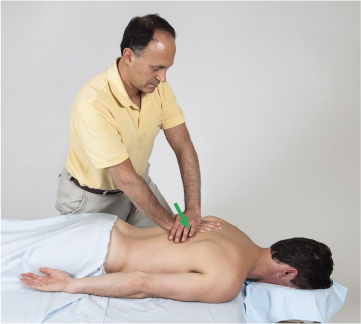
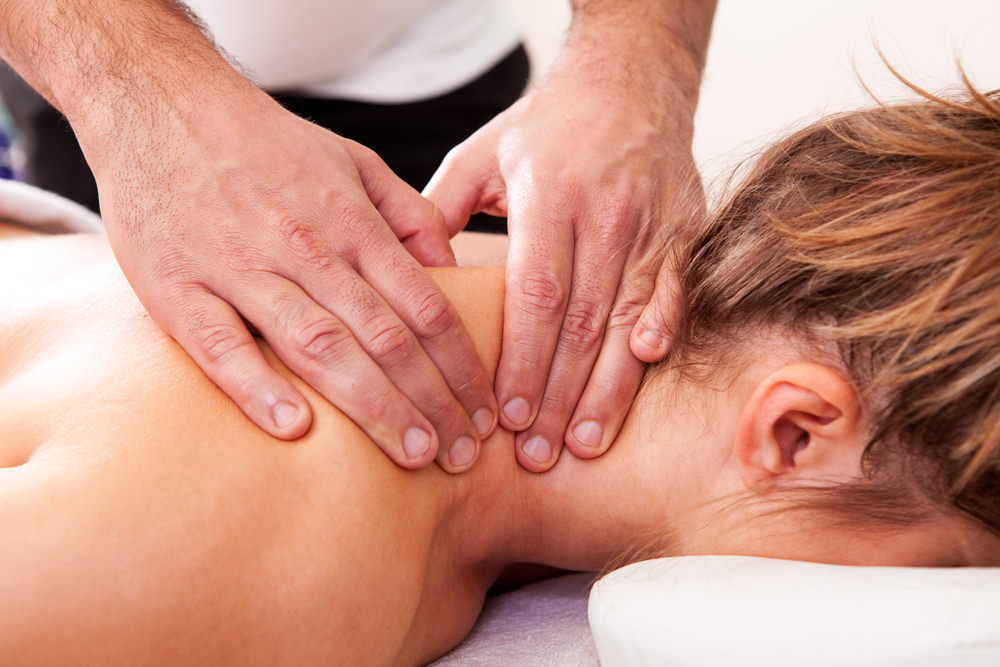
How Do We Treat Slumped Spinal Posture with Manual Therapy?
When performing soft tissue manipulation/massage, it is always wise to begin with light to medium pressure, and then transition to deeper pressure.
Not Just Tech—A Better Experience: AI in Dental Front Desks
AI is here to stay—but the way it’s being used in dental clinics like yours is anything but dehumanizing. It’s enhancing the heart of the practice: the patient experience.
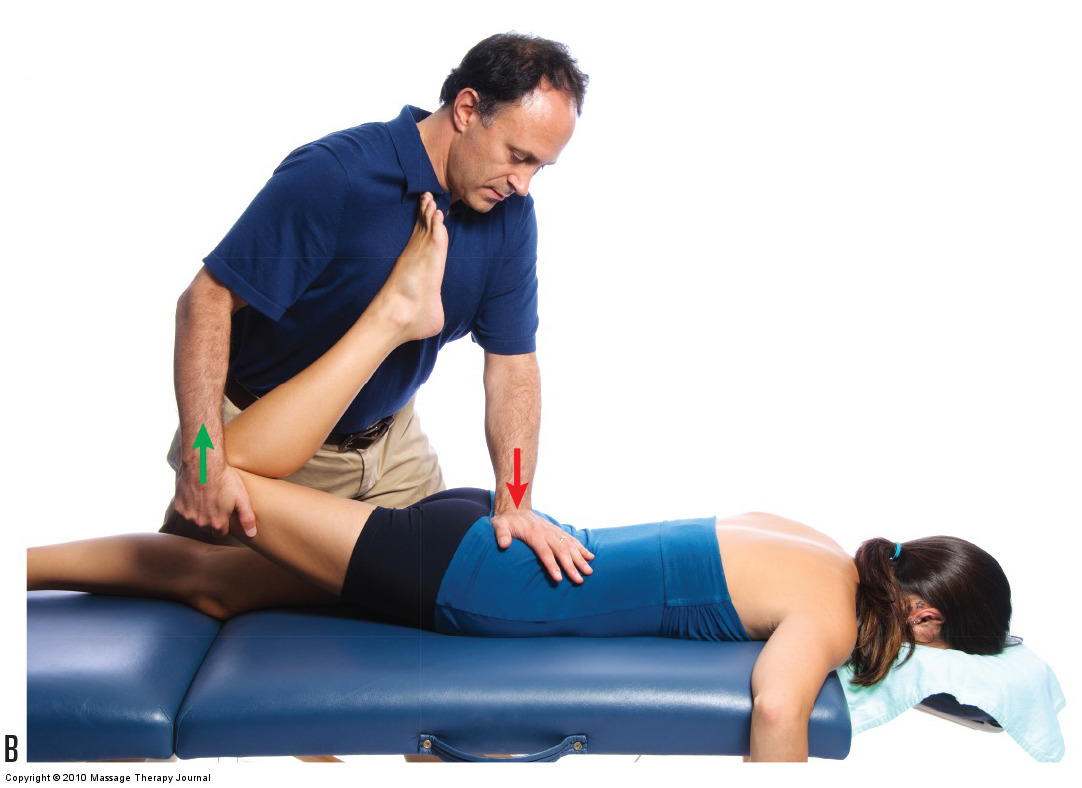
Nachlas and Yeoman’s Special Orthopedic AssessmentTests
This blog post article is part of a series of articles on assessment of the low back and pelvis. Scroll to the end of this article to see the others in this series. Nachlas and Yeoman’s Tests Nachlas’ test and …
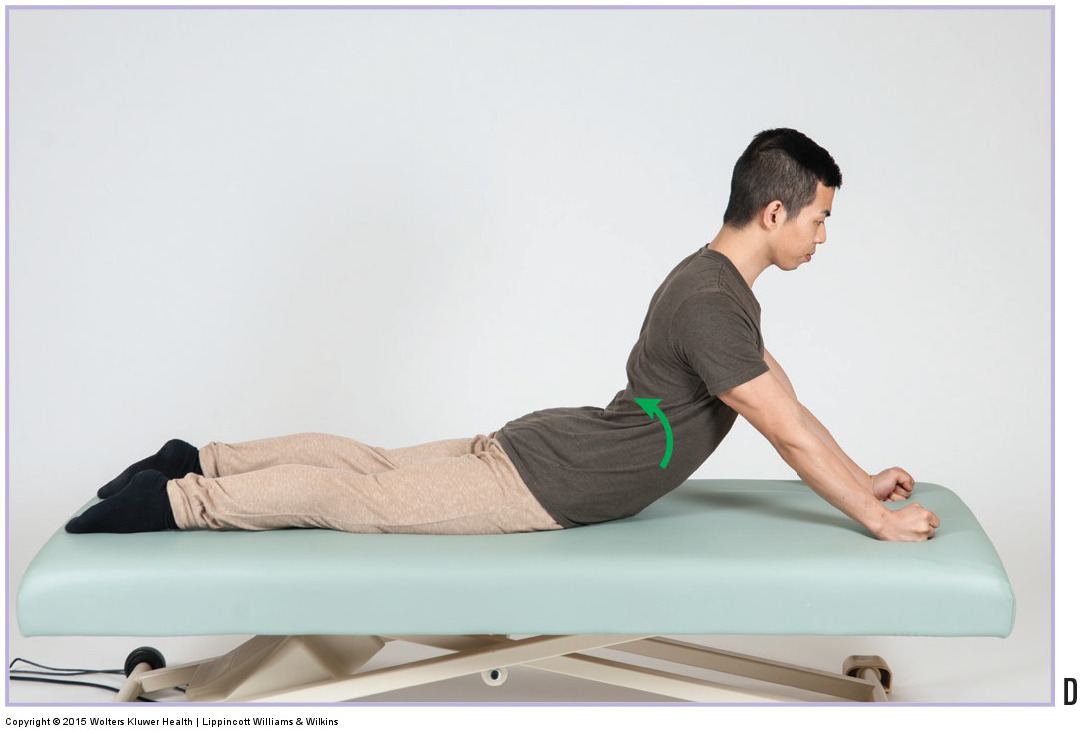
Back Extension McKenzie Exercises Effect on Disc Fluid
The authors concluded that little evidence was found supporting the hypothesis that extension McKenzie exercises affect disc fluid content.
Choosing a Quality Cannabis Dispensary in Los Angeles for Your Health
Whether you’re using cannabis for chronic pain, stress relief, or general wellness, prioritizing your health is essential.
Manual Therapy Certification for Chiropractors
What is most important in any Manual Therapy Certification program is marrying together the underlying science with the hands-on manual therapy skills.
The Science of Post-Exercise Massage
These evidence-based studies explain the physiology and suggest that post-exercise massage reduces tissue damage and accelerates muscle recovery.
Effective Ringworm Treatment Available Online
Even though a ringworm infection sounds horrible, it is a relatively common and non-lethal fungal infection.
What Causes Silent Migraines? Know the Triggers
By learning about the causes of silent migraines and their triggers, one can work to treat or prevent these episodes from occurring.
Guide to Using Welding Fume Extraction Arms
When you know their benefits and how to apply them, industries can protect their workforce and improve productivity.
How Compression Socks Support Circulation During Long Days on the Feet
With their ability to boost blood flow, reduce fatigue, and improve foot health, compression socks provide both immediate comfort and long-term benefits.
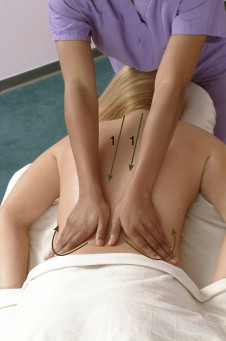
Self-care and medical approaches to tight spasmed muscles in the low back
Self-care for the client/patient with low back muscle spasm should include moist heat followed by stretching. Double knee to chest stretch is beneficial.
Essential Tools for Managing Respiratory Health
Having the right respiratory tools and knowing how to use them properly can transform your daily life and give you confidence to handle breathing challenges effectively.
7 Osteopathic Concepts Every Manual Therapist Should Understand
Understanding these concepts can transform the way you think and work. Mastery of the hands begins with mastery of these foundational ideas.
Real-World Massage Therapy is Effective for Treating Lower Back Pain
After 12 weeks, more than half of the patients reported improved outcomes in terms of pain reduction, and meaningful physical and mental improvement.
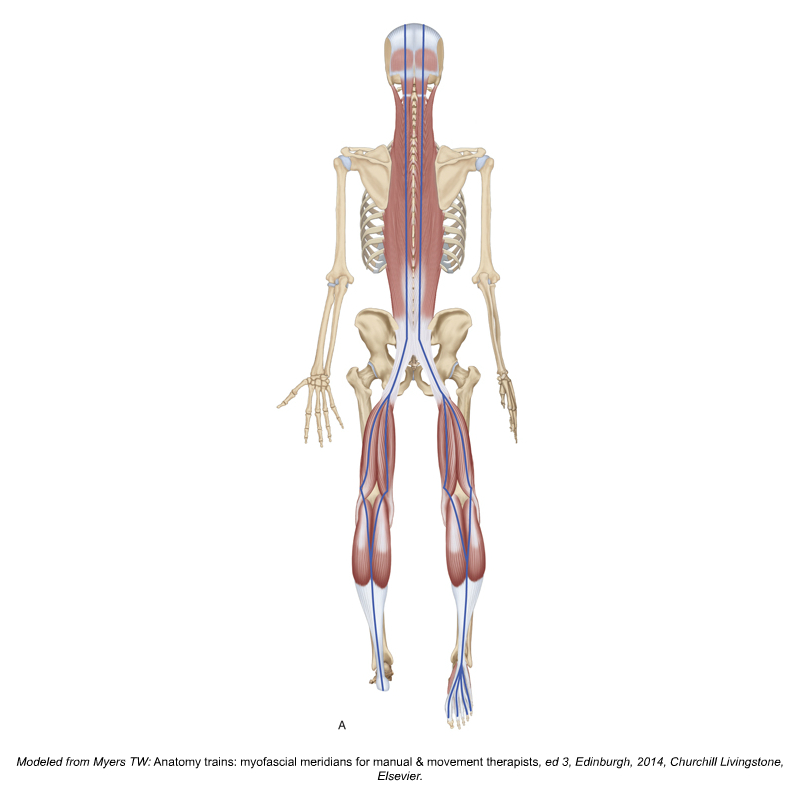
Massage of the Plantar Fascia Increases Hamstring Flexibility
This study found that remote stretching via self-myofascial release using foam roller massage of the plantar fascia does increase hamstring extensibility.
Health and Fitness Videos: How to get better YouTube Engagement
By focusing on essential techniques like tightening your hook, eliminating distractions, and highlighting key moments, you can create content that holds viewers’ attention.
What Are Peptides? A Beginner’s Guide to Their Role in the Body
As scientists learn more about how different peptides function, new breakthroughs are expected to emerge in medicine and everyday wellness.
The Effect of Stretching on Flexibility and Joint Range of Motion
All types of stretching showed joint range of motion improvements over the long term, however, static stretching technique showed the greatest improvement.
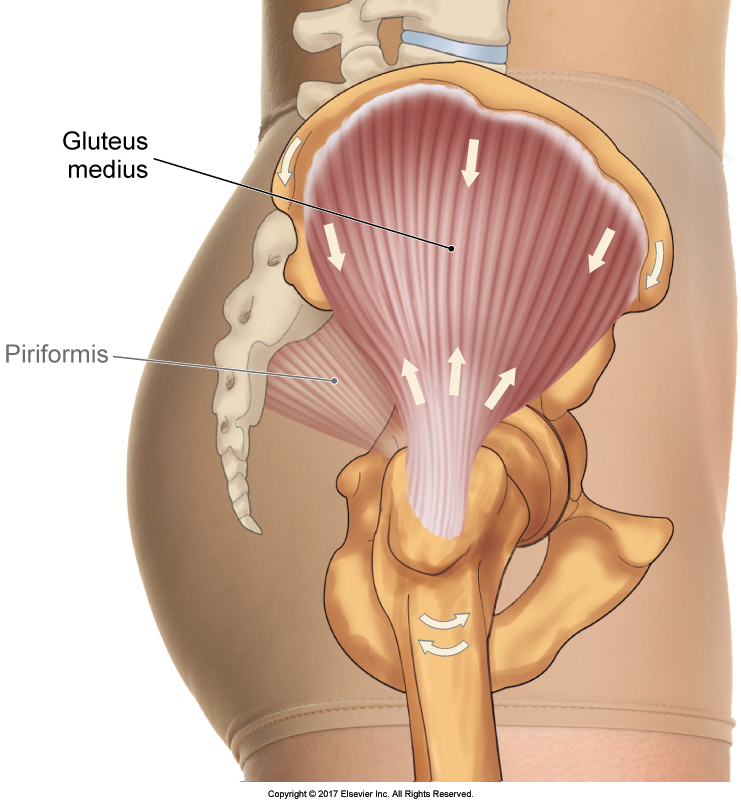
Clinical Tests for Gluteal Tendinopathy in Patients with Lateral Hip Pain
Patients with lateral hip pain on Single Leg Stance and who are not palpably tender over the greater trochanter are unlikely to have gluteal tendinopathy.
Top 7 Tips for Choosing the Perfect Glasses Online
Choosing the perfect glasses is about more than clear eyesight; it’s also about boosting your confidence, comfort, and personal style.